Aortic valve replacement with the MedInzh-ST full-flow mechanical implant and modern bicuspid model: comparison of short-term results
Published 2024-08-30
Keywords
- Aortic Valve,
- Aortic Valve Disease,
- Heart Valve Prosthesis,
- Retrospective Studies
How to Cite
Copyright (c) 2024 Lepilin M.A., Tsekhanovich V.N., Sharifulin R.M., Bogachev-Prokophiev A.V.

This work is licensed under a Creative Commons Attribution 4.0 International License.
Abstract
Introduction: Mechanical heart valves prostheses have certain disadvantages related to impeding blood flow due to their shape and the design principle of the locking elements. The design of the new model of mechanical prostheses is based on the principle of full flow, which enables to increase the effective area of the valve opening and retain the identical dimensions of the implant. The results of using this type of prosthesis have not been sufficiently studied.
Objective: The study aimed to compare the short-term results of aortic valve replacement with the mechanical full-flow prosthesis and with the standard mechanical prosthesis.
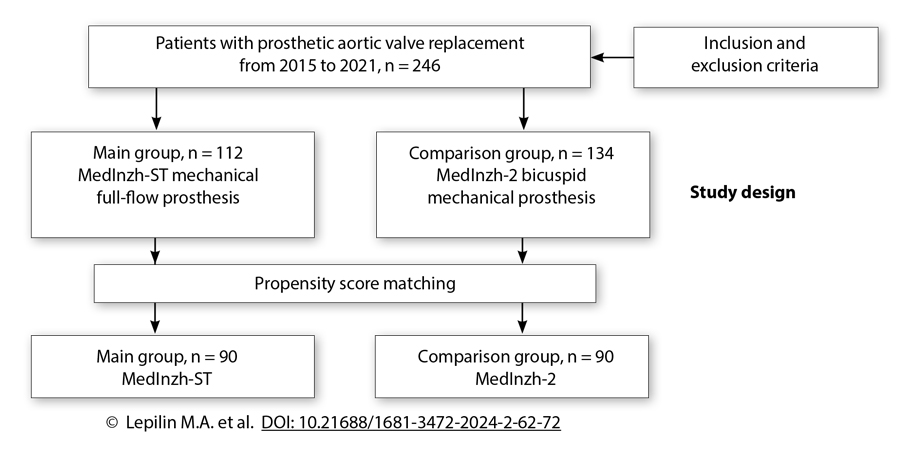
Methods: The retrospective study included 246 patients who underwent aortic valve replacement with mechanical prosthesis over the period from 2015 to 2021. The MedInzh-2 classical bicuspid valve was implanted in 134 patients, and the new full-flow prosthesis was used in 112 patients. A pseudorandomization procedure (Propensity score matching) was performed to equalize the groups. The level of the transprosthetic gradient was used as the primary endpoint.
Results: Propensity score matching resulted into forming two groups of 90 patients each. Hospital mortality in the MedInzh-ST group and the MedInzh-2 group amounted to 2.2% and 6.7%, respectively (Р = 0.178). In the early postoperative period, no differences in the processes of left ventricular cavity remodeling were found between the groups. In the MedInzh-ST full-flow prosthesis group, significantly lower values of transprosthetic gradients were revealed (mean gradients 12.6 versus 16.1 mm Hg, P < 0.001). The effective prosthetic orifice area was statistically higher in the full-flow implant group (2.04 versus 1.89 cm2, P < 0.001).
Conclusion: Application of the MedInzh-ST mechanical valve proved to be safe at surgical correction of aortic valve diseases. The prosthesis was hemodynamically effective that was confirmed by a significantly lower level of transprosthetic gradient and a larger effective valve orifice area in comparison to the standard bicuspid mechanical prosthesis.
Received 4 April 2024. Revised 18 August 2024. Accepted 20 August 2024.
Funding
The study was supported by the Grant of the Russian Science Foundation No. 23-15-00434.
Conflict of interest
The authors declare no conflict of interest.
Contribution of the authors
The authors contributed equally to this article.
References
- Nishimura R.A., Otto C.M., Bonow R.O., Carabello B.A., Erwin J.P. 3rd, Guyton R.A., O'Gara P.T., Ruiz C.E., Skubas N.J., Sorajja P., Sundt T.M. 3rd, Thomas J.D., Anderson J.L., Halperin J.L., Albert N.M., Bozkurt B., Brindis R.G., Creager M.A., Curtis L.H., DeMets D., Guyton R.A., Hochman J.S., Kovacs R.J., Ohman E.M., Pressler S.J., Sellke F.W., Shen W.-K., Stevenson W.G., Yancy C.W.; American College of Cardiology/American Heart Association. 2014 AHA/ACC guideline for the management of patients with valvular heart disease: a report of the American College of Cardiology/American Heart Association Task Force on Practice Guidelines. J Thorac Cardiovasc Surg. 2014;148(1):e1-e132. PMID: 24939033. https://doi.org/10.1016/j.jtcvs.2014.05.014
- Nkomo V.T., Gardin J.M., Skelton T.N., Gottdiener J.S., Scott C.G., Enriquez-Sarano M. Burden of valvular heart diseases: a population-based study. Lancet. 2006;368(9540):1005-1011. PMID: 16980116. https://doi.org/10.1016/S0140-6736(06)69208-8
- Pawade T.A., Newby D.E., Dweck M.R. Calcification in aortic stenosis: The skeleton key. J Am Coll Cardiol. 2015;66(5):561-577. PMID: 26227196. https://doi.org/10.1016/j.jacc.2015.05.066
- Rajamannan N.M., Evans F.J., Aikawa E., Grande-Allen K.J., Demer L.L., Heistad D.D., Simmons C.A., Masters K.S., Mathieu P., O'Brien K.D., Schoen F.J., Towler D.A., Yoganathan A.P., Otto C.M. Calcific aortic valve disease: not simply a degenerative process: A review and agenda for research from the National Heart and Lung and Blood Institute Aortic Stenosis Working Group. Executive summary: Calcific aortic valve disease-2011 update. Circulation. 2011;124(16):1783-1791. PMID: 22007101; PMCID: PMC3306614. https://doi.org/10.1161/CIRCULATIONAHA.110.006767
- Астапов Д.А., Демидов Д.П., Семенова Е.И. Протезирование аортального клапана бескаркасным биологическим протезом. Хирургия. Журнал им. Н.И. Пирогова. 2016;(5):4-12. https://doi.org/10.17116/hirurgia201654-12 Astapov D.A., Demidov D.P., Semenova E.I. Aortic valve replacement with stentless bioprosthesis. Khirurgiya. Zhurnal im. N.I. Pirogova = Pirogov Russian Journal of Surgery. 2016;(5):4-12. (In Russ.) https://doi.org/10.17116/hirurgia201654-12
- Toole J.M., Stroud M.R., Kratz J.M., Crumbley A.J. 3rd, Bradley S.M., Crawford F.A. Jr, Ikonomidis J.S. Twenty-five year experience with the St. Jude medical mechanical valve prosthesis. Ann Thorac Surg. 2010;89(5):1402-1409. PMID: 20417752. https://doi.org/10.1016/j.athoracsur.2010.01.045
- Lund O., Nielsen S.L., Arildsen H., Ilkjaer L.B., Pilegaard H.K. Standard aortic St. Jude valve at 18 years: performance profile and determinants of outcome. Ann Thorac Surg. 2000;69(5):1459-1465. PMID: 10881823. https://doi.org/10.1016/s0003-4975(00)01191-7
- Khan S.S., Trento A., DeRobertis M., Kass R.M., Sandhu M., Czer L.S., Blanche C., Raissi S., Fontana G.P., Cheng W., Chaux A., Matloff J.M. Twenty-year comparison of tissue and mechanical valve replacement. J Thorac Cardiovasc Surg. 2001;122(2):257-269. PMID: 11479498. https://doi.org/10.1067/mtc.2001.115238
- Bryan A.J., Rogers C.A., Bayliss K., Wild J., Angelini G.D. Prospective randomized comparison of CarboMedics and St. Jude Medical bileaflet mechanical heart valve prostheses: ten-year follow-up. J Thorac Cardiovasc Surg. 2007;133(3):614-622. PMID: 17320553. https://doi.org/10.1016/j.jtcvs.2006.08.075
- Murday A.J., Hochstitzky A., Mansfield J., Miles J., Taylor B., Whitley E., Treasure T. A prospective controlled trial of St. Jude versus Starr Edwards aortic and mitral valve prostheses. Ann Thorac Surg. 2003;76(1):66-73; discussion 73-74. PMID: 12842515. https://doi.org/10.1016/s0003-4975(03)00118-8
- Бокерия Л.А., Гудкова Р.Г. Сердечно-сосудистая хирургия – 2015. Болезни и врожденные аномалии системы кровообращения. М.: НЦССХ им А.Н. Бакулева, 2016. 208 с. Bokeriya L.A., Gudkova R.G. Cardiovascular surgery – 2015. Diseases and congenital anomalies of the circulatory system. Moscow: Bakulev National Medical Research Center for Cardiovascular Surgery Publ.; 2016. 208 p. (In Russ.)
- Рогулина Н.В., Горбунова Е.В., Кондюкова Н.В., Одаренко Ю.Н., Барбараш Л.С. Сравнительная оценка качества жизни реципиентов механических и биологических протезов при митральном пороке. Российский кардиологический журнал. 2015;(7):94-97. https://doi.org/10.15829/1560-4071-2015-7-94-97 Rogulina N.V., Gorbunova E.V., Kondyukova N.V., Odarenko Yu.N., Barbarash L.S. Comparison of the life quality with mechanical and biological mitral prostheses. Russian Journal of Cardiology. 2015;(7):94-97. (In Russ.) https://doi.org/10.15829/1560-4071-2015-7-94-97
- Celiento M., Filaferro L., Milano A.D., Anastasio G., Ferrari G., Bortolotti U. Single center experience with the Sorin Bicarbon prosthesis: a 17-year clinical follow-up. J Thorac Cardiovasc Surg. 2014;148(5):2039-2044. PMID: 24332112. https://doi.org/10.1016/j.jtcvs.2013.11.015
- Tominaga R., Kurisu K., Ochiai Y., Tomita Y., Masuda M., Morita S., Yasui H. A 10-year experience with the Carbomedics cardiac prosthesis. Ann Thorac Surg. 2005;79(3):784-789. PMID: 15734377. https://doi.org/10.1016/j.athoracsur.2004.08.067
- Молчанов А.Н., Идов Э.М., Хрущев И.В., Гамзаев А.Б., Ананьев Д.А., Цеханович В.Н., Богачев-Прокофьев А.В., Чернов И.И., Дробот Д.Б., Глумсков А.Б., Евдокимов С.В. Результаты протезирования аортального клапана полнопроточным механическим протезом «МедИнж-СТ». Медицинский альманах. 2018;(1):105-108. Molchanov А.N., Idov E.М., Khruschev I.V., Gamzaev А.B., Ananiev D.А., Tsekhanovich V.N., Bogachev-Prokofiev А.V., Chernov I.I., Drobot D.B., Glumskov А.B., Evdokimov S.V. Results of aortic valve replacement with “MedInzh-ST” full-flow prosthetic cardiac valve. Medicinskij almanah = Medical Almanac. 2018;(1):105-108. (In Russ.)
- Biancari F., Martin M., Bordin G., Vettore E., Vinco G., Anttila V., Airaksinen J., Vasques F. Basic data from 176 studies on the immediate outcome after aortic valve replacement with or without coronary artery bypass surgery. J Cardiothorac Vasc Anesth. 2014;28(5):1251-1256. PMID: 24290746. https://doi.org/10.1053/j.jvca.2013.07.020
- Magovern J.A., Pennock J.L., Campbell D.B., Pae W.E., Bartholomew M., Pierce W.S., Waldhausen J.A. Aortic valve replacement and combined aortic valve replacement and coronary artery bypass grafting: predicting high risk groups. J Am Coll Cardiol. 1987;9(1):38-43. PMID: 3491844. https://doi.org/10.1016/S0735-1097(87)80079-7
- Энгиноев С.Т., Зеньков А.А., Чернов И.И., Джамбиева М.Н., Рамазанова Н.Э., Баев Д.Ю., Хассан М.М., Болурова А.М., Колесников В.Н. Непосредственные и среднесрочные результаты имплантации механического протеза «МедИнж-2» в аортальной позиции: десятилетний опыт одного центра. Креативная хирургия и онкология. 2024;14(1):20-28. https://doi.org/10.24060/2076-3093-2024-14-1-20-28 Enginoev S.T., Ziankou A.A., Chernov I.I., Dzhambieva M.N., Ramazanova N.E., Baev D.Yu., Hassan M.M., Bolurova A.M., Kolesnikov V.N. Immediate and mid-term results of implanting a MedInzh-2 mechanical prosthesis in the aortic position: ten-year experience of one center. Creative Surgery and Oncology. 2024;14(1):20-28. (In Russ.) https://doi.org/10.24060/2076-3093-2024-14-1-20-28
- Chambers J., Roxburgh J., Blauth C., O'Riordan J., Hodson F., Rimington H. A randomized comparison of the MCRI On-X and CarboMedics Top Hat bileaflet mechanical replacement aortic valves: early postoperative hemodynamic function and clinical events. J Thorac Cardiovasc Surg. 2005;130(3):759-764. PMID: 16153925. https://doi.org/10.1016/j.jtcvs.2005.02.057
- Jawitz O.K., Wang T.Y., Lopes R.D., Chavez A., Boyer B., Kim H., Anstrom K.J., Becker R.C., Blackstone E., Ruel M., Thourani V.H., Puskas J.D., Gerdisch M.W., Johnston D., Capps S., Alexander J.H., Svensson L.G. Rationale and design of PROACT Xa: A randomized, multicenter, open-label, clinical trial to evaluate the efficacy and safety of apixaban versus warfarin in patients with a mechanical On-X Aortic Heart Valve. Am Heart J. 2020;227:91-99. PMID: 32693197; PMCID: PMC7484170. https://doi.org/10.1016/j.ahj.2020.06.014
- Базылев В.В., Глумсков А.Б., Евтюшкин И.А., Идов Э.М., Молчанов А.Н., Богачев-Прокофьев А.В., Салегин А.В., Чигинев В.А., Гамзаев А.Б., Ананьев Д.А., Козлов А.В., Сакович В.А., Дробот Д.Б., Тарасов Д.Г., Чернов И.И., Цеханович В.Н. Среднесрочные результаты клинического исследования аортальных полнопроточных механических протезов клапанов сердца «МедИнж-СТ». Бюллетень НЦССХ им. А.Н. Бакулева РАМН. Сердечно-сосудистые заболевания. 2016;17(S6):27. Bazylev V.V., Glumskov A.B., Yevtyushkin I.A., Idov E.M., Molchanov A.N., Bogachev-Prokophiev A.V., Salegin A.V., Chiginev V.A., Gamzayev A.B., Ananyev D.A., Kozlov A.V., Sakovich V.A., Drobot D.B., Tarasov D.G., Chernov I.I., Tsekhanovich V.N. Mid-term results of clinical studies of aortic full-flow mechanical heart valve prostheses “MedInzh-ST”. The Bulletin of Bakoulev Center. Cardiovascular Diseases. 2016;17(S6):27. (In Russ.)
- Абдульянов И.В., Вагизов И.И., Каипов А.Э. Клинические результаты протезирования клапанов сердца двустворчатым полнопроточным механическим протезом «МедИнж-СТ». Ангиология и сосудистая хирургия. Журнал им. академика А.В. Покровского. 2020;26(4):141-148. https://doi.org/10.33529/ANGIO2020419 Abdulyanov I.V., Vagizov I.I., Kaipov A.E. Clinical results of cardiac valve repair with bicuspid full-flow mechanical prosthesis “MedEng-ST”. Angiology and Vascular Surgery. 2020;26(4):141-148. (In Russ.) https://doi.org/10.33529/ANGIO2020419

