Nitric oxide and mitochondria injuries in kidney tissue upon a simulation of cardiopulmonary bypass and circulatory arrest: an experimental study
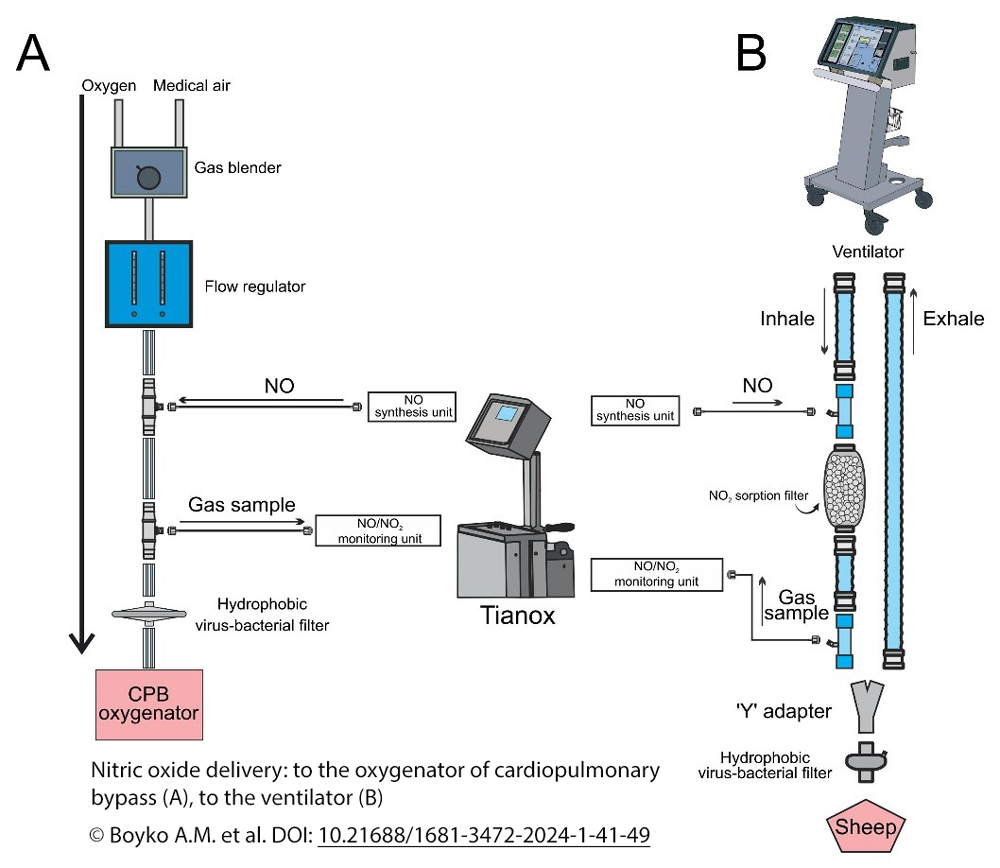
Published 2024-04-15
Keywords
- Adenosine Triphosphate,
- Animals,
- Cardiopulmonary Bypass,
- Kidney,
- Mitochondrial Diseases
- Nitric Oxide,
- Reperfusion Injury ...More
How to Cite
Copyright (c) 2024 Boyko A.M., Kamenshchikov N.O., Miroshnichenko A.G., Podoksenov Yu.K., Svirko Yu.S., Lugovskiy V.A., Diakova M.L., Kravchenko I.V., Mukhomedzyanov A.V., Maslov L.N., Bazarbekova B.A., Petlin K.A., Panfilov D.S., Kozlov B.N.

This work is licensed under a Creative Commons Attribution 4.0 International License.
Abstract
Introduction: Surgical interventions under cardiopulmonary bypass and circulatory arrest are complicated by impaired microcirculation in tissues; during hypoxic period the mitochondria dysfunction becomes the leading pathogenetic factor of ischemia-reperfusion injuries. In this regard, the search for methods of organ protection seems to be an extremely urgent task. The using of nitric oxide can be a promising technique given its pluripotent properties.
Objective: The study was aimed to examining of mitochondria injuries in kidney biopsies stipulated by cardiopulmonary bypass and circulatory arrest when simulating cardiac surgery, as well as to assessing the potentials of organ protection with nitric oxide in the experiment.
Methods: The study was carried out on Altai breed sheep and included simulating of cardiopulmonary bypass and circulatory arrest. The first group (n = 6) was provided with intraoperative nitric oxide donation. The second group (n = 6) served as a control (without nitric oxide donation). Mitochondria injuries were assessed in kidney biopsies by measuring transmembrane potential and Ca2+-binding capacity of organelles, as well as by determining ATP and lactate concentrations.
Results: Nitric oxide therapy was associated with less mitochondria dysfunction in kidney biopsies compared with the control group. There was a steady trend to the amelioration of the energy maintenance in the renal parenchyma in the nitric oxide donation group.
Conclusion: A steady trend towards optimizing the energy supply of tissues under cardiopulmonary bypass and circulatory arrest was revealed in an experiment against the background of NO donation at a concentration of 80 ppm.
Received 11 February 2024. Revised 28 March 2024. Accepted 29 March 2024.
Funding: The The study was carried out within the framework of the state assignment “Protection of organs by nitric oxide in cardiovascular surgery: technological support (synthesis and delivery devices), mechanisms for implementing protective effects and impact on clinical outcomes” (topic No. 122123000017-3).
Conflict of interest: The authors declare no conflict of interest.
Contribution of the authors
Conception and study design: A.M. Boyko, N.O. Kamenshchikov, Yu.K. Podoksenov, L.N. Maslov, B.N. Kozlov
Data collection and analysis: A.M. Boyko, Yu.S. Svirko, V.A. Lugovskiy, A.V. Mukhomedzyanov, B.A. Bazarbekova
Statistical analysis: I.V. Kravchenko
Drafting the article: A.M. Boyko
Critical revision of the article: N.O. Kamenshchikov, A.G. Miroshnichenko, Yu.K. Podoksenov, M.L. Diakova, K.A. Petlin, D.S. Panfilov, B.N. Kozlov
Final approval of the version to be published: A.M. Boyko, N.O. Kamenshchikov, A.G. Miroshnichenko, Yu.K. Podoksenov, Yu.S. Svirko, V.A. Lugovskiy, M.L. Diakova, I.V. Kravchenko, A.V. Mukhomedzyanov, L.N. Maslov, B.A. Bazarbekova, K.A. Petlin, D.S. Panfilov, B.N. Kozlov
References
- Каменщиков Н.О., Подоксенов Ю.К., Дьякова М.Л., Бойко А.М., Козлов Б.Н. Острое повреждение почек в кардиохирургии: определение, эпидемиология, исходы и социально-экономическая значимость. Патология кровообращения и кардиохирургия. 2020;24(4):11-21. https://doi.org/10.21688/1681-3472-2020-4-11-21 Kamenshchikov N.O., Podoksenov Y.K., Diakova M.L., Boyko A.M., Kozlov B.N. Acute kidney injury in cardiac surgery: definition, epidemiology, outcomes and socio-economic significance. Patologiya krovoobrashcheniya i kardiokhirurgiya = Circulation Pathology and Cardiac Surgery. 2020;24(4):11-21. (In Russ.) https://doi.org/10.21688/1681-3472-2020-4-11-21
- Scherner M., Weber C., Schmidt H., Kuhr K., Hamacher S., Sabashnikov A., Eghbalzadeh K., Mader N., Wahlers T., Wippermann J. Impact of urgent coronary artery bypass grafting on acute kidney injury: a matched cohort study. Med Klin Intensivmed Notfmed. 2022;117(2):152-158. PMID: 33471151. https://doi.org/10.1007/s00063-020-00769-x
- Harky A., Joshi M., Gupta S., Teoh W.Y., Gatta F., Snosi M. Acute kidney injury associated with cardiac surgery: a comprehensive literature review. Braz J Cardiovasc Surg. 2020;35(2):211-224. PMID: 32369303; PMCID: PMC7199993. https://doi.org/10.21470/1678-9741-2019-0122
- Amano K., Takami Y., Ishikawa H., Ishida M., Tochii M., Akita K., Sakurai Y., Noda M., Takagi Y. Lower body ischaemic time is a risk factor for acute kidney injury after surgery for type A acute aortic dissection. Interact Cardiovasc Thorac Surg. 2020;30(1):107-112. PMID: 31501854. https://doi.org/10.1093/icvts/ivz220
- Ghincea C.V., Reece T.B., Eldeiry M., Roda G.F., Bronsert M.R., Jarrett M.J., Pal J.D., Cleveland J.C. Jr., Fullerton D.A., Aftab M. Predictors of acute kidney injury following aortic arch surgery. J Surg Res. 2019;242:40-46. PMID: 31063910. https://doi.org/10.1016/j.jss.2019.03.055
- Lei C., Berra L., Rezoagli E., Yu B., Dong H., Yu S., Hou L., Chen M., Chen W., Wang H., Zheng Q., Shen J., Jin Z., Chen T., Zhao R., Christie E., Sabbisetti V.S., Nordio F., Bonventre J.V., Xiong L., Zapol W.M. Nitric oxide decreases acute kidney injury and stage 3 chronic kidney disease after cardiac surgery. Am J Respir Crit Care Med. 2018;198(10):1279-1287. PMID: 29932345; PMCID: PMC6290943. https://doi.org/10.1164/rccm.201710-2150OC
- Kamenshchikov N.O., Duong N., Berra L. Nitric oxide in cardiac surgery: a review article. Biomedicines. 2023;11(4):1085. PMID: 37189703; PMCID: PMC10135597. https://doi.org/10.3390/biomedicines11041085
- Khwaja A. KDIGO clinical practice guidelines for acute kidney injury. Nephron Clin Pract. 2012;120(4):c179-c184. PMID: 22890468. https://doi.org/10.1159/000339789
- Kork F., Balzer F., Spies C.D., Wernecke K.D., Ginde A.A., Jankowski J., Eltzschig H.K. Minor postoperative increases of creatinine are associated with higher mortality and longer hospital length of stay in surgical patients. Anesthesiology. 2015;123(6):1301-1311. PMID: 26492475; PMCID: PMC4679549. https://doi.org/10.1097/ALN.0000000000000891
- Haase M., Devarajan P., Haase-Fielitz A., Bellomo R., Cruz D.N., Wagener G., Krawczeski C.D., Koyner J.L., Murray P., Zappitelli M., Goldstein S.L., Makris K., Ronco C., Martensson J., Martling C.R., Venge P., Siew E., Ware L.B., Ikizler T.A., Mertens P.R. The outcome of neutrophil gelatinase-associated lipocalin-positive subclinical acute kidney injury: a multicenter pooled analysis of prospective studies. J Am Coll Cardiol. 2011;57(17):1752-1761. PMID: 21511111; PMCID: PMC4866647. https://doi.org/10.1016/j.jacc.2010.11.051
- Schurle A., Koyner J.L. CSA-AKI: incidence, epidemiology, clinical outcomes, and economic impact. J Clin Med. 2021;10(24):5746. PMID: 34945041; PMCID: PMC8706363. https://doi.org/10.3390/jcm10245746
- Brown J.K., Shaw A.D., Mythen M.G., Guzzi L., Reddy V.S., Crisafi C., Engelman D.T.; PeriOperative Quality Initiative and the Enhanced Recovery After Surgery Cardiac Workgroup. Adult cardiac surgery-associated acute kidney injury: joint consensus report. J Cardiothorac Vasc Anesth. 2023;37(9):1579-1590. PMID: 37355415. https://doi.org/10.1053/j.jvca.2023.05.032
- Hofmann F. A concise discussion of the regulatory role of cGMP kinase I in cardiac physiology and pathology. Basic Res Cardiol. 2018;113(4):1-11. PMID: 29934662. https://doi.org/10.1007/s00395-018-0690-1
- Lukowski R., Cruz Santos M., Kuret A., Ruth P. cGMP and mitochondrial K+ channels—Compartmentalized but closely connected in cardioprotection. Br J Pharmacol. 2022;179(11):2344-2360. PMID: 33991427. https://doi.org/10.1111/bph.15536
- Prokudina E.S., Naryzhnaya N.V., Mukhomedzyanov A.V., Gorbunov A.S., Zhang Y., Yaggi A.S., Tsibulnikov S.Y., Nesterov E.A., Lishmanov Y.B., Suleiman M.S., Oeltgen P.R., Maslov L.N. Effect of chronic continuous normobaric hypoxia on functional state of cardiac mitochondria and tolerance of isolated rat heart to ischemia and reperfusion: role of µ and delta2 opioid receptors. Physiol Res. 2019;68(6):909-920. PMID: 31647288. https://doi.org/10.33549/physiolres.933945
- Бойко А.М., Каменщиков Н.О., Мирошниченко А.Г., Подоксенов Ю.К., Серебрякова О.Н., Дзюман А.Н., Свирко Ю.С., Дымбрылова О.Н., Луговский В.А., Дьякова М.Л., Панфилов Д.С., Козлов Б.Н. Влияние доставки оксида азота на повреждение почек при моделировании искусственного кровообращения с циркуляторным арестом в эксперименте. Фундаментальная и клиническая медицина. 2023;8(3):18-25. https://doi.org/10.23946/2500-0764-2023-8-3-18-25 Boyko A.M., Kamenshchikov N.O., Miroshnichenko A.G., Podoksenov Yu.K., Serebryakova O.N., Dzyuman A.N., Svirko Yu.S., Dymbrylova O.N., Lugovskiy V.A., Diakova M.L., Panfilov D.S., Kozlov B.N. Influence of nitric oxide delivery on kidney damage in experimental model of cardiopulmonary bypass with circulatory arrest. Fundamental and Clinical Medicine. 2023;8(3):18-25. (In Russ.) https://doi.org/10.23946/2500-0764-2023-8-3-18-25
- Nagasaka Y., Fernandez B.O., Steinbicker A.U., Spagnolli E., Malhotra R., Bloch D.B., Bloch K.D., Zapol W.M., Feelisch M. Pharmacological preconditioning with inhaled nitric oxide (NO): organ-specific differences in the lifetime of blood and tissue NO metabolites. Nitric Oxide. 2018;80:52-60. PMID: 30114529; PMCID: PMC6198794. https://doi.org/10.1016/j.niox.2018.08.006
- Signori D., Magliocca A., Hayashida K., Graw J.A., Malhotra R., Bellani G., Berra L., Rezoagli E. Inhaled nitric oxide: role in the pathophysiology of cardio-cerebrovascular and respiratory diseases. Intensive Care Med Exp. 2022;10(1):28. PMID: 35754072; PMCID: PMC9234017. https://doi.org/10.1186/s40635-022-00455-6
- Poderoso J.J., Helfenberger K., Poderoso C. The effect of nitric oxide on mitochondrial respiration. Nitric Oxide. 2019;88:61-72. PMID: 30999001. https://doi.org/10.1016/j.niox.2019.04.005
- Shiva S., Sack M.N., Greer J.J., Duranski M., Ringwood L.A., Burwell L., Wang X., MacArthur P.H., Shoja A., Raghavachari N., Calvert J.W., Brookes P.S., Lefer D.J., Gladwin M.T. Nitrite augments tolerance to ischemia/reperfusion injury via the modulation of mitochondrial electron transfer. J Exp Med. 2007;204(9):2089-102. PMID: 17682069; PMCID: PMC2118713. https://doi.org/10.1084/jem.20070198
- Тё М.А., Каменщиков Н.О., Подоксенов Ю.К., Мухомедзянов А.В., Маслов Л.Н., Козлов Б.Н. Влияние доставки оксида азота на энергетическое обеспечение почечной ткани при проведении искусственного кровообращения: экспериментальное исследование. Сибирский журнал клинической и экспериментальной медицины. 2024;39(1):163-170. https://doi.org/10.29001/2073-8552-2022-592 Tyo M.A., Kamenshchikov N.O., Podoksenov Yu.K., Mukhomedzyanov A.V., Maslov L.N., Kozlov B.N. Effect of nitric oxide delivery on energy supply of renal tissue in cardiopulmonary bypass: an experimental study. The Siberian Journal of Clinical and Experimental Medicine. 2024;39(1):163-170. (In Russ.) https://doi.org/10.29001/2073-8552-2022-592
- Тё М.А., Каменщиков Н.О., Подоксенов Ю.К., Мухомедзянов А.В., Маслов Л.Н., Козлов Б.Н. Влияние донации оксида азота на выраженность митохондриальной дисфункции почечной ткани при моделировании искусственного кровообращения: экспериментальное исследование. Вестник интенсивной терапии им. А.И. Салтанова. 2023;(4):176-184. https://doi.org/10.21320/1818-474X-2023-4-176-184 Tyo M.A., Kamenshchikov N.O., Podoksenov Y.K., Mukhomedzyanov A.V., Maslov L.N., Kozlov B.N. The effect of nitric oxide donation on the severity of mitochondrial disfunction to the renal tissue in cardiopulmonary bypass simulation: an experimental study. Annals of Critical Care. 2023;(4):176-184. (In Russ.) https://doi.org/10.21320/1818-474X-2023-4-176-184
- Kumar A., Noda K., Philips B., Velayutham M., Stolz D.B., Gladwin M.T., Shiva S., D'Cunha J. Nitrite attenuates mitochondrial impairment and vascular permeability induced by ischemia-reperfusion injury in the lung. Am J Physiol Lung Cell Mol Physiol. 2020;318(4):L580-L591. PMID: 32073901; PMCID: PMC7191477. https://doi.org/10.1152/ajplung.00367.2018
- Jiang M., Bai M., Lei J., Xie Y., Xu S., Jia Z., Zhang A. Mitochondrial dysfunction and the AKI-to-CKD transition. Am J Physiol Renal Physiol. 2020;319(6):F1105-F1116. PMID: 33073587. https://doi.org/10.1152/ajprenal.00285.2020
- Фрелих Г.А., Поломеева Н.Ю., Васильев А.С., Удут В.В. Современные методы оценки функционального состояния митохондрий. Сибирский журнал клинической и экспериментальной медицины. 2013;28(3):7-13. Frelikh G.A., Polomeeva N.U., Vasilev A.S., Udut V.V. State-of-the art methods of evaluation of mitochondrial function. The Siberian Journal of Clinical and Experimental Medicine. 2013;28(3):7-13. (In Russ.)

