Coronary microvascular obstruction in percutaneous coronary interventions in myocardial infarction patients: a comprehensive approach to prevention and treatment
Published 2024-11-08
Keywords
- Cohort Studies,
- Multivariate Analysis,
- Myocardial Infarction,
- No-Reflow Phenomenon,
- Percutaneous Coronary Intervention
- ST Elevation Myocardial Infarction ...More
How to Cite
Copyright (c) 2024 Frolov A.A., Pochinka I.G., Frolov I.A., Kuzmichev K.V., Mukhin A.S., Sharabrin E.G.

This work is licensed under a Creative Commons Attribution 4.0 International License.
Abstract
Objective: The study intends to evaluate the prognostic value of a comprehensive approach to prevention and treating the coronary microvascular obstruction (CMVO) upon percutaneous coronary interventions (PCI) in patients with ST-segment elevation myocardial infarction (STEMI).
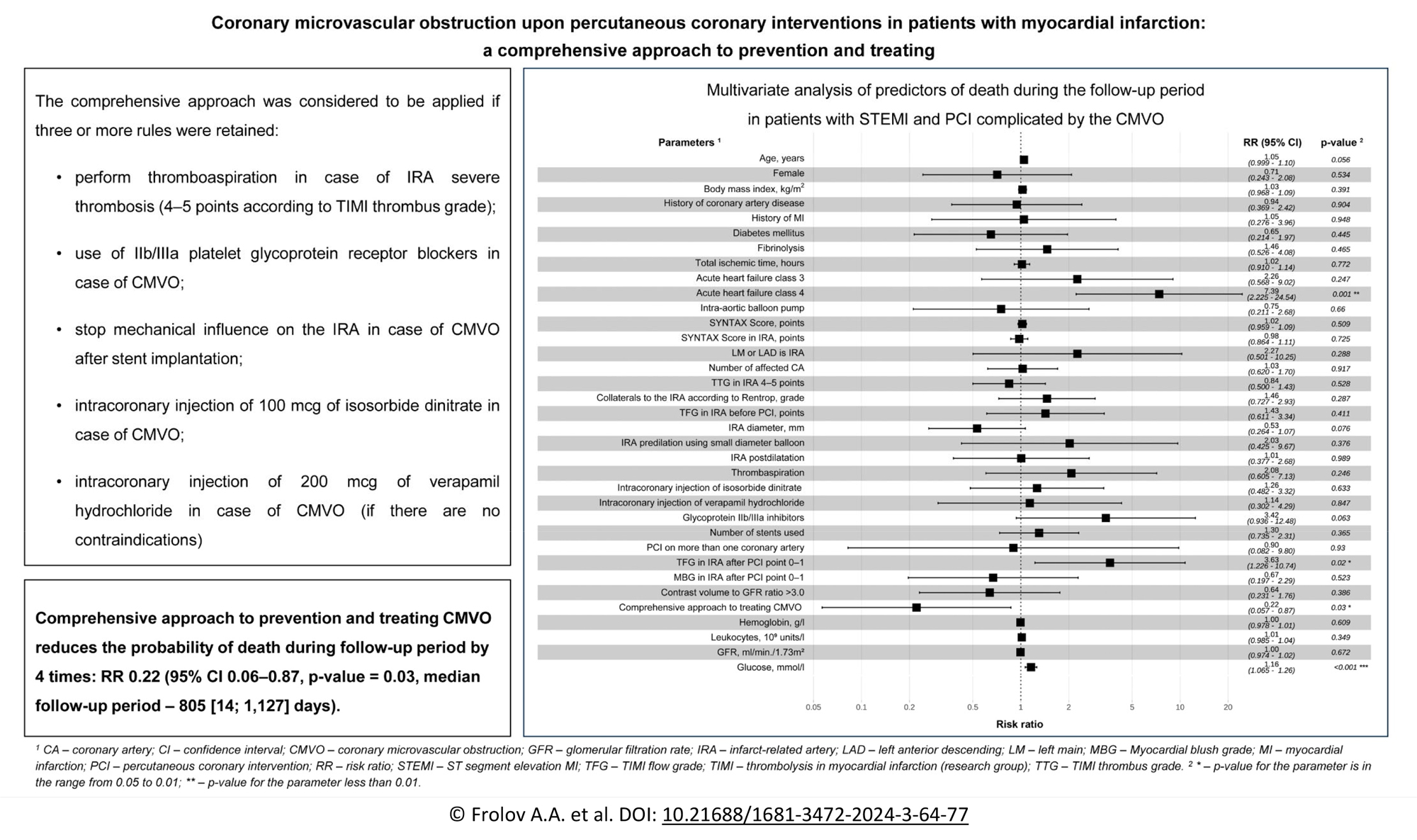
Methods: A single-center cohort study was conducted in patients characterizing by type 1 STEMI, emergency PCI, a total ischemic time of less than 12 hours, and the development of CMVO (TIMI flow grade < 3 or Myocardial blush grade < 2). Patients with cardiogenic shock prior to PCI were excluded. A proposed comprehensive approach included the following five rules: thromboaspiration in case of severe thrombosis, platelet glycoprotein IIb/IIIa receptor blockers, "minimally invasive PCI," intracoronary administration of isosorbide dinitrate and verapamil hydrochloride upon the development of CMVO. The approach was considered to be applied if three or more rules were retained. The median follow-up period was 805 [14; 1,127] days. A multivariate analysis of the risk of long-term mortality was performed using the Cox proportional hazards model.
Results: A total of 202 patients were included in the study and 53 (26.3%) of them had a fatal outcome; in particular, 16 (7.9%) patients died at the hospital stage and 27 (13.4%) after discharge. Multivariate analysis of predictors of mortality showed that the using of a comprehensive approach to prevention and treating CMVO reduces the probability of death during follow-up period by 4 times with risk ratio 0.22, 95% confidence interval 0.06–0.87 and p = 0.03.
Conclusion: The introducing of the proposed comprehensive approach to prevention and treating CMVO upon PCI in patients with STEMI is associated with a lower probability of death within 805 days after the intervention.
Received 30 July 2024. Revised 25 September 2024. Accepted 1 October 2024.
Funding
The study did not have sponsorship.
Conflict of interest
The authors declare no conflict of interest.
Contribution of the authors
Conception and study design: A.A. Frolov, E.G. Sharabrin, I.G. Pochinka
Data collection and analysis: A.A. Frolov, I.A. Frolov, K.V. Kuzmichev
Statistical analysis: A.A. Frolov, I.A. Frolov, K.V. Kuzmichev
Drafting the article: A.A. Frolov, I.G. Pochinka, I.A. Frolov
Critical revision of the article: I.G. Pochinka, A.S. Mukhin, E.G. Sharabrin
Final approval of the version to be published: A.A. Frolov, I.G. Pochinka, I.A. Frolov, K.V. Kuzmichev, A.S. Mukhin, E.G. Sharabrin
References
- Гиляров М.Ю., Иванов И.И., Константинова Е.В., Расчётнова Н.И., Шостак Н.А. Феномен no-reflow и реперфузионное повреждение миокарда: механизмы и методы лечения. Клиницист. 2021;15(1-4):10-19. https://doi.org/10.17650/1818-8338-2021-15-1-4-K645 Gilyarov M.Yu., Ivanov I.I., Konstantinova E.V., Raschetnova N.I., Shostak N.A. No-reflow phenomenon and reperfusion injury. Mechanisms and treatment. The Clinician. 2021;15(1-4):10-19. (In Russ.) https://doi.org/10.17650/1818-8338-2021-15-1-4-K645
- Byrne R.A., Rossello X., Coughlan J.J., Barbato E., Berry C., Chieffo A., Claeys M.J., Dan G.A., Dweck M.R., Galbraith M., Gilard M., Hinterbuchner L., Jankowska E.A., Jüni P., Kimura T., Kunadian V., Leosdottir M., Lorusso R., Pedretti R.F.E., Rigopoulos A.G., Rubini Gimenez M., Thiele H., Vranckx P., Wassmann S., Wenger N.K., Ibanez B.; ESC Scientific Document Group. 2023 ESC Guidelines for the management of acute coronary syndromes. Eur Heart J. 2023;44(38):3720-3826. PMID: 37622654. https://doi.org/10.1093/eurheartj/ehad191
- Фролов А.А., Фролов И.А., Уланова Н.Д., Починка И.Г., Кузьмичев К.В., Мухин А.С., Шарабрин Е.Г. Фенотипы синдрома коронарной микрососудистой обструкции (no-reflow), развивающегося в ходе выполнения чрескожных коронарных вмешательств при инфаркте миокарда. Бюллетень сибирской медицины. 2023;22(4):137-146. https://doi.org/10.20538/1682-0363-2023-4-137-146 Frolov A.A., Frolov I.A., Ulanova N.D., Pochinka I.G., Kuzmichev K.V., Mukhin A.S., Sharabrin E.G. Phenotypes of coronary microvascular obstruction phenomenon (no-reflow) during percutaneous coronary interventions in myocardial infarction. Bulletin of Siberian Medicine. 2023;22(4):137-146. (In Russ.) https://doi.org/10.20538/1682-0363-2023-4-137-146
- Журавлев А.С., Азаров А.В., Семитко С.П., Иоселиани Д.Г. Феномен no-reflow во время первичного чрескожного коронарного вмешательства у пациентов с острым инфарктом миокарда с подъемом сегмента ST, обусловленным массивным коронарным тромбозом. Патогенез и предикторы no-reflow. Кардиология. 2021;61(2):99-105. https://doi.org/10.18087/cardio.2021.2.n1175 Zhuravlev A.S., Azarov A.V., Semitko S.P., Ioseliani D.G. The no-reflow phenomenon during primary percutaneous coronary intervention in patients with ST-segment elevation myocardial infarction due to massive coronary thrombosis. Pathogenesis and predictors of no-reflow. Kardiologiia. 2021;61(2):99-105. (In Russ.) https://doi.org/10.18087/cardio.2021.2.n1175
- Kaur G., Baghdasaryan P., Natarajan B., Sethi P., Mukherjee A., Varadarajan P., Pai R.G. Pathophysiology, diagnosis, and management of coronary no-reflow phenomenon. Int J Angiol. 2021;30(1):15-21. PMID: 34025092. PMCID: PMC8128485. https://dx.doi.org/10.1055/s-0041-1725979
- Фролов А.А., Починка И.Г., Шахов Б.Е., Шарабрин Е.Г., Кузьмичев К.В. Феномен коронарной микрососудистой обструкции (no-reflow) при проведении чрескожных коронарных вмешательств у пациентов с инфарктом миокарда. Патология кровообращения и кардиохирургия. 2020;24(1):18-27. https://doi.org/10.21688/1681-3472-2020-1-18-27 Frolov A.A., Pochinka I.G., Shahov B.E., Sharabrin E.G., Kuzmichev K.V. Coronary microvascular obstruction (the no-reflow phenomenon) during percutaneous coronary interventions in patients with myocardial infarction. Patologiya krovoobrashcheniya i kardiokhirurgiya = Circulation Pathology and Cardiac Surgery. 2020;24(1):18-27. (In Russ.) https://doi.org/10.21688/1681-3472-2020-1-18-27
- Ndrepepa G., Kastrati A. Coronary No-reflow after primary percutaneous coronary intervention-current knowledge on pathophysiology, diagnosis, clinical impact and therapy. J Clin Med. 2023;12(17):5592. PMID: 37685660. PMCID: PMC10488607. https://doi.org/10.3390/jcm12175592
- Konijnenberg L.S.F., Damman P., Duncker D.J., Kloner R.A., Nijveldt R., van Geuns R.M., Berry C., Riksen N.P., Escaned J., van Royen N. Pathophysiology and diagnosis of coronary microvascular dysfunction in ST-elevation myocardial infarction. Cardiovasc Res. 2020;116(4):787-805. PMID: 31710673. PMCID: PMC7061278. https://doi.org/10.1093/cvr/cvz301
- Khalfallah M., Allaithy A., Maria D.A. Impact of the total ischemia time on no-reflow phenomenon in patients with ST elevation myocardial infarction undergoing primary percutaneous coronary intervention. Anatol J Cardiol. 2022;26(5):382-387. PMID: 35552174. PMCID: PMC9366414. https://doi.org/10.5152/AnatolJCardiol.2021.846
- Antonopoulos A.S., Simantiris S., Tousoulis D. Thrombus aspiration in STEMI: Whom we aspire it may help? Int J Cardiol. 2024;399:131671. PMID: 38216061. https://doi.org/10.1016/j.ijcard.2023.131671
- Kirresh A., Candilio L., Stone G.W. Intralesional delivery of glycoprotein IIb/IIIa inhibitors in acute myocardial infarction: review and recommendations. Catheter Cardiovasc Interv. 2022;99(3):641-649. PMID: 34767293. https://doi.org/10.1002/ccd.30008
- Karamasis G.V., Kalogeropoulos A.S., Gamma R.A., Clesham G.J., Marco V., Tang K.H., Jagathesan R., Sayer J.W., Robinson N.M., Kabir A., Aggarwal R.K., Kelly P.A., Prati F., Keeble T.R., Davies J.R. Effects of stent postdilatation during primary PCI for STEMI: Insights from coronary physiology and optical coherence tomography. Catheter Cardiovasc Interv. 2021;97(7):1309-1317. PMID: 35265354. PMCID: PMC8858403. https://doi.org/10.1002/ccd.28932
- Dawson L.P., Rashid M., Dinh D.T., Brennan A., Bloom J.E., Biswas S., Lefkovits J., Shaw J.A., Chan W., Clark D.J., Oqueli E., Hiew C., Freeman M., Taylor A.J., Reid C.M., Ajani A.E., Kaye D.M., Mamas M.A., Stub D.; MIG and BCIS Investigators. No-reflow prediction in acute coronary syndrome during percutaneous coronary intervention: The NORPACS Risk Score. Circ Cardiovasc Interv. 2024;17(4):e013738. PMID: 38487882. https://doi.org/10.1161/circinterventions.123.013738
- Li X., Sun S., Luo D., Yang X., Ye J., Guo X., Xu S., Sun B., Zhang Y., Luo J., Zhou Y., Tu S., Dong H. Microvascular and prognostic effect in lesions with different stent expansion during primary PCI for STEMI: insights from coronary physiology and intravascular ultrasound. Front Cardiovasc Med. 2022;9:816387. PMID: 35355977. PMCID: PMC8959302. https://doi.org/10.3389/fcvm.2022.816387
- Xu X., Zhou J., Zhang Y., Li Q., Guo L., Mao Y., He L. Evaluate the correlation between the TIMI Frame Count, IMR, and CFR in coronary microvascular disease. J Interv Cardiol. 2022;2022:6361398. PMID: 35185397. PMCID: PMC8828352. https://doi.org/10.1155/2022/6361398
- Hamza M., Elgendy I.Y. Intracoronary eptifibatide with vasodilators to prevent no-reflow in diabetic STEMI with high thrombus burden. A randomized trial. Rev Esp Cardiol. 2022;75(9):727-733. PMID: 35039226. https://doi.org/10.1016/j.rec.2021.10.012
- Arab T.A., Sedhom R., Gomaa Y., el Etriby A. Intracoronary adenosine compared with adrenaline and verapamil in the treatment of no-reflow phenomenon following primary PCI in STEMI patients. Int J Cardiol. 2024;410:132228. PMID: 38844092. https://doi.org/10.1016/j.ijcard.2024.132228
- Мазнев Д.С., Болдуева С.А., Леонова И.А. Мануальная тромбаспирация как метод профилактики феномена no-reflow. Дальневосточный медицинский журнал. 2019;(4):81-85. https://doi.org/10.35177/1994-5191-2019-4-81-86 Maznev D.S., Boldueva S.А., Leonova I.А. Manual thromboaspiration as a method of prevention on no-reflow phenomenon. Far East Medical Journal. 2019;(4):81-85. (In Russ.) https://doi.org/10.35177/1994-5191-2019-4-81-86
- Zeng Q., Zhang L.D., Wang W. A meta-analysis of randomized controlled trials investigating tirofiban combined with conventional drugs by intracoronary administration for no-reflow prevention. Anatol J Cardiol. 2021;25(1):7-16. PMID: 33382055. PMCID: PMC7803802. https://dx.doi.org/10.14744/anatoljcardiol.2020.99469
- Mueller H.S., Dyer A., Greenberg M.A., The TIMI Study Group. The Thrombolysis in Myocardial Infarction (TIMI) trial. Phase I findings. N Engl J Med. 1985;312(14):932-936. PMID: 4038784. https://doi.org/10.1056/nejm198504043121437
- van ‘t Hof A.W., Liem A., Suryapranata H., Hoorntje J.C., de Boer M.J., Zijlstra F. Zwolle Myocardial Infarction Study Group. Angiographic assessment of myocardial reperfusion in patients treated with primary angioplasty for acute myocardial infarction: myocardial blush grade. Circulation. 1998;97(23):2302-2306. PMID: 9639373. https://doi.org/10.1161/01.cir.97.23.2302
- Killip T. 3rd, Kimball J.T. Treatment of myocardial infarction in a coronary care unit. A two year experience with 250 patients. Am J Cardiol. 1967;20(4):457-464. PMID: 6059183. https://doi.org/10.1016/0002-9149(67)90023-9
- Sianos G., Papafaklis M.I., Serruys P.W. Angiographic thrombus burden classification in patients with ST-segment elevation myocardial infarction treated with percutaneous coronary intervention. J Invasive Cardiol. 2010;22(10 Suppl B):6B-14B. PMID: 20947930.
- Rentrop K.P., Feit F., Sherman W., Thornton J.C. Serial angiographic assessment of coronary artery obstruction and collateral flow in acute myocardial infarction. Report from the second Mount Sinai-New York University Reperfusion Trial. Circulation. 1989;80(5):1166-1175. PMID: 2509103. https://doi.org/10.1161/01.cir.80.5.1166
- Sianos G., Morel M.A., Kappetein A.P., Morice M.C., Colombo A., Dawkins K., van den Brand M., Van Dyck N., Russell M.E., Mohr F.W., Serruys P.W. The SYNTAX Score: an angiographic tool grading the complexity of coronary artery disease. EuroIntervention. 2005;1(2):219-227. PMID: 19758907.
- van der Molen A.J., Reimer P., Dekkers I.A., Bongartz G., Bellin M.F., Bertolotto M., Clement O., Heinz-Peer G., Stacul F., Webb J.A.W., Thomsen H.S. Post-contrast acute kidney injury – Part 1: Definition, clinical features, incidence, role of contrast medium and risk factors: recommendations for updated ESUR Contrast Medium Safety Committee guidelines. Eur Radiol. 2018;28(7):2845-2855. PMID: 29426991. PMCID: PMC5986826. https://doi.org/10.1007/s00330-017-5246-5
- Austin P.C., White I.R., Lee D.S., van Buuren S. Missing data in clinical research: a tutorial on multiple imputation. Can J Cardiol. 2021;37(9):1322-1331. PMID: 33276049. PMCID: PMC8499698. https://doi.org/10.1016/j.cjca.2020.11.010
- Фролов А.А., Починка И.Г., Фролов И.А., Кузьмичев К.В., Мухин А.С., Шарабрин Е.Г., Синютин В.Н. Шкала оценки тяжести коронарной микрососудистой обструкции (no-reflow) при чрескожных коронарных вмешательствах у пациентов с инфарктом миокарда. Патология кровообращения и кардиохирургия. 2023;7(4):52-63. https://doi.org/10.21688/1681-3472-2023-4-52-63 Frolov A.A., Pochinka I.G., Frolov I.A., Kuzmichev K.V., Mukhin A.S., Sharabrin E.G., Sinyutin V.N. Severity scale of coronary microvascular obstruction (no-reflow) during percutaneous coronary interventions in myocardial infarction patients. Patologiya krovoobrashcheniya i kardiokhirurgiya = Circulation Pathology and Cardiac Surgery. 2023;27(4):52-63. (In Russ.) https://doi.org/10.21688/1681-3472-2023-4-52-63
- Вышлов Е.В., Диль С.В., Баев А.Е., Гергерт Е.С., Пекарский С.Е., Рябов В.В. интракоронарное введение эпинефрина при рефрактерном феномене no-reflow у пациентов с острым инфарктом миокарда. Кардиология. 2024:64(6):34-42. https://doi.org/10.18087/cardio.2024.6.n2493 Vyshlov E.V., Dil S.V., Baev А.Е., Gergert Е.S., Pekarsky S.E., Ryabov V.V. Intracoronary administration of epinephrine in the refractory no-reflow phenomenon in patients with acute myocardial infarction. Kardiologiia. 2024;64(6):34-42. (In Russ.) https://doi.org/10.18087/cardio.2024.6.n2493
- Rigattieri S., Lettieri C., Tiberti G., Romano M., Ferlini M., Testa L., Pierini S., Ettori F., Passamonti E., Marchese A., Musumeci G., Esposito G., Tarantini G. Primary percutaneous coronary intervention with high-bolus dose tirofiban: the FASTER (Favorite Approach to Safe and effective Treatment for Early Reperfusion) multicenter registry. J Interv Cardiol. 2022;2022:9609970. PMID: 35418809. PMCID: PMC8983258. https://doi.org/10.1155/2022/9609970
- Sun B., Liu Z., Yin H., Wang T., Chen T., Yang S., Jiang Z. Intralesional versus intracoronary administration of glycoprotein IIb/IIIa inhibitors during percutaneous coronary intervention in patients with acute coronary syndromes: A meta-analysis of randomized controlled trials. Medicine (Baltimore). 2017;96(40):e8223. PMID: 28984776. PMCID: PMC5738012. https://dx.doi.org/10.1097/md.0000000000008223
- Minai K., Kawai M., Ogawa K., Nagoshi T., Morimoto S., Inoue Y., Tanaka T.D., Komukai K., Ogawa T., Yoshimura M. A pilot evaluation study of diffuse coronary arterial contraction causing ischemia by double measurement of left ventriculography before and after intracoronary administration of nitrates. Circ Rep. 2021;3(4):241-248. PMID: 33842730. PMCID: PMC8024012. https://doi.org/10.1253/circrep.cr-21-0015
- Kaul S., Methner C., Cao Z., Mishra A. Mechanisms of the "no-reflow" phenomenon after acute myocardial infarction: potential role of pericytes. JACC Basic Transl Sci. 2022;8(2):204-220. https://doi.org/10.1016/j.jacbts.2022.06.008
- Диль С.В., Вышлов Е.В., Рябов В.В. Интракоронарное введение эпинефрина и верапамила при рефрактерном феномене no-reflow у пациентов с острым инфарктом миокарда. Кардиоваскулярная терапия и профилактика. 2022;21(1):2936. https://doi.org/10.15829/1728-8800-2022-2936 Dil S.V., Vyshlov E.V., Ryabov V.V. Intracoronary epinephrine and verapamil in the refractory no-reflow phenomenon in patients with acute myocardial infarction. Cardiovascular Therapy and Prevention. 2022;21(1):2936. (In Russ.) https://doi.org/10.15829/1728-8800-2022-2936
- Dingli P.F., Escaned J. Minimalist immediate mechanical intervention in acute ST-segment elevation myocardial infarction: is it time to redefine targets? Cardiovasc Diagn Ther. 2017;7(1):4-10. PMID: 28164007. PMCID: PMC5253454. https://doi.org/10.21037/cdt.2016.11.03
- Сазанов Г.В., Шугушев З.Х. Эндоваскулярная профилактика развития дистальной эмболии в патогенезе развития феномена no-reflow при выполнении чрескожного коронарного вмешательства больным с острым коронарным синдромом с подъемом сегмента ST. Кардиологический вестник. 2024;19(1):23-28. https://doi.org/10.17116/Cardiobulletin20241901123 Sazanov G.V., Shugushev Z.Kh. Endovascular prevention of distal embolism in pathogenesis of no-reflow phenomenon in percutaneous coronary interventions in patients with ST-segment elevation acute coronary syndrome. Russian Cardiology Bulletin. 2024;19(1):23‑28. (In Russ.) https://doi.org/10.17116/Cardiobulletin20241901123
- Hori M., Inoue M., Kitakaze M., Koretsune Y., Iwai K., Tamai J., Ito H., Kitabatake A., Sato T., Kamada T. Role of adenosine in hyperemic response of coronary blood flow in microembolization. Am J Physiol. 1986;250(3Pt2):H509-518. PMID: 3953841. https://doi.org/10.1152/ajpheart.1986.250.3.h509
- Neumann F.J., Gick M. Direct stenting in ST-elevation myocardials infarction: convenient, but not improving outcomes. Eur Heart J. 2018;39(26):2480-2483. PMID: 29931300. https://doi.org/10.1093/eurheartj/ehy353
- Nepper-Christensen L., Kelaek H., Ahtarovski K.A., Hofsten D.E., Holmvang L., Pedersen F., Tilsted H.H., Aaroe J., Jensen S.E., Raungaard B., Terkelsen C.J., Kober L., Engstrøm T., Lonborg J. Angiographic outcome in patients treated with deferred stenting after ST-segment elevation myocardial infarction-results from DANAMI-3-DEFER. Eur Heart J Acute Cardiovasc Care. 2022;11(10):742-748. PMID: 36006808. https://doi.org/10.1093/ehjacc/zuac098
- Азаров А.В., Журавлев А.С., Семитко С.П. Эффективность отсроченного стентирования коронарных артерий в профилактике феномена no-reflow у пациентов с острым инфарктом миокарда с подъемом сегмента ST. Кардиоваскулярная терапия и профилактика. 2021;20(2):2629. https://doi.org/10.15829/1728-8800-2021-2629 Azarov A.V., Zhuravlev A.S., Semitko S.P. Effectiveness of deferred coronary artery stenting in the prevention of no-reflow in patients with acute ST-segment elevation myocardial infarction. Cardiovascular Therapy and Prevention. 2021;20(2):2629. (In Russ.) https://doi.org/10.15829/1728-8800-2021-2629

