Association of GUCY1A3 (rs7692387), CYP2C19*2 (rs4244285), CYP2C19*3 (rs4986893) gene polymorphism with antiplatelet drug metabolism and prognosis of cardiovascular complications: a systematic review
Published 2024-12-27
Keywords
- Aspirin,
- Cardiac Surgical Procedures,
- Clopidogrel,
- Cytochrome P-450 CYP2C19,
- Platelet Aggregation Inhibitors
- Polymorphism, Genetic,
- PubMed ...More
How to Cite
Copyright (c) 2024 Loginova I.Yu., Kurguzov A.V., Isaev A.S., Kamenskaya O.V., Doronin D.V., Klinkova A.S., Chernyavskiy A.M.

This work is licensed under a Creative Commons Attribution 4.0 International License.
Abstract
Introduction: The identification of predictors for resistance to antiplatelet drugs including the search for new gene polymorphisms responsible for the development of the pathological process is an important direction to reduce the risk of complications after cardiac surgery and improve postoperative prognosis.
Objective: The study was aimed at investigating the available data on the molecular genetic markers GUCY1A3 (rs7692387), CYP2C19*2 (rs4244285), CYP2C19*3 (rs4986893) and their association with antiplatelet drug metabolism and adverse outcome after cardiac surgery.
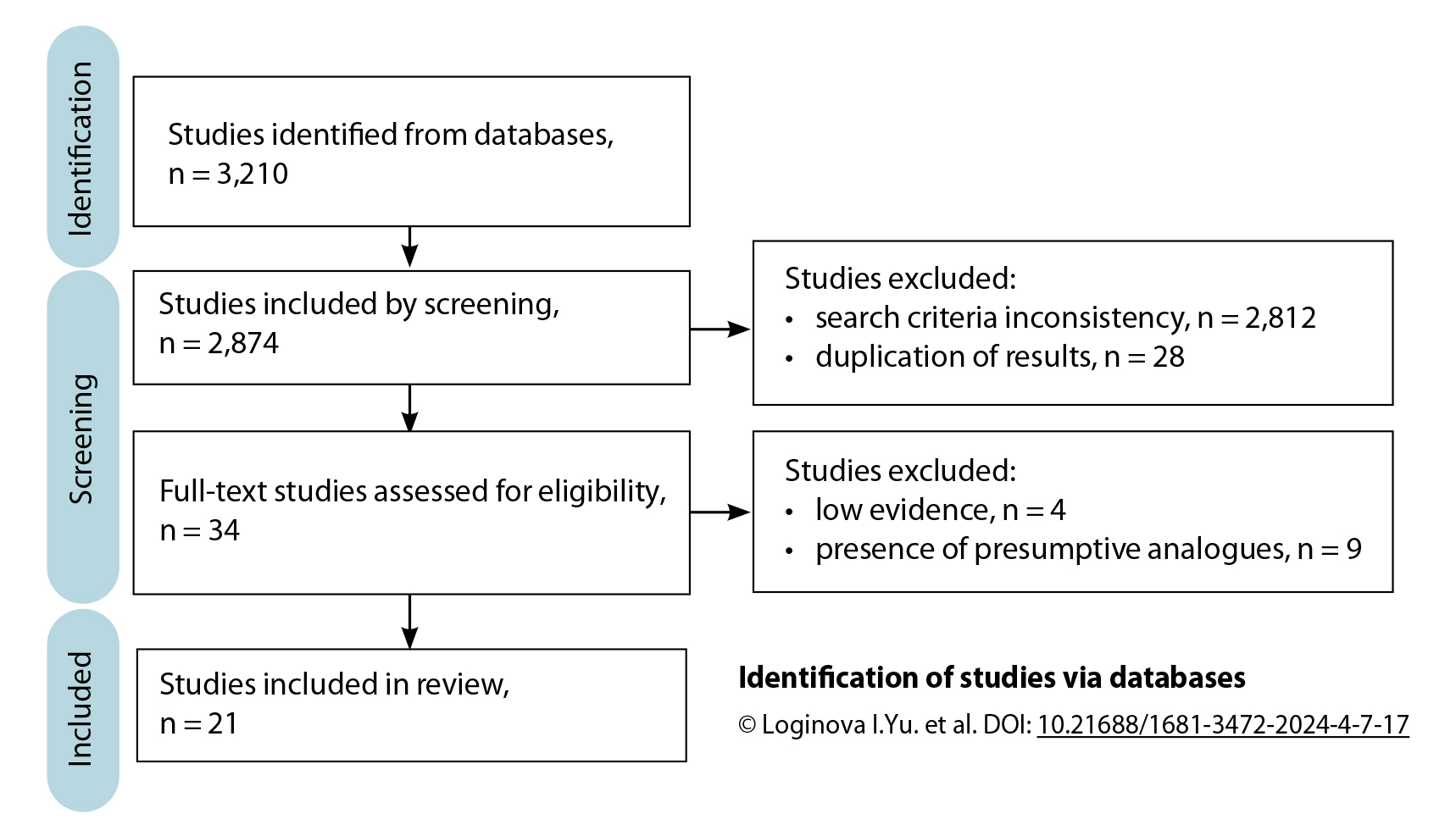
Methods: The systematic review was conducted in accordance with the PRISMA criteria. The search was performed in databases Medline (PubMed), Google Scholar and the Russian Science Citation Index using queries and keywords. During the first selection, 3,210 results were obtained. The final analysis included 21 studies conducted between 2004 and 2024.
Results: Since 2017 a number of studies have revealed the association of GUCY1A3 gene polymorphism with a high risk of cardiovascular diseases, as well as with an abnormal reaction to acetylsalicylic acid. The mechanism of the pathological process was related to the impact of gene polymorphism on vasoreactivity, platelet aggregation and, as a consequence, on the risk of thrombotic complications.
Polymorphisms of CYP2C19*2 and CYP2C19*3 were the most common variants of alleles that reduced clopidogrel metabolism and increased the risk of cardiovascular events. However, therapy based on CYP2C19 genotyping requires a more detailed investigation with the inclusion of ethnic, demographic and socio-economic factors in the analysis.
Conclusion: Resistance to acetylsalicylic acid, clopidogrel and other antiplatelet drugs depends on many genetic factors. Further investigation of the GUCY1A3 and CYP2C19 gene polymorphisms is promising for the development of algorithms for genotype-oriented antiplatelet therapy,
the introduction of which into medical practice will reduce the number of complications after cardiac surgery and improve the quality of medical care.
Received 16 September 2024. Revised 2 November 2024. Accepted 5 November 2024.
Funding
The study did not have sponsorship.
Conflict of interest
The authors declare no conflict of interest.
Contribution of the authors
Conception and study design: A.V. Kurguzov, O.V. Kamenskaya
Data collection and analysis: I.Yu. Loginova, A.S. Isaev, D.V. Doronin
Drafting the article: I.Yu. Loginova, A.S. Klinkova
Critical revision of the article: O.V. Kamenskaya, A.M. Chernyavskiy
Final approval of the version to be published: I.Yu. Loginova, A.V. Kurguzov, A.S. Isaev, O.V. Kamenskaya, D.V. Doronin, A.S. Klinkova, A.M. Chernyavskiy
References
- Neumann F.-J., Sousa-Uva M., Ahlsson A., Alfonso F., Banning A.P., Benedetto U., Byrne R.A., Collet J.-P., Falk V., Head S.J., Jüni P., Kastrati A., Koller A., Kristensen S.D., Niebauer J., Richter D.J., Seferovic P.M., Sibbing D., Stefanini G.G., Windecker S., Yadav R., Zembala M.O.; ESC Scientific Document Group. 2018 ESC/EACTS Guidelines on myocardial revascularization. Eur Heart J. 2019;40(2):87-165. PMID: 30165437. https://doi.org/10.1093/eurheartj/ehy394
- Коротаева Е.С., Королева Л.Ю., Ковалева Г.В., Кузьменко Е.А., Носов В.П. Основные предикторы тромбоза стента у пациентов с острым коронарным синдромом после чрескожного коронарного вмешательства на фоне различной двойной антитромбоцитарной терапии. Кардиология. 2018;58(1S):12-21. https://doi.org/10.18087/cardio.2423 Korotaeva E.S., Koroleva L.Yu., Kovaleva G.V., Kuzmenko E.A., Nosov V.P. Major predictors of stent thrombosis in patients with acute coronary syndrome following transcutaneous coronary intervention who received different double antiplatelet therapy. Kardiologiia = Cardiology. 2018;58(1S):12-21. (In Russ.) https://doi.org/10.18087/cardio.2423
- Wand S., Adam E.H., Wetz A.J., Meybohm P., Kunze-Szikszay N., Zacharowski K., Popov A.F., Moritz A., Moldenhauer L., Kaiser J., Bauer M., Weberet C.F. The prevalence and clinical relevance of ASA nonresponse after cardiac surgery: a prospective bicentric study. Clin Appl Thromb Hemost. 2018;24(1):179-185. PMID: 28301911; PMCID: PMC6714620. https://doi.org/10.1177/1076029617693939
- McLoughlin J., Farrow L., Ashcroft G.P. Prevalence of aspirin resistance among the arthroplasty population: A pilot study. Musculoskeletal Care. 2022;20(3):676-680. PMID: 35170209. https://doi.org/10.1002/msc.1619
- da Silva G.F., Lopes B.M., Moser V., Ferreira L.E. Impact of pharmacogenetics on aspirin resistance: a systematic review. Arq Neuropsiquiatr. 2023;81(1):62-73. PMID: 36918009; PMCID: PMC10014202. https://doi.org/10.1055/s-0042-1758445
- Lordkipanidze M., Pharand C., Schampaert E., Turgeon J., Palisaitis D.A., Diodati J.G. A comparison of six major platelet function tests to determine the prevalence of aspirin resistance in patients with stable coronary artery disease. Eur Heart J. 2007;28(14):1702-1708. PMID: 17569678. https://doi.org/10.1093/eurheartj/ehm226
- Cai G., Zhou W., Lu Y., Chen P., Lu Z., Fu Y. Aspirin resistance and other aspirin-related concerns. Neurol Sci. 2016;37(2):181-189. PMID: 26573589. https://doi.org/10.1007/s10072-015-2412-x
- Wang J., Liu J., Zhou Y., Wang F., Xu K., Kong D., Bai J., Chen J., Gong X., Meng H., Li C. Association among PlA1/A2 gene polymorphism, laboratory aspirin resistance and clinical outcomes in patients with coronary artery disease: An updated meta-analysis. Sci Rep. 2019;9(1):13177. PMID: 31511539; PMCID: PMC6739359. https://doi.org/10.1038/s41598-019-49123-y
- Du G., Lin Q., Wang J. A brief review on the mechanisms of aspirin resistance. Int J Cardiol. 2016;220:21-26. PMID: 27372038. https://doi.org/10.1016/j.ijcard.2016.06.104
- Christopher R., Sundaravadivel P., Chandra S.R., Ramakrishnan S. Platelet ADP receptor (P2RY1) polymorphism and the risk of inadequate platelet response to aspirin: Study in patients with ischemic stroke. Research Square. Epub 2024 Jan 10. https://doi.org/10.21203/rs.3.rs-3836500/v1
- Peng L.-L., Zhao Y.-Q., Zhou Z.-Y., Jin J., Zhao M., Chen X.-M., Chen L.-Y., Cai Y.-F., Li J.-L., Huang M. Associations of MDR1, TBXA2R, PLA2G7, and PEAR1 genetic polymorphisms with the platelet activity in Chinese ischemic stroke patients receiving aspirin therapy. Acta Pharmacol Sin. 2016;37(11):1442-1448. PMID: 27641736; PMCID: PMC5099418. https://doi.org/10.1038/aps.2016.90
- Xue M., Yang X., Yang L., Kou N., Miao Y., Wang M., Ren J., Zhao Q. rs5911 and rs3842788 genetic polymorphism, blood stasis syndrome, and plasma TXB2 and hs‐CRP levels are associated with aspirin resistance in Chinese chronic stable angina patients. Evid Based Complement Alternat Med. 2017;2017:9037094. PMID: 28465708; PMCID: PMC5390593. https://doi.org/10.1155/2017/9037094
- Ferreira M., Freitas-Silva M., Assis J., Pinto R., Nunes J.P., Medeiros R. The emergent phenomenon of aspirin resistance: Insights from genetic association studies. Pharmacogenomics. 2020;21(2):125-140. PMID: 31957546. https://doi.org/10.2217/pgs-2019-0133
- Wolf B., Kessler T., Schunkert H. Genetik der koronaren Herzkrankheit. Aktuelle Kardiologie. 2018;7(03):197-203. https://doi.org/10.1055/a-0624-1871
- Kessler T., Wobst J., Wolf B., Eckhold J., Vilne B., Hollstein R., Ameln S., Dang T.A., Sager H.B., Rumpf P.M., Aherrahrou R., Kastrati A., Björkegren J.L.M., Erdmann J., Lusis A.J., Civelek M., Kaiser F.J., Schunkert H. Functional characterization of the GUCY1A3 coronary artery disease risk locus. Circulation. 2017;136(5):476-489. PMID: 28487391; PMCID: PMC5560301. https://doi.org/10.1161/circulationaha.116.024152
- Malinowski D., Zawadzka M., Safranow K., Droździk M., Pawlik A. SELL and GUCY1A1 gene polymorphisms in patients with unstable angina. Biomedicines. 2022;10(10):2494. PMID: 36289756; PMCID: PMC9598954. https://doi.org/10.3390/biomedicines10102494
- Жабин С.Н., Лазаренко В.А., Черноусова С.С., Башкатов Д.А., Азарова Ю.Э., Клёсова Е.Ю., Быканова М.А., Полоников А.В. Полиморфизм rs7692387 гена GUCY1A1 – генетический маркер развития облитерирующего атеросклероза у курильщиков. Ангиология и сосудистая хирургия. Журнал имени академика А.В. Покровского. 2022;28(2):36-42. https://doi.org/10.33029/1027-6661-2022-28-2-36-42 Zhabin S.N., Lazarenko V.A., Chernousova S.S., Bashkatov D.A., Azarova Yu.E., Kolesova E.Yu., Bykanova M.A., Polonikov A.V. Polymorphism rs7692387 of GUCY1A1 as a genetic marker for peripheral artery disease in cigarette smokers. Angiology and Vascular Surgery. Journal named after Academician A.V. Pokrovsky. 2022;28(2):36-42. (In Russ.) https://doi.org/10.33029/1027-6661-2022-28-2-36-42
- Friede K.A., Voora D. Genetic influences on aspirin response in patients undergoing percutaneous coronary intervention. Cardiovasc Res. 2019;115(10):1452-1453. PMID: 31049556; PMCID: PMC6933505. https://doi.org/10.1093/cvr/cvz110
- Kessler T., Wolf B., Eriksson N., Kofink D., Mahmoodi B.K., Rai H., Tragante V., Åkerblom A., Becker R.C., Bernlochner I., Bopp R., James S., Katus H.A., Mayer K., Munz M., Nordio F., O’Donoghue M.L., Sager H.B., Sibbing D., Solakov L., Storey R.F., Wobst J., Asselbergs F.W., Byrne R.A., Erdmann J., Koenig W., Laugwitz K.-L., Ten Berg J.M., Wallentin L., Kastrati A., Schunkert H. Association of the coronary artery disease risk gene GUCY1A3 with ischaemic events after coronary intervention. Cardiovasc Res. 2019;115(10):1512-1518. PMID: 30768153. https://doi.org/10.1093/cvr/cvz015
- Li J.-L., Liu L.-Y., Jiang D.-D., Jiang Y.-Y., Zhou G.-Q., Mo D.-C., Luo M. Associations between GUCY1A3 genetic polymorphisms and large artery atherosclerotic stroke risk in Chinese Han population: a case-control study. Lipids Health Dis. 2019;18(1):233. PMID: 31883534; PMCID: PMC6935057. https://doi.org/10.1186/s12944-019-1177-2
- Hall K.T., Kessler T., Buring J.E., Passow D., Sesso H.D., Zee R.Y.L., Ridker P.M., Chasman D.I., Schunkert H. Genetic variation at the coronary artery disease risk locus GUCY1A3 modifies cardiovascular disease prevention effects of aspirin. Eur Heart J. 2019;40(41):3385-3392. PMID: 31228190; PMCID: PMC6933533. https://doi.org/10.1093/eurheartj/ehz384
- Pradhan A., Bhandari M., Vishwakarma P., Sethi R. Clopidogrel resistance and its relevance: Current concepts. J Family Med Prim Care. 2024;13(6):2187-2199. PMID: 39027844; PMCID: PMC11254075. https://doi.org/10.4103/jfmpc.jfmpc_1473_23
- Kirac D., Yaman A.E., Doran T., Mihmanli M., Keles E.C. COX-1, COX-2 and CYP2C19 variations may be related to cardiovascular events due to acetylsalicylic acid resistance. Mol Biol Rep. 2022;49(4):3007-3014. PMID: 35000048. https://doi.org/10.1007/s11033-022-07124-7
- Cavallari L.H., Lee C.R., Beitelshees A.L., Cooper-DeHoff R.M., Duarte J.D., Voora D., Kimmel S.E., McDonough C.W., Gong Y., Dave C.V., Pratt V.M., Alestock T.D., Anderson R.D., Alsip J., Ardati A.K., Brott B.C., Brown L., Chumnumwat S., Clare-Salzler M.J., Coons J.C., Denny J.C., Dillon C., Elsey A.R., Hamadeh I.S., Harada S., Hillegass W.B., Hines L., Horenstein R.B., Howell L.A., Jeng L.J.B., Kelemen M.D., Lee Y.M., Magvanjav O., Montasser M., Nelson D.R., Nutescu E.A., Nwaba D.C., Pakyz R.E., Palmer K., Peterson J.F., Pollin T.I., Quinn A.H., Robinson S.W., Schub J., Skaar T.C., Smith D.M., Sriramoju V.B., Starostik P., Stys T.P., Stevenson J.M., Varunok N., Vesely M.R., Wake D.T., Weck K.E., Weitzel K.W., Wilke R.A., Willig J., Zhao R.Y., Kreutz R.P., Stouffer G.A., Empey P.E., Limdi N.A., Shuldiner A.R., Winterstein A.G., Johnson J.A.; IGNITE Network. Multisite investigation of outcomes with implementation of CYP2C19 genotype-guided antiplatelet therapy after percutaneous coronary intervention. JACC Cardiovasc Interv. 2018;11(2):181-191. PMID: 29102571; PMCID: PMC5775044. https://doi.org/10.1016/j.jcin.2017.07.022
- Shen D.-L., Wang B., Bai J., Han Q., Liu C., Huang X.-H., Zhang J.-Y. Clinical value of CYP2C19 genetic testing for guiding the antiplatelet therapy in a Chinese population. J Cardiovasc Pharmacol. 2016;67:232-236. PMID: 26727381. https://doi.org/10.1097/fjc.0000000000000337
- Xie X., Ma Y.-T., Yang Y.-N., Li X.-M., Zheng Y.-Y., Ma X., Fu Z.-Y., Ba Bayinsilema, Li Y., Yu Z.-X., Chen Y., Chen B.-D., Liu F., Huang Y., Liu C., Baituola G. Personalized antiplatelet therapy according to CYP2C19 genotype after percutaneous coronary intervention: a randomized control trial. Int J Cardiol. 2013;168(4):3736-3740. PMID: 23850318. https://doi.org/10.1016/j.ijcard.2013.06.014
- Castrichini M., Luzum J.A., Pereira N. Pharmacogenetics of antiplatelet therapy. Annu Rev Pharmacol Toxicol. 2023;63:211-229. PMID: 35914768; PMCID: PMC9868113. https://doi.org/10.1146/annurev-pharmtox-051921-092701
- Liu J., Zhao Y., Chen H., Yang F., Chen L., Hao G., Gao X. Relationship between recurrent ischemic events in cerebrovascular disease and cytochrome P450 2C19 gene polymorphism on the basis of thrombelastography. Ann Palliat Med. 2022;11(1):240-249. PMID: 35144415. https://doi.org/10.21037/apm-21-3775
- Li L., Luo S. Analysis of CYP2C19 gene genotype in patients with acute cerebral infarction and its relationship with disease progression. Russ J Genet. 2023;59:1092-1097. https://doi.org/10.1134/S1022795423100083
- Cheng Y., Sun Y., Zhang D., Ma X., Liu C., Hu C., Sun T., Zhao Z., Liu X., Zhou Y. Influence of CYP2C19 genetic variants and smoking on dual antiplatelet efficacy in patients with coronary artery disease. Front Cardiovasc Med. 2023;10:1105001. PMID: 36760562; PMCID: PMC9902702. https://doi.org/10.3389/fcvm.2023.1105001
- Li W., Yang X., Chen J., Zhu J.-W., Zeng L.-H., Long H.-H., Chen Z., Tang J., Lan X.-F. The association between CYP2C19 genetic polymorphism and prognosis in patients receiving endovascular therapy. Ann Indian Acad Neurol. 2024;27(1):27-33. PMID: 38495252; PMCID: PMC10941889. https://doi.org/10.4103/aian.aian_564_23
- Marcucci R., Berteotti M., Gragnano F., Galli M., Cavallari I., Renda G., Capranzano P., Santilli F., Capodanno D., Angiolillo D.J., Cirillo P., Calabrò P., Patti G., De Caterina R. Monitoring antiplatelet therapy: where are we now? J Cardiovasc Med. 2023;24(Suppl 1):e24-e35. https://doi.org/10.2459/jcm.0000000000001406
- Aftab Siddiqui M., Jain C., Usmani A., Hafeez A., Khalid M., Mujahid M. Pharmacogenetics and pharmacogenomics impact on aspirin response. In: Khullar M., Mittal A., Patil A., editors. Pharmacogenomics and Pharmacogenetics in Drug Therapy. IntechOpen, 2024. 116 p. https://doi.org/10.5772/intechopen.113026
- Nguyen A.B., Cavallari L.H., Rossi J.S., Stouffer G.A., Lee C.R. Evaluation of race and ethnicity disparities in outcome studies of CYP2C19 genotype-guided antiplatelet therapy. Front Cardiovasc Med. 2022;9:991646. PMID: 36082121; PMCID: PMC9445150. https://doi.org/10.3389/fcvm.2022.991646
- Krishnan K., Nguyen T.N., Appleton J.P., Law Z.K., Caulfied M., Cabrera C.P., Lenthall R., Hewson D., England T., McConachie N., Dhillon P., Malik L., Podlasek A., Smith C.J., Dawson J., Robinson T.G., Sprigg N., James M.A., White P., Desborough M.J.R., Hermans J., Bath P.M. Antiplatelet resistance: A review of concepts, mechanisms, and implications for management in acute ischemic stroke and transient ischemic attack. Stroke: Vascular and Interventional Neurology. 2023;3(3):e000576. https://doi.org/10.1161/svin.122.000576
- Ogweno G., Kimathi E. Emerging clinical problem of resistance to antiplatelet therapy in primary prevention and treatment of cardiovascular events in people living with HIV: Conundrum despite effective cART. In: Okware S., editor. HIV Treatment — New Development. IntechOpen, 2024. 116 p. https://doi.org/10.5772/intechopen.112500
- Семащенко К.С., Монгуш Т.С., Косинова А.А., Субботина Т.Н., Гринштейн Ю.И. Изучение ассоциации нуклеотидных полиморфизмов в генах тромбоцитарных рецепторов и цитохрома Р450 с развитием резистентности к антитромбоцитарным препаратам у пациентов с ишемической болезнью сердца. Рациональная фармакотерапия в кардиологии. 2022;18(3):289-296. https://doi.org/10.20996/1819-6446-2022-06-15 Semashchenko K.S., Mongush T.S., Kosinova A.A., Subbotina T.N., Grinshtein Y.I. Study the association of nucleotide polymorphisms in platelet receptor and cytochrome P450 genes with the development of resistance to antiplatelet drugs in patients with coronary artery disease. Rational Pharmacotherapy in Cardiology. 2022;18(3):289-296. (In Russ.) https://doi.org/10.20996/1819-6446-2022-06-15
- Якуббеков Н.Т., Муллабаева Г.У., Абдуллаева С.Я., Никишин А.Г. Сравнительный анализ степени и скорости агрегации тромбоцитов на терапии клопидогрелем и прасугрелем с учетом G681A гена CYP2C19 у больных с многососудистом поражением коронарного русла. Высшая школа. 2022;(10):57-61. Yakubbekov N.T., Mullabaeva G.U., Abdullaeva S.Ya., Nikishin A.G. Comparative analysis of the degree and rate of platelet aggregation on therapy with clopidogrel and prasugrel, taking into account G681A of the CYP2C19 gene in patients with multivessel coronary disease. Vysshaya shkola = Higher School. 2022;(10):57-61. (In Russ.)
- Пронько Т.П., Снежицкий В.А., Степуро Т.Л., Копыцкий А.В. Ассоциация полиморфных вариантов генов CYP2C19, P2RY12, ITGB3, ITGA2 и eNOS3 с высокой остаточной реактивностью тромбоцитов на фоне приема клопидогрела и ацетилсалициловой кислоты в разные сроки инфаркта миокарда. Рациональная фармакотерапия в кардиологии. 2023;19(3):222-229. https://doi.org/10.20996/1819-6446-2023-2904 Pronko T.P., Snezhitskiy V.A., Stepuro T.L., Kapytski A.V. Association of polymorphic variants of CYP2C19, P2RY12, ITGB3, ITGA2 and eNOS3 genes with high residual platelet reactivity while taking clopidogrel and acetylsalicylic acid at different terms of myocardial infarction. Rational Pharmacotherapy in Cardiology. 2023;19(3):222-229. (In Russ.) https://doi.org/10.20996/1819-6446-2023-2904
- Tuteja S., Glick H., Matthai W., Nachamkin I., Nathan A., Monono K., Carcuffe C., Maslowski K., Chang G., Kobayashi T., Anwaruddin S., Hirshfeld J., Wilensky R.L., Herrmann H.C., Kolansky D.M., Rader D.J., Giri J. Prospective CYP2C19 genotyping to guide antiplatelet therapy following percutaneous coronary intervention. Circ Genom Precis Med. 2020;13(1):11-19. PMID: 31928229. https://doi.org/10.1161/circgen.119.002640
- Claassens D.M.F., Vos G.J.A., Bergmeijer T.O., Hermanides R.S., van ’t Hof A.W.J., van der Harst P., Barbato E., Morisco C., Tjon Joe Gin R.M., Asselbergs F.W., Mosterd A., Herrman J.-R., Dewilde W.J.M., Janssen P.W.A., Kelder J.C., Postma M.J., de Boer A., Boersma C., Deneer V.H.M., Ten Berg J.M. A genotype-guided strategy for oral P2Y12 inhibitors in primary PCI. N Eng J Med. 2019;381(17):1621-1631. PMID: 31479209. https://doi.org/10.1056/nejmoa1907096
- Pereira N.L., Farkouh M.E., So D., Lennon R., Geller N., Mathew V., Bell M., Bae J.-H., Jeong M.H., Chavez I., Gordon P., Abbott J.D., Cagin C., Baudhuin L., Fu Y.-P., Goodman S.G., Hasan A., Iturriaga E., Lerman A., Sidhu M., Tanguay J.-F., Wang L., Weinshilboum R., Welsh R., Rosenberg Y., Bailey K., Rihal C. Effect of genotype-guided oral P2Y12 inhibitor selection vs conventional clopidogrel therapy on ischemic outcomes after percutaneous coronary intervention: The TAILOR-PCI randomized clinical trial. JAMA. 2020;324(8):761-771. PMID: 32840598; PMCID: PMC7448831. https://doi.org/10.1001/jama.2020.12443
- Мальцева А.Н., Гринштейн Ю.И. Недостаточный ответ тромбоцитов на применение ацетилсалициловой кислоты и клопидогрела при ишемической болезни сердца после коронарной реваскуляризации. Является ли резистентность к антитромбоцитарным препаратам обратимой? РМЖ. 2021;9:1-5. Maltseva A.N., Grinshtein Yu.I. Lack of platelet response to the use of acetylsalicylic acid and clopidogrel in coronary heart disease after coronary revascularization. Is resistance to antiplatelet drugs reversible? RMJ. 2021;9:1-5. (In Russ.)

