Published 2023-03-30
Keywords
- Allografts,
- Endocarditis,
- Heart Valve Prosthesis,
- Retrospective Studies,
- Staphylococcus aureus
How to Cite
Copyright (c) 2023 Bogachev-Prokophiev A.V., Sharifulin R.M., Zheleznev S.I., Karadzha A.V., Afanasyev A.V., Pivkin A.N., Zalesov A.S.

This work is licensed under a Creative Commons Attribution 4.0 International License.
Abstract
Background: Prosthetic valve endocarditis, the most severe form of infective endocarditis, occurs in 1-6% of patients with valve prostheses and is still associated with poor prognosis and high in-hospital mortality.
Objective: To assess outcomes of allograft aortic root replacement in patients with prosthetic valve endocarditis.
Methods: The retrospective analysis included adult patients with prosthetic valve endocarditis, who underwent allograft aortic root replacement between 2011 and 2022.
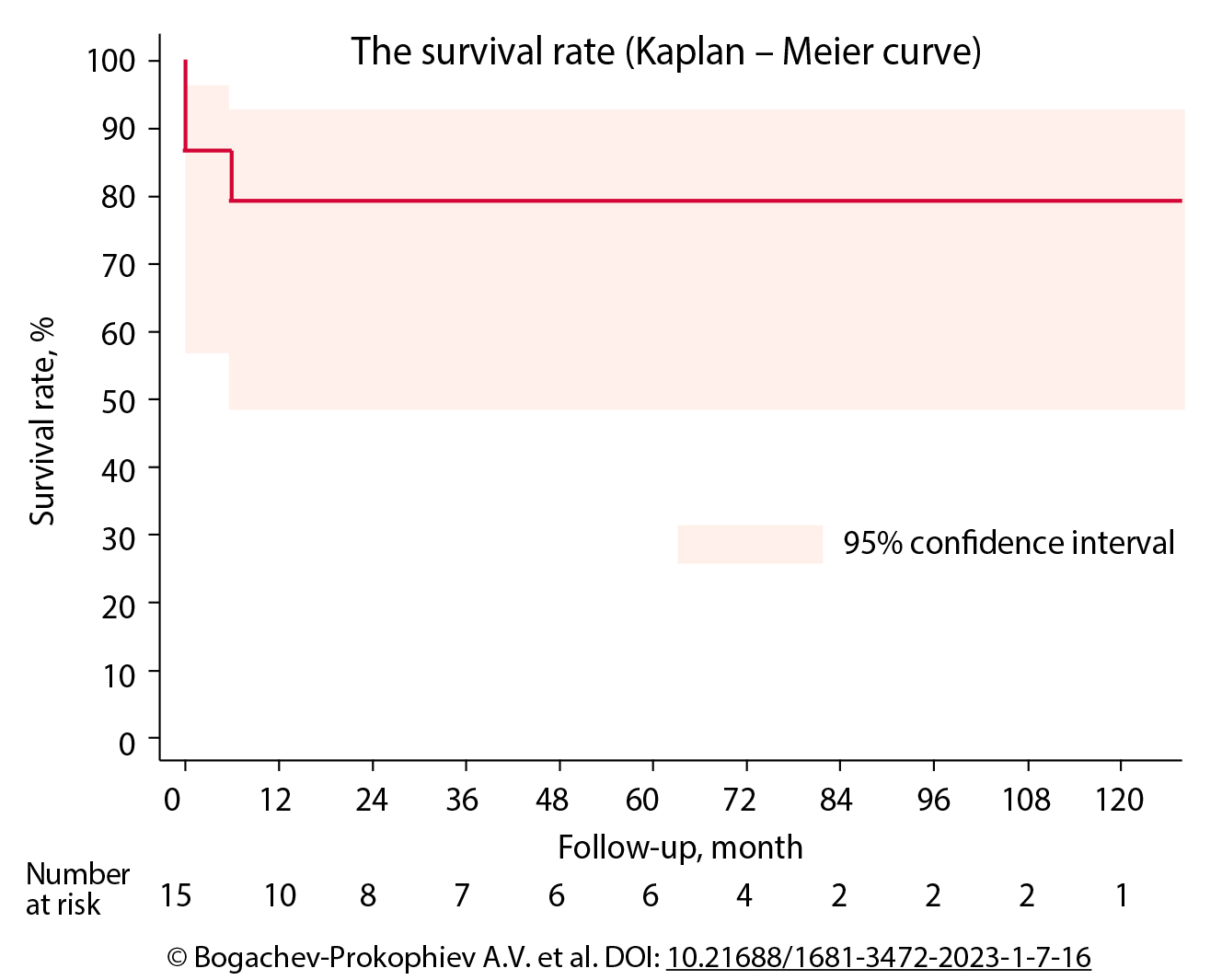
Results: Of 15 study patients, early infective endocarditis was found in 60.0% of the cases. The most common cause was Staphylococcus aureus (26.7%). Early mortality was 13.3%. Thromboembolic events occurred in 2 patients (13.3%). The median follow-up period was 48.5 (6-140) months. Late death was reported in 1 patient. The 5-year survival rate was 79.0%. One patient had recurrent infective endocarditis. Two patients underwent reintervention: one for a proximal anastomotic pseudoaneurysm and another one for structural degeneration of the allograft. Five-year freedom from reintervention was 91.7%.
Conclusion: Due to the high rate of the freedom from recurrent infective endocarditis, allograft aortic root replacement is an effective treatment for patients with prosthetic valve endocarditis.
Received 7 November 2022. Revised 9 December 2022. Accepted 20 December 2022.
Funding: The study was supported by the grant of the president of the Russian Federation (No. 075-15-2022-823).
Conflict of interest: The authors declare no conflict of interest.
Contribution of the authors
Conception and study design: A.V. Bogachev-Prokophiev
Data collection and analysis: A.V. Karadzha, A.N. Pivkin, A.S. Zalesov
Statistical analysis: R.M. Sharifulin, A.V. Afanasyev
Drafting the article: R.M. Sharifulin, A.V. Afanasyev
Critical revision of the article: A.V. Bogachev-Prokophiev, S.I. Zheleznev
Final approval of the version to be published: A.V. Bogachev-Prokophiev, R.M. Sharifulin, S.I. Zheleznev, A.V. Karadzha, A.V. Afanasyev, A.N. Pivkin, A.S. Zalesov
References
- Wang A. Statement from the International Collaboration on Endocarditis on the current status of surgical outcome in infective endocarditis. Ann Cardiothorac Surg. 2019;8(6):678-680. PMID: 31832359; PMCID: PMC6892721. https://dx.doi.org/10.21037/acs.2019.05.19
- Habib G., Lancellotti P., Antunes M.J., Bongiorni M.G., Casalta J.-P., Del Zotti F., Dulgheru R., El Khoury G., Erba P.A., Iung B., Miro J.M., Mulder B.J., Plonska-Gosciniak E., Price S., Roos-Hesselink J., Snygg-Martin U., Thuny F., Mas P.T., Vilacosta I., Zamorano J.L.; ESC Scientific Document Group. 2015 ESC Guidelines for the management of infective endocarditis: The Task Force for the Management of Infective Endocarditis of the European Society of Cardiology (ESC). Endorsed by: European Association for Cardio-Thoracic Surgery (EACTS), the European Association of Nuclear Medicine (EANM). Eur Heart J. 2015;36(44):3075-3128. PMID: 26320109. https://dx.doi.org/10.1093/eurheartj/ehv319
- Chu V.H., Park L.P., Athan E., Delahaye F., Freiberger T., Lamas C., Miro J.M., Mudrick D.W., Strahilevitz J., Tribouilloy C., Durante-Mangoni E., Pericas J.M., Fernández-Hidalgo N., Nacinovich F., Rizk H., Krajinovic V., Giannitsioti E., Hurley J.P., Hannan M.M., Wang A.; International Collaboration on Endocarditis. Association between surgical indications, operative risk, and clinical outcome in infective endocarditis: a prospective study from the International Collaboration on Endocarditis. Circulation. 2015;131(2):131-140. PMID: 25480814. https://dx.doi.org/10.1161/CIRCULATIONAHA.114.012461
- Lalani T., Chu V.H., Park L.P., Cecchi E., Corey G.R., Durante-Mangoni E., Fowler Jr V.G., Gordon D., Grossi P., Hannan M., Hoen B., Muñoz P., Rizk H., Kanj S.S., Selton-Suty C., Sexton D.J., Spelman D., Ravasio V., Tripodi M.F., Wang A.; International Collaboration on Endocarditis–Prospective Cohort Study Investigators. In-hospital and 1-year mortality in patients undergoing early surgery for prosthetic valve endocarditis. JAMA Intern Med. 2013;173(16):1495-1504. PMID: 23857547. https://dx.doi.org/10.1001/jamainternmed.2013.8203
- Davierwala P.M., Marin-Cuartas M., Misfeld M., Deo S.V., Lehmann S., Garbade J., Holzhey D.M., Borger M.A., Bakhtiary F. Five-year outcomes following complex reconstructive surgery for infective endocarditis involving the intervalvular fibrous body. Eur J Cardiothorac Surg. 2020;58(5):1080-1087. PMID: 32380545. https://dx.doi.org/10.1093/ejcts/ezaa146
- Navia J.L., Elgharably H., Hakim A.H., Witten J.C., Haupt M.J., Germano E., Houghtaling P.L., Bakaeen F.G., Pettersson G.B., Lytle B.W., Roselli E.E., Gillinov A.M., Svensson L.G. Long-term outcomes of surgery for invasive valvular endocarditis involving the aortomitral fibrosa. Ann Thorac Surg. 2019;108(5):1314-1323. PMID: 31254508. https://dx.doi.org/10.1016/j.athoracsur.2019.04.119
- Solari S., Mastrobuoni S., De Kerchove L., Navarra E., Astarci P., Noirhomme P., Poncelet A., Jashari R., Rubay J., El Khoury G. Over 20 years experience with aortic homograft in aortic valve replacement during acute infective endocarditis. Eur J Cardiothorac Surg. 2016;50:1158-1164. PMID: 27229671. https://dx.doi.org/10.1093/ejcts/ezw175
- Musci M., Weng Y., Hübler M., Amiri A., Pasic M., Kosky S., Stein J., Siniawski H., Hetzer R. Homograft aortic root replacement in native or prosthetic active infective endocarditis: twenty-year single-center experience. J Thorac Cardiovasc Surg. 2010;139(3):665-673. PMID: 19767017. https://dx.doi.org/10.1016/j.jtcvs.2009.07.026
- Kim J.B., Ejiofor J.I., Yammine M., Camuso J.M., Walsh C.W., Ando M., Melnitchouk S.I., Rawn J.D., Leacche M., MacGillivray T.E., Cohn L.H., Byrne J.G., Sundt T.M. Are homografts superior to conventional prosthetic valves in the setting of infective endocarditis involving the aortic valve? J Thorac Cardiovasc Surg. 2016;151(5):1239-1246. PMID: 26936004. https://dx.doi.org/10.1016/j.jtcvs.2015.12.061
- Yanagawa B., Mazine A., Tam D.Y., Jüni P., Bhatt D.L., Spindel S., Puskas J.D., Verma S., Friedrich J.O. Homograft versus conventional prosthesis for surgical management of aortic valve infective endocarditis: a systematic review and meta-analysis. Innovations (Phila). 2018;13(3):163-170. PMID: 29912740. https://dx.doi.org/10.1097/IMI.0000000000000510
- Sharifulin R., Bogachev-Prokophiev A., Varnek Y., Klimko N., Malakhova O., Volkov A., Murashev I., Pivkin A., Karaskov A. Successful treatment of an aortotomy site aspergillus infection. Ann Thorac Surg. 2019;108(4):e253-e255. PMID: 30910659. https://dx.doi.org/10.1016/j.athoracsur.2019.02.036
- Elgharably H., Hakim A.H., Unai S., Hussain S.T., Shrestha N.K., Gordon S., Rodriguez L., Gillinov A.M., Svensson L.G., Navia J.L. The incorporated aortomitral homograft for double-valve endocarditis: the 'hemi-Commando' procedure. Early and mid-term outcomes. Eur J Cardiothorac Surg. 2018;53(5):1055-1061. PMID: 29253091. https://dx.doi.org/10.1093/ejcts/ezx439
- Чернов И.И., Екимов С.С., Мотрева А.П., Кондратьев Д.А., Маркина М.И., Тарасов Д.Г. Лечение протезного эндокардита с использованием аортально-митрального гомографта. Клиническая и экспериментальная хирургия. Журнал им. акад. Б.В. Петровского. 2015;3:70-72. Chernov I.I., Ekimov S.S., Motreva A.P., Kondratyev D.A., Markina M.I., Tarasov D.G. Double valve replacement with aorto-mitral homograft in patient with prosthestic endocarditis. Clin Experiment Surg. Petrovsky J. 2015;3:70-72. (In Russ.)
- Спиридонов С.В., Шкет А.П., Чеснов Ю.М., Щетинко Н.Н., Одинцов В.О., Шумовец В.В., Андрущук В.В., Комаровский А.А., Островский Ю.П. Непосредственные результаты протезирования аортального клапана с использованием аллографтов. Новости хирургии. 2014;22(4):443-448. https://dx.doi.org/10.18484/2305-0047.2014.4.443 Spirydonov S.V., Shket A.P., Chesnov Yu.M., Shchetinko N.N., Odintsov V.O., Shumovets V.V., Andrushchuk V.V., Komarovsky A.A., Ostrovsky Yu.P. The immediate results of aortic valve replacement with allografts. Novosti Khirurgii. 2014;22(4):443-448. (In Russ.) https://dx.doi.org/10.18484/2305-0047.2014.4.443
- Heinz A., Dumfarth J., Ruttmann-Ulmer E., Grimm M., Müller L.C. Freestyle root replacement for complex destructive aortic valve endocarditis. J Thorac Cardiovasc Surg. 2014;147(4):1265-1270. PMID: 23849892. https://dx.doi.org/10.1016/j.jtcvs.2013.05.014
- Melina G., De Robertis F., Gaer J.A., Angeloni E., El-Hamamsy I., Bahrami T., Pepper J.R., Takkenberg J.J.M., Yacoub M.H. Long-term survival after xenograft versus homograft aortic root replacement: Results from a prospective randomized trial. J Thorac Cardiovasc Surg. 2019;161(1):57-65. PMID: 31735388. https://dx.doi.org/10.1016/j.jtcvs.2019.09.119
- Караськов А.М., Опен А.Б., Демидов Д.П., Железнев С.И., Демин И.И., Астапов Д.А. Операция Росса как метод радикальной коррекции аортальной недостаточности при инфекционном эндокардите высокой степени активности. Патология кровообращения и кардиохирургия. 2011;(3):71-73. Karaskov A.M., Open A.B., Demidov D.P., Zheleznev S.I., Demin I.I., Astapov D.A. Ross operation as a method of radical correction of aortic insufficiency in infectious endocarditis of high activity levels. Patologiya krovoobrashcheniya i kardiokhirurgiya = Circulation Pathology and Cardiac Surgery. 2011;(3):71-73. (In Russ.)
- Chauvette V., Bouhout I., Lefebvre L., Tarabzoni M., Chamberland M.È., Poirier N., Demers P., Chu M.W.A., Perron J., El-Hamamsy I. The Ross procedure is a safe and durable option in adults with infective endocarditis: a multicentre study. Eur J Cardiothorac Surg. 2020;58(3):537-543. PMID: 32236477. https://dx.doi.org/10.1093/ejcts/ezaa078
- Сулейманов Б.Р., Муратов Р.М., Бритиков Д.В., Соболева Н.Н., Титов Д.А. Использование алло- и аутографтов (операция Росса) при активном инфекционном эндокардите с деструкцией корня аорты. Анналы хирургии. 2016;21(3):180-186. Suleymanov B.R., Muratov R.M., Britikov D.V., Soboleva N.N., Titov D.A. The use of allo- and autografts (Ross procedure) in active infective endocarditis with the aortic root destruction. Annaly khirurgii = Annals of Surgery. Russian Journal. 2016;21(3):180-186. (In Russ.)

