Intraoperative stimulation mapping of sensory branches of the trigeminal nerve using unconditioned reflexes: a case series
Published 2024-12-27
Keywords
- Case Reports,
- Intraoperative Neurophysiological Monitoring,
- Microvascular Decompression Surgery,
- Neurosurgical Procedures,
- Trigeminal Nerve
- Trigeminal Neuralgia,
- Reflexes ...More
How to Cite
Copyright (c) 2024 Levin E.A., Kilchukov M.G., Glushaeva A.A., Kiselev R.S.

This work is licensed under a Creative Commons Attribution 4.0 International License.
Abstract
Introduction: Intraoperative stimulation mapping enables to determine the location of nerves in the surgical field when visualization is difficult, as well as to identify visualized nerves, thereby reducing the risk of postoperative iatrogenic complications. Motor nerve mapping is widely used in neurosurgical procedures but only a few attempts at intraoperative sensory nerve mapping have been reported to date. The introduction of an effective method for mapping the sensory branches/portions of the trigeminal nerve can reduce the risk of complications such as facial hypo- and hyperesthesia after operations in the posterior cranial fossa.
Objective: To demonstrate the possibility of using unconditioned reflex motor reactions for stimulation mapping of the sensory branches/portions of the trigeminal nerve.
Methods: Intraoperative neuromonitoring records were analyzed in three patients with trigeminal neuralgia who underwent nerve stimulation mapping during microvascular decompression. The using of an extended to 40 ms time window for recording myographic responses enabled to record both short-latency direct motor responses to stimulation of motor nerves and long-latency reflex motor responses to stimulation of the sensory branches of the trigeminal nerve.
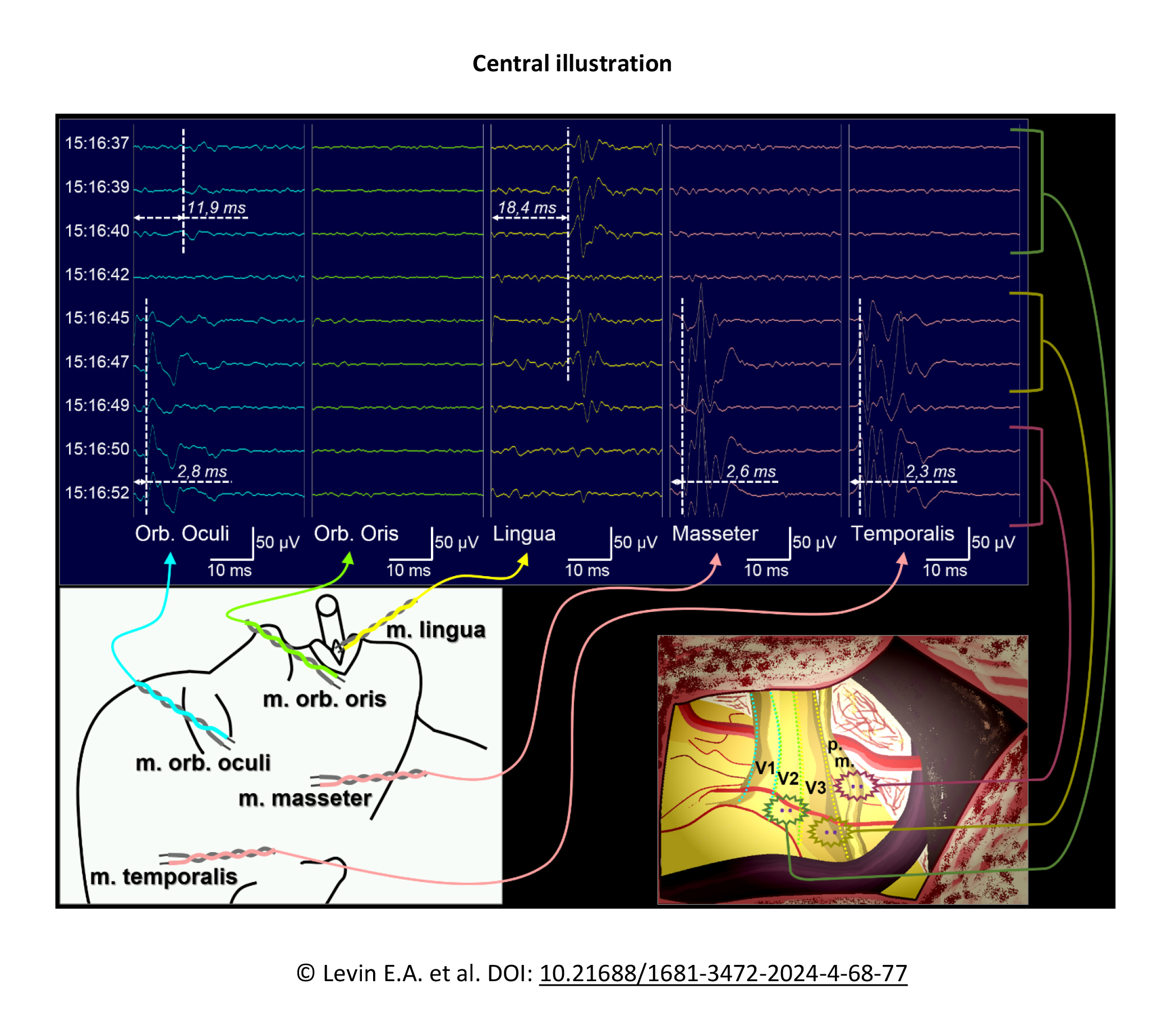
Results: It was shown that unconditioned reflex reactions of the orbicularis oculi muscle (stimulation of the V1 portion of the trigeminal nerve, blink reflex) and tongue muscles (stimulation of V3, trigemino hypoglossal reflex) were successfully induced in patients under total intravenous anesthesia with both monopolar and bipolar stimulation. One patient also showed a reaction of the orbicularis oris muscle (stimulation of V2, snout reflex). The technique used enabled to differentiate not only the motor and sensory roots of the trigeminal nerve, but also its different sensory portions separately.
Conclusion: The intraoperative stimulation mapping of sensory branches/portions of the trigeminal nerve via unconditioned reflex motor responses can be performed using the equipment and anesthesia regimen typical for motor nerve mapping.
Received 10 October 2024. Revised 1 November 2024. Accepted 12 November 2024.
Informed consent
The patients’ informed consent to use the records for medical purposes is obtained.
Funding
The study was supported by the grant of Russian Science Foundation No. 23-25-00322.
Conflict of interest
The authors declare no conflict of interest.
Contribution of the authors
The authors contributed equally to this article.
References
- Gudmundsson K., Rhoton A.L., Rushton J.G. Detailed anatomy of the intracranial portion of the trigeminal nerve. J Neurosurg. 1971;35(5):592-600. PMID: 5120007. https://doi.org/10.3171/jns.1971.35.5.0592
- Lopez J.R., Legatt A.D. Monitoring surgery around the cranial nerves. Handb Clin Neurol. 2022;186:319-351. PMID: 35772894. https://doi.org/10.1016/B978-0-12-819826-1.00020-X
- Шкарубо А.Н., Огурцова А.А., Мощев Д.А., Лубнин А.Ю., Андреев Д.Н., Коваль К.В., Чернов И.В. Нейрофизиологическая идентификация черепных нервов в эндоскопической эндоназальной хирургии опухолей основания черепа. Журнал «Вопросы нейрохирургии» имени Н.Н. Бурденко. 2016;80(3):35-49. https://doi.org/10.17116/neiro201680335-49 Shkarubo A.N., Ogurtsova A.A., Moshchev D.A., Lubnin A.Y., Andreev D.N., Koval K.V., Chernov I.V. Neurophysiological identification of the cranial nerves in endoscopic endonasal surgery of skull base tumors. Burdenko’s Journal of Neurosurgery. 2016;80(3):35-49. (In Russ.) https://doi.org/10.17116/neiro201680335-49
- Stechison M.T., Møller A., Lovely T.J. Intraoperative mapping of the trigeminal nerve root: technique and application in the surgical management of facial pain. Neurosurgery. 1996;38(1):76-82. PMID: 8747954. https://doi.org/10.1097/00006123-199601000-00018
- Lin B., Lu X., Zhai X., Cai Z. Use of sensory and motor action potentials to identify the position of trigeminal nerve divisions for radiofrequency thermocoagulation. J Neurosurg. 2014;121(6):1497-1503. PMID: 25280092. https://doi.org/10.3171/2014.8.JNS132484
- Carrai R., Morone F., Baldanzi F., Martinelli C., Bonaudo C., Tola S., Muscas G., Caramelli R., Spalletti M., Grippo A., Bucciardini L., Amadori A., Della Pupa A. Intraoperative mapping of the sensory root of the trigeminal nerve in patients with pontocerebellar angle pathology. World Neurosurg. 2023;178:e104-112. PMID: 37454910. https://doi.org/10.1016/j.wneu.2023.06.146
- Choi J., Diaz-Baamonde A., Sánchez Roldán M.L.A., Pescador A.M., Kim J.-S., Tellez M.J., Park K.S., Deletis V. Advancing intraoperative neurophysiological monitoring with human reflexes. J Clin Neurol. 2024;20(2):119. PMID: 38433484; PMCID: PMC10921042. https://doi.org/10.3988/jcn.2023.0416
- Deletis V., Urriza J., Ulkatan S., Fernandez‐Conejero I., Lesser J., Misita D. The feasibility of recording blink reflexes under general anesthesia. Muscle Nerve. 2009;39(5):642-646. PMID: 19347924. https://doi.org/10.1002/mus.21257
- Fernandez-Conejero I., Ulkatan S., Sen C., Deletis V. Intra-operative neurophysiology during microvascular decompression for hemifacial spasm. Clin Neurophysiol. 2012;123(1):78-83. PMID: 22136736. https://doi.org/10.1016/j.clinph.2011.10.007
- Pescador A.M., Tellez M.J., Roldan M.D., Samusyte G., Lawson E.C., Coelho P., Lejarde A., Rathore A., Le D., Ulkatan S. Methodology for eliciting the brainstem trigeminal-hypoglossal reflex in humans under general anesthesia. Clin Neurophysiol. 2022;137:1-10. PMID: 35231863. https://doi.org/10.1016/j.clinph.2022.02.004
- Szelenyi A., Fava E. Long latency responses in tongue muscle elicited by various stimulation sites in anesthetized humans. New insights into tongue-related brainstem reflexes. Brain Stimul. 2022;15(3):566-575. PMID: 35341967. https://doi.org/10.1016/j.brs.2022.03.003
- Ali H.H., Utting J.E., Gray C. Stimulus frequency in the detection of neuromuscular block in humans. Br J Anaesth. 1970;42(11):967-978. PMID: 5488360. https://doi.org/10.1093/bja/42.11.967
- Macaluso G.M., De Laat A. H-reflexes in masseter and temporalis muscles in man. Exp Brain Res. 1995;107:315-320. PMID: 8773249. https://doi.org/10.1007/BF00230051
- Girlanda P., Roberto M.L., Dattola R., Morgante L., Venuto C., Messina C. Electrophysiological study of the snout reflex in normal subjects and in parkinsonian and pseudobulbar patients. Eur Neurol. 1986;25(3):166-171. PMID: 3699067. https://doi.org/10.1159/000116004
- Cruccu G., Bowsher D. Intracranial stimulation of the trigeminal nerve in man. II. Reflex responses. J Neurol Neurosurg Psychiatry. 1986;49(4):419-427. PMID: 3701351; PMCID: PMC1028769. https://doi.org/10.1136/jnnp.49.4.419
- Maisonobe T., Tankere F., Lamas G., Soudant J., Bouche P., Willer J.C., Fournier E. Reflexes elicited from cutaneous and mucosal trigeminal afferents in normal human subjects. Brain Research. 1998;810(1-2):220-228. PMID: 9813339. https://doi.org/10.1016/s0006-8993(98)00953-6
- Григорян Г.Ю., Древаль О.Н., Ситников А.Р., Григорян Ю.А. Анатомическое обоснование хирургического лечения тригеминальной невралгии, сочетающейся с опухолями мостомозжечкового угла. Журнал «Вопросы нейрохирургии» имени Н.Н. Бурденко. 2019;83(1):53-66. https://doi.org/10.17116/neiro20198301153 Grigoryan G.Yu., Dreval O.N., Sitnikov A.R., Grigoryan Yu.A. Anatomical rationale for surgical treatment of trigeminal neuralgia combined with cerebellopontine angle tumors. Burdenko’s Journal of Neurosurgery. 2019;83(1):53-66. (In Russ.) https://doi.org/10.17116/neiro20198301153
- Chen D.Q., Quan J., Guha A., Tymianski M., Mikulis D., Hodaie M. Three-dimensional in vivo modeling of vestibular schwannomas and surrounding cranial nerves with diffusion imaging tractography. Neurosurgery. 2011;68(4):1077-1083. PMID: 21242825. https://doi.org/10.1227/NEU.0b013e31820c6cbe
- Huang X., Xu J., Xu M., Chen M., Ji K., Ren J., Zhong P. Functional outcome and complications after the microsurgical removal of giant vestibular schwannomas via the retrosigmoid approach: a retrospective review of 16-year experience in a single hospital. BMC Neurology. 2017;17(1):18. PMID: 28137246; PMCID: PMC5282727. https://doi.org/10.1186/s12883-017-0805-6
- Ashram Y.A., Zohdy Y.M., Rayan T.A., Badr-El-Dine M.M. Value of intraoperative monitoring of the trigeminal nerve in detection of a superiorly displaced facial nerve during surgery for large vestibular schwannomas. Neurosurg Rev. 2022;45(2):1343-1351. PMID: 34533668. https://doi.org/10.1007/s10143-021-01646-7
- Terrier L.-M., Amelot A., François P., Destrieux C., Zemmoura I., Velut S. Therapeutic failure in trigeminal neuralgia: from a clarification of trigeminal nerve somatotopy to a targeted partial sensory rhizotomy. World Neurosurg. 2018;117:e138-e145. PMID: 29883821. https://doi.org/10.1016/j.wneu.2018.05.211
- Bigder M.G., Krishnan S., Cook E.F., Kaufmann A.M. Microsurgical rhizotomy for trigeminal neuralgia in MS patients: technique, patient satisfaction, and clinical outcomes. J Neurosurg. 2018;130(6):1877-1888. PMID: 30004276. https://doi.org/10.3171/2017.12.JNS171647
- Dandy W.E. An operation for the cure of tic douloureux: partial section of the sensory root at the pons. Archives of Surgery. 1929;18(2):687-734. https://doi.org/10.1001/archsurg.1929.04420030081005

