Microscope-assisted coronary artery bypass grafting in diffuse coronary artery disease: immediate and mid-term results
Published 2023-09-29
Keywords
- Coronary Artery Bypass,
- Coronary Artery Disease,
- Microsurgery,
- Plaque, Atherosclerotic,
- Retrospective Studies
How to Cite
Copyright (c) 2023 Semchenko A.N., Shevchenko A.M., Zaicev I.V., Semchenko A.V., Vnukova T.B.

This work is licensed under a Creative Commons Attribution 4.0 International License.
Abstract
Background: In recent years, a typical candidate for coronary artery bypass grafting (CABG) has become a patient with complex, multivessel coronary artery disease (CAD), often with an unsatisfactory and small distal bed. The prevalence of diffuse CAD is 4.2%-46.0%, and the CABG refusal rate due to this disease accounts for 1.3%-15.0%. Diffuse CAD is an independent predictor of mortality and poor prognosis after CABG. Due to a lack of uniform criteria for diffuse CAD and randomized trials, there is no preferred surgical treatment option for such patients.
Objective: To evaluate immediate and mid-term results of microscope-assisted CABG in patients with ischemic heart disease and diffuse CAD.
Methods: We calculated a diffuseness score and determined whether the criterion of diffuse lesion by SYNTAX score was met. For our retrospective study we selected 187 ischemic heart disease patients with 3-vessel CAD who underwent microscope-assisted CABG. A coronary lesion with a diffuseness score of >18 was considered diffuse if the SYNTAX score criterion was met for each of the main coronary arteries. The patients were divided into 2 groups: group 1 for patients with diffuse CAD (n = 60) and group 2 for patients with CAD that did not meet the criterion to be considered diffused (n = 127). The propensity score matching was used to reduce differences between the groups. The primary end point was death from any cause; the secondary end points were adverse cardiovascular events (death from cardiac causes, myocardial infarction, repeated revascularization, acute cerebrovascular accident) and angina.
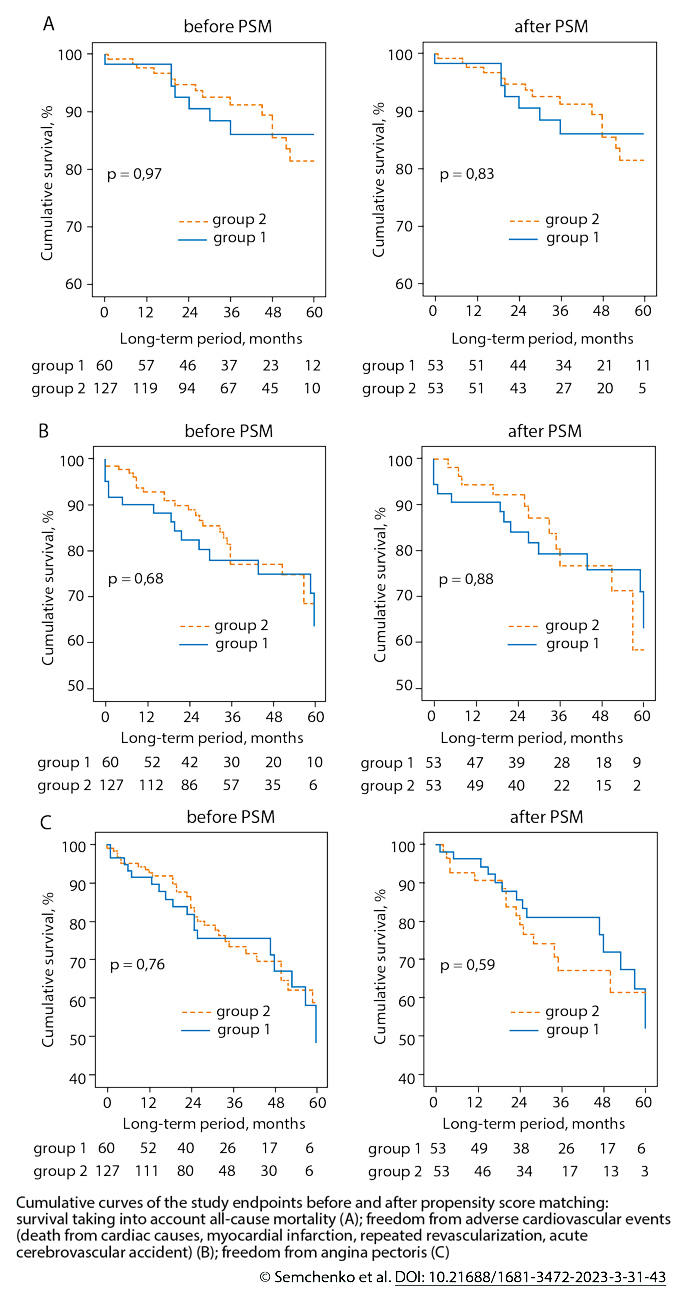
Results: No significant differences in the frequency of in-hospital specific and nonspecific complications were found. The frequency of achieved complete revascularization was comparable between the groups. There were no significant differences in the long-term survival, adverse cardiovascular events, and freedom from angina during the median follow-up of 39 months (min 1 month; max 60 months). The univariate analysis after the propensity score matching showed that diffuse CAD was not a significant predictor of death from any cause [hazard ratio (HR), 1.141; 95% CI, 0.348-3.742; P = .83], adverse cardiovascular events [HR, 0.940; 95% CI, 0.425-2.078; P = .88], and angina [HR, 0.817; 95% CI, 0.394-1.696; P = .59]. The multivariate analysis revealed no significant association between diffuse CAD and death from any cause both before [HR, 1.382; 95% CI, 0.396-4.815; P = .61] and after propensity score matching [HR, 2.079; 95% CI, 0.158-27.422; P = .58]. We found that within 60 months after CABG, the risk of death from any cause was increased: by patient’s age [HR, 1.166; 95% CI, 1.043-1.303; P = .007], male sex [HR, 5.583; 95% CI, 1.062-29.344; P = .042], and diabetes mellitus [HR, 3.673; 95% CI, 1.143-11.805; P = .029] before the propensity score matching and by patient’s age [HR, 2.055; 95% CI, 1.028-4.104; P = .041] and cardiopulmonary bypass time [HR, 1.190; 95% CI, 1.014-1.397; P = .033] after the propensity score matching.
Conclusion: Microscope-assisted CABG in patients with diffuse CAD can achieve satisfactory immediate and mid-term results. We found no association between diffuse CAD and the risk of adverse events.
Received 30 January 2023. Revised 29 June 2023. Accepted 5 July 2023.
Funding: The study did not have sponsorship.
Conflict of interest: The authors declare no conflict of interest.
Contribution of the authors
Conception and study design: A.N. Semchenko
Data collection and analysis: A.M. Shevchenko, I.V. Zaicev, A.V. Semchenko, T.B. Vnukova
Statistical analysis: A.N. Semchenko
Drafting the article: A.N. Semchenko, I.V. Zaicev
Critical revision of the article: A.M. Shevchenko, A.V. Semchenko, T.B. Vnukova
Final approval of the version to be published: A.N. Semchenko, A.M. Shevchenko, I.V. Zaicev, A.V. Semchenko, T.B. Vnukova
References
- da Rocha A.S.C., Dassa N.P.R., Pittella F.J.M., Barbosa O.N., Brito J.O.R., Tura B., da Silva P.R.D. High mortality associated with precluded coronary artery bypass surgery caused by severe distal coronary artery disease. Circulation. 2005;112(9 Suppl):I328-I331. PMID: 16159841. https://doi.org/10.1161/CIRCULATIONAHA.104.525717
- Чарчян Э.Р., Ховрин В.В., Скворцов А.А., Пюмпюлян А.Г. Коронарное шунтирование передней межжелудочковой артерии при ее диффузном атеросклеротическом поражении. Коронарная эндартерэктомия или шунт-пластика? Кардиология и сердечно-сосудистая хирургия. 2018;11(6):14-20. https://doi.org/10.17116/kardio20181106114 Charchyan E.R., Khovrin V.V., Skvortsov A.A., Pyumpyulyan A.G. Coronary artery bypass grafting of the diffusely diseased left anterior descending artery. Coronary endarterectomy or patch angioplasty? Kardiologiya i serdechno-sosudistaya khirurgiya = Russian Journal of Cardiology and Cardiovascular Surgery. 2018;11(6):14‑20. (In Russ.) https://doi.org/10.17116/kardio20181106114
- Курбанов С.К., Власова Э.Е., Саличкин Д.В., Майоров Г.Б., Галяутдинов Д.М., Васильев В.П., Ширяев А.А., Акчурин Р.С. Госпитальные и годичные результаты коронарного шунтирования при диффузном поражении коронарных артерий. Кардиологический вестник. 2019;14(1):60‑66. https://doi.org/10.17116/Cardiobulletin20191401160 Kurbanov S.K., Vlasova E.E., Salichkin D.V., Mayorov G.B., Galayutdinov D.M., Vasiliev V.P., Shiryaev A.A., Akchurin R.S. In-hospital and one-year outcomes after coronary artery bypass grafting in patients with diffuse coronary artery disease. Russian Cardiology Bulletin. 2019;14(1):60‑66. (In Russ.) https://doi.org/10.17116/Cardiobulletin20191401160
- Brown R.A., Shantsila E., Varma C., Lip G.Y.H. Epidemiology and pathogenesis of diffuse obstructive coronary artery disease: the role of arterial stiffness, shear stress, monocyte subsets and circulating microparticles. Ann Med. 2016;48(6):444-455. PMID: 27282244. https://doi.org/10.1080/07853890.2016.1190861
- Акчурин Р.С., Ширяев А.А., Андреев А.В., Васильев В.П., Галяутдинов Д.М., Зайковский В.Ю., Мукимов Ш.Д. Коронарное шунтирование при диффузном поражении коронарных артерий: использование аутоартериальных трансплантатов. Кардиологический вестник. 2021;16(4):5-10. https://doi.org/10.17116/Cardiobulletin2021160415 Akchurin R.S., Shiryaev A.A., Andreev A.V., Vasiliev V.P., Galyautdinov D.M., Zaykovskiy V.Yu., Mukimov Sh.D. Coronary artery bypass grafting for diffuse coronary atherosclerosis using autologous arterial grafts. Russian Cardiology Bulletin. 2021;16(4):5-10. (In Russ.) https://doi.org/10.17116/Cardiobulletin2021160415
- Henry T.D., Satran D., Hodges J.S., Johnson R.K., Poulose A.K., Campbell A.R., Garberich R.F., Bart B.A., Olson R.E., Boisjolie C.R., Harvey K.L., Arndt T.L., Traverse J.H. Long-term survival in patients with refractory angina. Eur Heart J. 2013;34(34):2683-2688. PMID: 23671156. https://doi.org/10.1093/eurheartj/eht165
- Graham M.M., Chambers R.J., Davies R.F. Angiographic quantification of diffuse coronary artery disease: reliability and prognostic value for bypass operations. J Thorac Cardiovasc Surg. 1999;118(4):618-627. PMID: 10504625. https://doi.org/10.1016/S0022-5223(99)70006-1
- McNeil M., Buth K., Brydie A., MacLaren A., Baskett R. The impact of diffuseness of coronary artery disease on the outcomes of patients undergoing primary and reoperative coronary artery bypass grafting. Eur J Cardiothorac Surg. 2007;31(5):827-833. PMID: 17346985. https://doi.org/10.1016/j.ejcts.2006.12.033
- Ширяев А.А., Акчурин Р.С., Васильев В.П., Галяутдинов Д.М., Власова Э.Е., Курбанов С.К., Зайковский В.Ю. Годовые результаты коронарного шунтирования у пациентов с диффузным поражением коронарных артерий. Кардиология и сердечно-сосудистая хирургия. 2021;14(5):413-419. https://doi.org/10.17116/kardio202114051413 Shiryaev A.A., Akchurin R.S., Vasiliev V.P., Galyautdinov D.M., Vlasova E.E., Kurbanov S.K., Zaikovskii V.Yu. Annual outcomes of coronary artery bypass grafting in patients with diffuse lesion of coronary arteries. Kardiologiya i serdechno-sosudistaya khirurgiya = Russian Journal of Cardiology and Cardiovascular Surgery. 2021;14(5):413‑419. (In Russ.) https://doi.org/10.17116/kardio202114051413
- Fukui T., Tabata M., Taguri M., Manabe S., Morita S., Takanashi S. Extensive reconstruction of the left anterior descending coronary artery with an internal thoracic artery graft. Ann Thorac Surg. 2011;91(2):445-451. PMID: 21256288. https://doi.org/10.1016/j.athoracsur.2010.10.002
- Jalal A. An objective method for grading of distal disease in the grafted coronary arteries. Interact Cardiovasc Thorac Surg. 2007;6(4):451-455. PMID: 17669896. https://doi.org/10.1510/icvts.2007.156273
- Акчурин Р.С., Ширяев А.А., Васильев В.П., Галяутдинов Д.М., Власова Э.Е., Курбанов С.К. Диффузное поражение коронарных артерий в коронарной хирургии (аналитический обзор). Клиническая и экспериментальная хирургия. Журнал имени академика Б.В. Петровского. 2018;6(4):75-81. https://doi.org/10.24411/2308-1198-2018-14011 Akchurin R.S., Shiryaev A.A., Vasiliev V.P., Galyautdinov D.M., Vlasova E.E., Kurbanov S.K. Diffuse coronary artery disease in coronary surgery (analytical review). Clinical and Experimental Surgery. Petrovsky Journal. 2018;6(4):75-81. (In Russ.) https://doi.org/10.24411/2308-1198-2018-14011
- Альсов С.А., Осипов Д.Е., Акчурин Р.С., Ширяев А.А., Сирота Д.А., Хван Д.С., Чернявский А.М., Цирихов В.Р. Микрохирургия коронарных артерий с использованием операционного микроскопа. Хирургия. Журнал им. Н.И. Пирогова. 2019;1:60-64. https://doi.org/10.17116/hirurgia201901160 Alsov S.A., Osipov D.E., Akchurin R.S., Shiryaev A.A., Sirota D.A., Khvan D.S., Chernyavskiy A.M., Tsirikhov V.R. Microsurgery of coronary arteries using an operating microscope. Khirurgiya. Zhurnal im. N.I. Pirogova = Pirogov Journal of Surgery. 2019;1:60-64. (In Russ.) https://doi.org/10.17116/hirurgia201901160
- Семченко А.Н. Микрохирургическая техника в коронарной хирургии: возможности, перспективы и ограничения. Хирургия. Журнал им. Н.И. Пирогова. 2019;6:80-87. https://doi.org/10.17116/hirurgia201906180 Semchenko A.N. Microsurgical technique in coronary bypass surgery: possibilities, perspectives and limitations. Khirurgiya. Zhurnal im. N.I. Pirogova = Pirogov Journal of Surgery. 2019;6:80-87. (In Russ.) https://doi.org/10.17116/hirurgia201906180
- Sianos G., Morel M.-A., Kappetein A.P., Morice M.-C., Colombo A., Dawkins K., van den Brand M., Van Dyck N., Russell M.E., Mohr F.W., Serruys P.W. The SYNTAX Score: an angiographic tool grading the complexity of coronary artery disease. EuroIntervention. 2005;1(2):219-227. PMID: 19758907.
- Bernstein S.J., Brorsson B., Aberg T., Emanuelsson H., Brook R.H., Werkö L. Appropriateness of referral of coronary angiography patients in Sweden. SECOR/SBU Project Group. Heart. 1999;81(5):470-477. PMID: 10212163; PMCID: PMC1729044. https://doi.org/10.1136/hrt.81.5.470
- Mukherjee D., Bhatt D.L., Roe M.T., Patel V., Ellis S.G. Direct myocardial revascularization and angiogenesis — how many patients might be eligible? Am J Cardiol. 1999;84(5):598-600. PMID: 10482164. https://doi.org/10.1016/s0002-9149(99)00387-2
- Lozano I., Capin E., de la Hera J.M., Llosa J.C., Carro A., López-Palop R. Diffuse coronary artery disease not amenable to revascularization: long-term prognosis. Rev Esp Cardiol (Engl Ed). 2015;68(7):631-633. PMID: 25936615. https://doi.org/10.1016/j.rec.2015.02.013
- Cavender M.A., Alexander K.P., Broderick S., Shaw L.K., McCants C.B., Kempf J., Ohman E.M. Long-term morbidity and mortality among medically managed patients with angina and multivessel coronary artery disease. Am Heart J. 2009;158(6):933-940. PMID: 19958859. https://doi.org/10.1016/j.ahj.2009.10.013
- Kandzari D.E., Lam L.C., Eisenstein E.L., Clapp-Channing N., Fine J.T., Califf R.M., Mark D.B., Jollis J.G. Advanced coronary artery disease: Appropriate end points for trials of novel therapies. Am Heart J. 2001;142(5):843-851. PMID: 11685173. https://doi.org/10.1067/mhj.2001.119136
- Dourado L.O.C., Bittencourt M.S., Pereira A.C., Poppi N.T., Dallan L.A.O., Krieger J.E., Cesar L.A.M., Gowdak L.H.W. Coronary artery bypass surgery in diffuse advanced coronary artery disease: 1-year clinical and angiographic results. Thorac Cardiovasc Surg. 2018;66(6):477-482. PMID: 28355655. https://doi.org/10.1055/s-0037-1601306
- Qiu Z., Auchoybur Merveesh L., Xu Y., Jiang Y., Wang L., Xu M., Xiang F., Chen X. The midterm results of coronary endarterectomy in patients with diffuse coronary artery disease. J Cardiothorac Surg. 2018;13(1):90. PMID: 30041678; PMCID: PMC6057028. https://doi.org/10.1186/s13019-018-0776-8
- Neumann F.-J., Sousa-Uva M., Ahlsson A., Alfonso F., Banning A.P., Benedetto U., Byrne R.A., Collet J.-P., Falk V., Head S.J., Jüni P., Kastrati A., Koller A., Kristensen S.D., Niebauer J., Richter D.J., Seferovic P.M., Sibbing D., Stefanini G.G., Windecker S., Yadav R., Zembala M.O.; ESC Scientific Document Group. 2018 ESC/EACTS Guidelines on myocardial revascularization. Eur Heart J. 2019;40(2):87-165. PMID: 30165437. https://doi.org/10.1093/eurheartj/ehy394
- Wang J., Gu C., Yu W., Gao M., Yu Y. Short- and long-term patient outcomes from combined coronary endarterectomy and coronary artery bypass grafting: a meta-analysis of 63,730 patients (PRISMA). Medicine (Baltimore). 2015;94(41):e1781. PMID: 26469920; PMCID: PMC4616783. https://doi.org/10.1097/MD.0000000000001781
- Soylu E., Harling L., Ashrafian H., Casula R., Kokotsakis J., Athanasiou T. Adjunct coronary endarterectomy increases myocardial infarction and early mortality after coronary artery bypass grafting: a meta-analysis. Interact Cardiovasc Thorac Surg. 2014;19(3):462-473. PMID: 24893867. https://doi.org/10.1093/icvts/ivu157
- Song Y., Xu F., Du J., Zhang J., Feng W. Coronary endarterectomy with coronary artery bypass graft decreases graft patency compared with isolated coronary artery bypass graft: a meta-analysis. Interact Cardiovasc Thorac Surg. 2017;25(1):30-36. PMID: 28329247. https://doi.org/10.1093/icvts/ivx045
- Zarrabi K., Dehghani P., Abdi Ardekani A., Zarrabi M.A., Zolghadrasli A. The comparison between two surgical methods for left internal mammary artery (LIMA) anastomosis on left anterior descending (LAD) artery in patients with severe diffuse lesions: short to mid-term results. Acta Med Iran. 2015;53(6):369-372. PMID: 26069175.
- Semchenko A., Makarov A., Karpov I., Zharenkov M. Microscope-assisted coronary artery bypass grafting: technique and results. Braz J Cardiovasc Surg. 2020;35(5):815-820. PMID: 33118747; PMCID: PMC7598973. https://doi.org/10.21470/1678-9741-2019-0416
- Семченко А.Н., Макаров А.Д. Микроскоп-ассистированное коронарное шунтирование: особенности выполнения анастомоза «бок-в-бок». Патология кровообращения и кардиохирургия. 2021;25(2):102-107. https://dx.doi.org/10.21688/1681-3472-2021-2-102-107 Semchenko A.N., Makarov A.D. Microscope-assisted coronary artery bypass grafting: features of creating side-to-side anastomosis. Patologiya krovoobrashcheniya i kardiokhirurgiya = Circulation Pathology and Cardiac Surgery. 2021;25(2):102-107. (In Russ.) https://dx.doi.org/10.21688/1681-3472-2021-2-102-107
- Tseng Y.-H., Kao C.-C., Lin C.-C., Lu M.-S., Lu C.-H., Huang Y.-K. The influence of diffuse left anterior descending artery lesions on outcomes of coronary artery bypass grafting. Heart Surg Forum. 2020;23(4):E498-E506. PMID: 32726216. https://doi.org/10.1532/hsf.2975
- Li D., Guo P., Chen L., Wu Y., Wang G., Xiao C. Outcomes of surgical patch angioplasty of the coronary artery for diffuse coronary artery disease. Braz J Cardiovasc Surg. 2020;35(5):706-712. PMID: 33118736; PMCID: PMC7598967. https://doi.org/10.21470/1678-9741-2019-0390
- Wang C., Chen J., Gu C., Li J. Analysis of survival after coronary endarterectomy combined with coronary artery bypass grafting compared with isolated coronary artery bypass grafting: a meta-analysis. Interact Cardiovasc Thorac Surg. 2019;29(3):393-401. PMID: 31180487. https://doi.org/10.1093/icvts/ivz125

