Does aortic valve anatomy affect the long-term outcomes of aortic root reimplantation? A retrospective study with propensity score matching
Published 2024-12-27
Keywords
- Aortic Valve,
- Aortic Valve Insufficiency,
- Bicuspid Aortic Valve Disease,
- Follow-Up Studies,
- Propensity Score
- Reimplantation,
- Retrospective Studies ...More
How to Cite
Copyright (c) 2024 Kokorin A.V., Aminov V.V., Lukin O.P., Bogachev-Prokofiev A.V.

This work is licensed under a Creative Commons Attribution 4.0 International License.
Abstract
Introduction: The results of aortic root reimplantation techniques in patients with tricuspid aortic valve (TAV) are generally recognized. However, data on the results of valve-preserving operations in patients with bicuspid aortic valve (BAV) remain limited.
Objective: In this retrospective study we compare the long-term results of reimplantation technique, depending on the type of aortic valve (AV): BAV versus TAV.
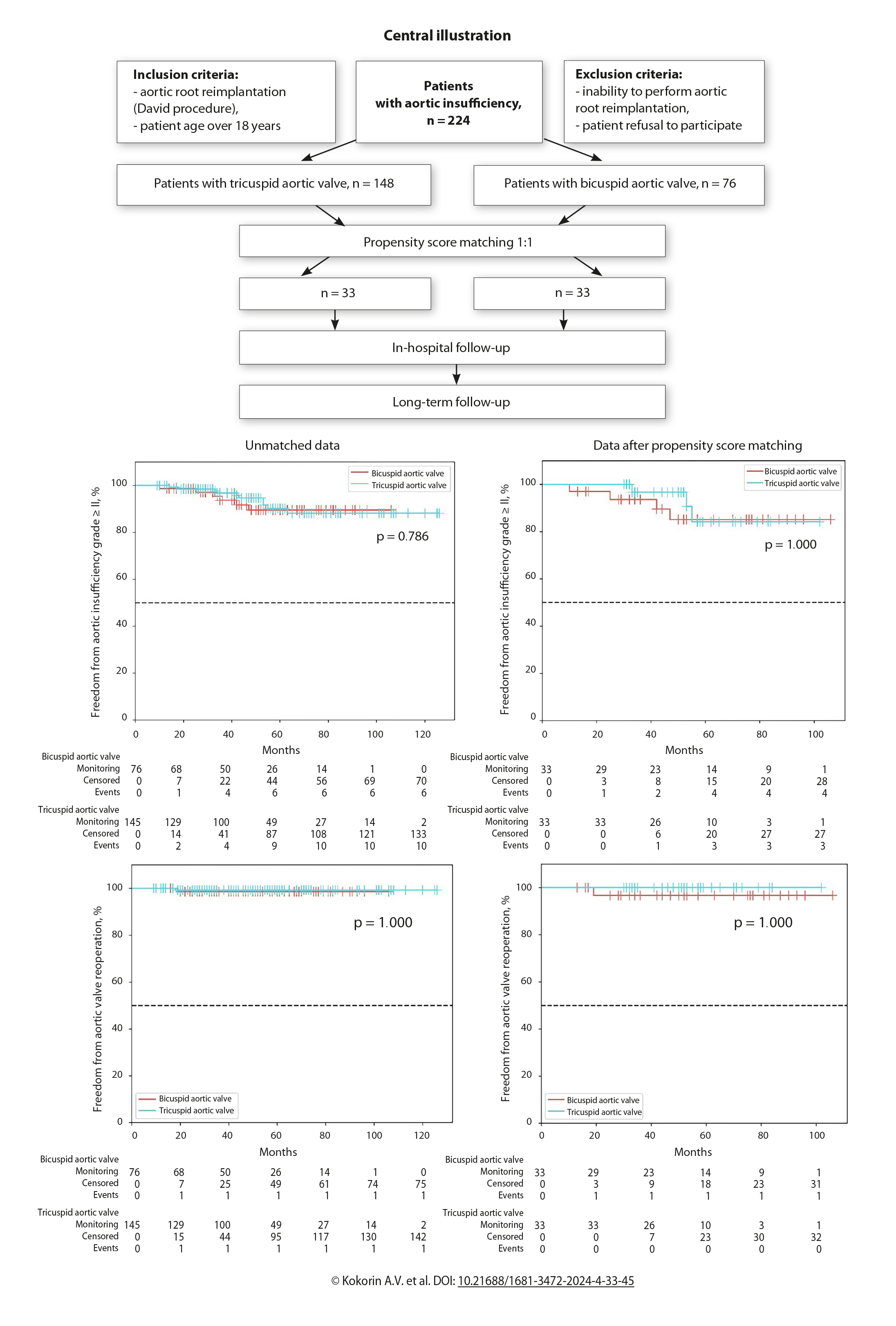
Methods: The retrospective study included 224 patients (average age 48.43 ± 13.70 years, 81.2% men) who underwent valve-preserving operations by reimplantation of the aortic root from January 2013 to January 2023. Depending on the anatomical variant of the AV, the entire sample was divided into two groups: 76 patients with BAV (33.9%) and 148 patients with TAV (66.1%). To eliminate the systematic differences between the compared groups, the propensity score matching (PSM) analysis was used in order to compare groups by 12 criteria. As a result, 33 pairs of patients were formed. After the PSM analysis, there were no significant differences between the groups.
Results: In total, 221 (98.2%) patients were examined in the long-term period. The average follow-up period for the entire sample was 53.17 ± 26.34 months. After the PSM analysis, there were no significant differences between the groups in the number of patients examined, namely 33 individuals (100%) in each group. The average follow-up period was 55.24 ± 22.66 months. At long-term follow-up, 100% survival was recorded in both groups. Prior to the PSM analysis, the freedom from aortic insufficiency (AI) grade ≥ II in the patients with TAV was 90.2% and 88.2% at 5 and 10 year follow-up periods, and in patients with BAV this indicator was 89.6% and 89.6% (p = 0.786), respectively. After the PSM analysis, the freedom from AI grade ≥ II in the patients with TAV was 84.2% and 84.2% at 5 and 8 year follow-up periods, and in the group with BAV it was 85.1% and 85.1% (p = 1.000), respectively. Prior to the PSM analysis, freedom from aortic valve reoperation at 5 and 10 year follow-up periods in the patients with TAV was 99.3%, and in the patients with BAV it was 98.6% (p = 1.000). After the PSM analysis, this indicator at 5 and 8 year follow-up periods in the patients with TAV and with BAV was 100% and 96.7%, respectively (p = 1.000).
Conclusion: The reimplantation technique enables to effectively reconstruct the aortic root regardless of the anatomical variant of the AV, providing excellent survival with a low risk of reoperation.
Received 2 October 2024. Revised 4 November 2024. Accepted 8 November 2024.
Funding
The research was carried out within the framework of the grant of the Russian Science Foundation No. 23-15-00434.
Conflict of interest
The authors declare no conflict of interest.
Contribution of the authors
The authors contributed equally to this article.
References
- Misawa Y. Valve-related complications after mechanical heart valve implantation. Surg Today. 2015;45(10):1205-1209. PMID: 25519937; PMCID: PMC4565860. https://doi.org/10.1007/s00595-014-1104-0
- Chan V., Malas T., Lapierre H., Boodhwani M., Lam B.-K., Rubens F.D., Hendry P.J., Masters R.G., Goldstein W., Mesana T.G., Ruel M. Reoperation of left heart valve bioprostheses according to age at implantation. Circulation. 2011;124(11 Suppl):S75-S80. PMID: 21911822. https://doi.org/10.1161/CIRCULATIONAHA.110.011973
- David T.E., Feindel C.M. An aortic valve-sparing operation for patients with aortic incompetence and aneurysm of the ascending aorta. J Thorac Cardiovasc Surg. 1992;103(4):617-621; discussion 622. PMID: 1532219. https://doi.org/10.1016/S0022-5223(19)34942-6
- David T.E., David C.M., Feindel C.M., Manlhiot C. Reimplantation of the aortic valve at 20 years. J Thorac Cardiovasc Surg. 2017;153(2):232-238. PMID: 27923487. https://doi.org/10.1016/j.jtcvs.2016.10.081
- David T.E., Armstrong S., Manlhiot C., McCrindle B.W., Feindel C.M. Long-term results of aortic root repair using the reimplantation technique. J Thorac Cardiovasc Surg. 2013;145(3 Suppl):S22-S25. PMID: 23260437. https://doi/10.1016/j.jtcvs.2012.11.075
- Coselli J.S., Hughes M.S., Green S.Y., Price M.D., Zarda S., de la Cruz K.I., Preventza O., LeMaire S.A. Valve-sparing aortic root replacement: early and midterm outcomes in 83 patients. Ann Thorac Surg. 2014;97(4):1267-1273; discussion 1273-1274. PMID: 24424011. https://doi.org/10.1016/j.athoracsur.2013.10.076
- Kvitting J.-P.E., Kari F.A., Fischbein M.P., Liang D.H., Beraud A.-S., Stephens E.H., Mitchell R.S., Miller D.C. David valve-sparing aortic root replacement: equivalent mid-term outcome for different valve types with or without connective tissue disorder. J Thorac Cardiovasc Surg. 2013;145(1):117-127; discussion 126-127. PMID: 23083792; PMCID: PMC6382393. https://doi.org/10.1016/j.jtcvs.2012.09.013
- Ouzounian M., Feindel C.M., Manlhiot C., David C., David T.E. Valve-sparing root replacement in patients with bicuspid versus tricuspid aortic valves. J Thorac Cardiovasc Surg. 2019;158(1):1-9. PMID: 31248507. https://doi.org/10.1016/j.jtcvs.2018.10.151
- Karciauskas D., Mizariene V., Jakuska P., Ereminiene E., Orda P., Ordiene R., Vaskelyte J.J., Nedzelskiene I., Kinduris S., Benetis R. Early and long-term results of aortic valve sparing aortic root reimplantation surgery for bicuspid and tricuspid aortic valves. Perfusion. 2019;34(6):482-489. PMID: 30823866. https://doi.org/10.1177/0267659119831926
- Klotz S., Stock S., Sievers H.-H., Diwoky M., Petersen M., Stierle U., Richardt D. Survival and reoperation pattern after 20 years of experience with aortic valve-sparing root replacement in patients with tricuspid and bicuspid valves. J Thorac Cardiovasc Surg. 2018;155(4):1403-1411.e1. PMID: 29338868. https://doi.org/10.1016/j.jtcvs.2017.12.039
- Sievers H.-H., Schmidtke C. A classification system for the bicuspid aortic valve from 304 surgical specimens. J Thorac Cardiovasc Surg. 2007;133(5):1226-1233. PMID: 17467434. https://doi.org/10.1016/j.jtcvs.2007.01.039
- de Kerchove L., Boodhwani M., Glineur D., Noirhomme P., El Khoury G. A new simple and objective method for graft sizing in valve-sparing root replacement using the reimplantation technique. Ann Thorac Surg. 2011;92(2):749-751. PMID: 21801943. https://doi.org/10.1016/j.athoracsur.2011.03.015
- David T.E., David C.M., Manlhiot C., Colman J., Crean A.M., Bradley T. Outcomes of aortic valve-sparing operations in Marfan syndrome. J Am Coll Cardiol. 2015;66(13):1445-1453. PMID: 26403341. https://doi.org/10.1016/j.jacc.2015.07.041
- David T.E., David C.M., Ouzounian M., Feindel C.M., Lafreniere-Roula M. A progress report on reimplantation of the aortic valve. J Thorac Cardiovasc Surg. 2021;161(3):890-899.e1. PMID: 33008570. https://doi.org/10.1016/j.jtcvs.2020.07.121
- Tamer S., Mastrobuoni S., Lemaire G., Jahanyar J., Navarra E., Poncelet A., Astarci P., El Khoury G., de Kerchove L. Two decades of valve-sparing root reimplantation in tricuspid aortic valve: impact of aortic regurgitation and cusp repair. Eur J Cardiothorac Surg. 2021;59(5):1069-1076. PMID: 33332548. https://doi.org/10.1093/ejcts/ezaa427
- David T.E. Aortic valve sparing in different aortic valve and aortic root conditions. J Am Coll Cardiol. 2016;68(6):654-664. PMID: 27491910. https://doi.org/10.1016/j.jacc.2016.04.062
- Zakkar M., Youssefi P., Acar C., Khelil N., Debauchez M., Lansac E. Bicuspid aortic valve repair adapted to aortic phenotype. Ann Cardiothorac Surg. 2019;8(3):401-410. PMID: 31240187; PMCID: PMC6562075. https://doi.org/10.21037/acs.2019.04.13
- Holubec T., Zacek P., Jamaliramin M., Emmert M.Y., Tuna M., Nedbal P., Dominik J., Harrer J., Falk V., Vojacek J. Valve cuspidity: a risk factor for aortic valve repair? J Card Surg. 2014;29(5):585-592. PMID: 24919866. https://doi.org/10.1111/jocs.12382
- Safari M., Monsefi N., Karimian-Tabrizi A., Miskovic A., Van Linden A., Zacek P., Moritz A., Walther T., Holubec T. Longer-term outcomes after bicuspid aortic valve repair in 142 patients. J Card Surg. 2021;36(12):4645-4651. PMID: 34547142. https://doi.org/10.1111/jocs.16006
- Bavaria J.E., Desai N., Szeto W.Y., Komlo C., Rhode T., Wallen T., Vallabhajosyula P. Valve-sparing root reimplantation and leaflet repair in a bicuspid aortic valve: comparison with the 3-cusp David procedure. J Thorac Cardiovasc Surg. 2015;149(2 Suppl):S22-S28. PMID: 25500099. https://doi.org/10.1016/j.jtcvs.2014.10.103
- de Meester C., Vanovershelde J.-L., Jahanyar J., Tamer S., Mastrobuoni S., Van Dyck M., Navarra E., Poncelet A., Astarci P., El Khoury G., de Kerchove L. Long-term durability of bicuspid aortic valve repair: a comparison of 2 annuloplasty techniques. Eur J Cardiothorac Surg. 2021;60(2):286-294. PMID: 33495781. https://doi.org/10.1093/ejcts/ezaa471
- Fattouch K., Moscarelli M., Castrovinci S., Murana G., Dioguardi P., Guccione F., Nasso G., Speziale G., Lancellotti P. Mid-term results of bicuspid aortic valve repair guided by morphology and function assessment. Interact Cardiovasc Thorac Surg. 2017;25(1):83-88. PMID: 28379458. https://doi.org/10.1093/icvts/ivx027
- Shrestha M.L., Beckmann E., Abd Alhadi F., Krueger H., Meyer-Bockenkamp F., Bertele S., Koigeldiyev N., Kaufeld T., Fleissner F., Korte W., Schmitto J., Cebotari S., Harringer W., Haverich A., Martens A. Elective David I procedure has excellent long-term results: 20-year single-center experience. Ann Thorac Surg. 2018;105(3):731-738. PMID: 29198631. https://doi.org/10.1016/j.athoracsur.2017.08.040
- Aicher D., Kunihara T., Abou Issa O., Brittner B., Gräber S., Schäfers H.-J. Valve configuration determines long-term results after repair of the bicuspid aortic valve. Circulation. 2011;123(2):178-185. PMID: 21200006. https://doi.org/10.1161/CIRCULATIONAHA.109.934679
- Schneider U., Feldner S.K., Hofmann C., Schöpe J., Wagenpfeil S., Giebels C., Schäfers H.-J. Two decades of experience with root remodeling and valve repair for bicuspid aortic valves. J Thorac Cardiovasc Surg. 2017;153(4):S65-S71. PMID: 28168982. https://doi.org/10.1016/j.jtcvs.2016.12.030
- Mosala Nezhad Z., de Kerchove L., Hechadi J., Tamer S., Boodhwani M., Poncelet A., Noirhomme P., Rubay J., El Khoury G. Aortic valve repair with patch in non-rheumatic disease: indication, techniques and durability. Eur J Cardiothorac Surg. 2014;46(6):997-1005; discussion 1005. PMID: 24618389. https://doi.org/10.1093/ejcts/ezu058
- Sromicki J., Van Hemelrijck M., Schmiady M.O., Greutmann M., Bonassin Tempesta F., Mestres C.A., Vogt P.R., Carrel T.P., Holubec T. Twenty-five year experience with aortic valve-sparing root replacement in a single teaching center. Front Cardiovasc Med. 2023;10:1104149. PMID: 36970369; PMCID: PMC10036903. https://doi.org/10.3389/fcvm.2023.1104149

