Ischemic mitral regurgitation: mitral valve replacement, restrictive annuloplasty or multi-component reconstruction with subvalvular intervention (systematic review and meta-analysis)
Published 2024-11-08
Keywords
- Coronary Artery Bypass,
- Ischemia,
- Mitral Valve,
- Mitral Valve Insufficiency,
- PubMed
- Search Engine ...More
How to Cite
Copyright (c) 2024 Skopin I.I., Latyshev M.S., Kakhktsyan P.V., Ukurova Z.R., Murysova D.V., Babukhina Yu.I., Dremin A.V., Asatryan T.V.

This work is licensed under a Creative Commons Attribution 4.0 International License.
Abstract
Objective: The study is aimed at assessing short- and long-term results of various strategies of surgical treatment in patients with ischemic mitral insufficiency.
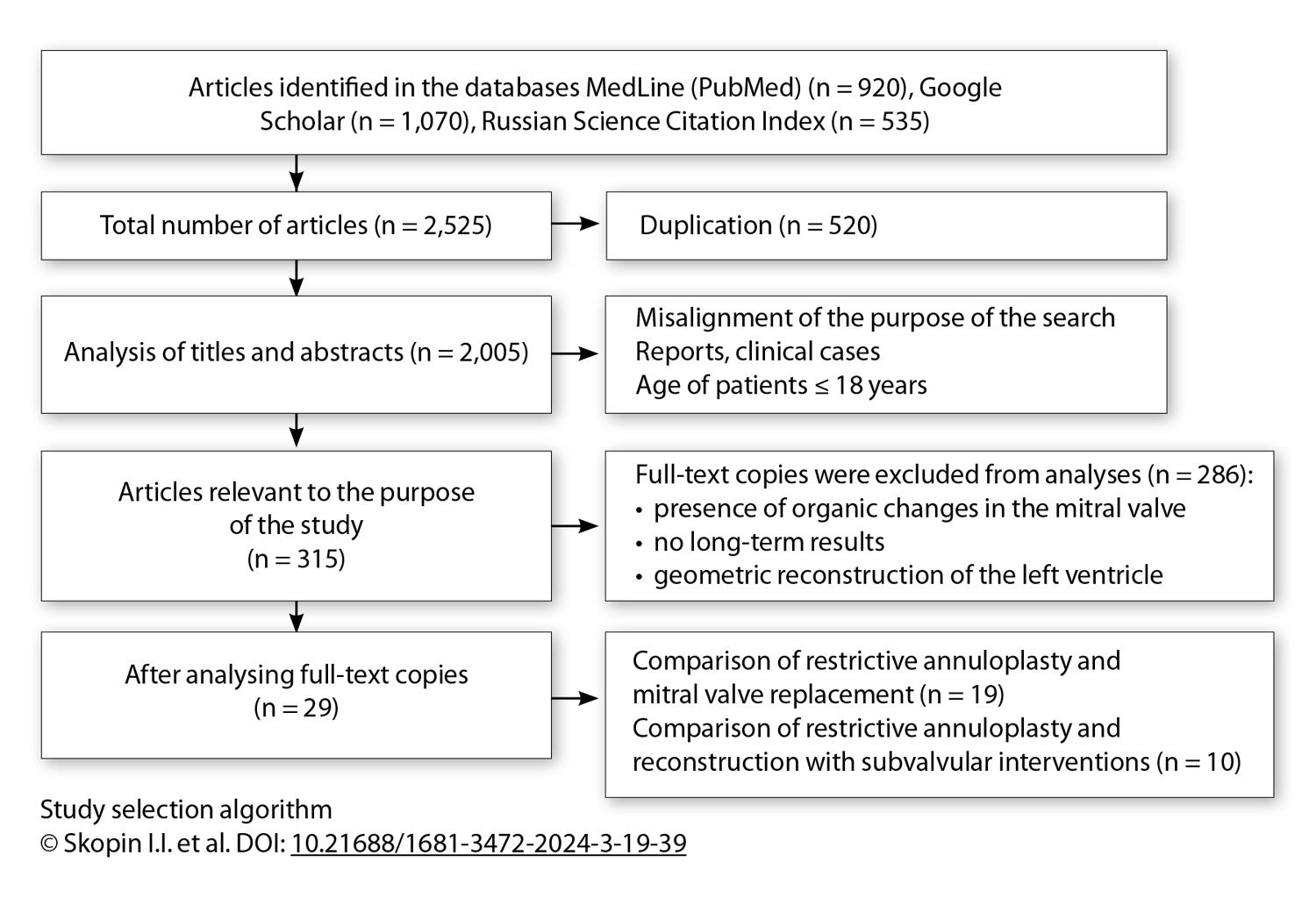
Methods: The study design was accomplished according to the PRISMA criteria in the PubMed, Google Scholar and eLibrary databases. Surgical treatment included 3 strategies: mitral valve replacement (MVR) with preservation of subvalvular structures, restrictive annuloplasty (RA) and reconstruction with intervention on subvalvular structures (RISS). The primary endpoint included all-cause death during 30 days or follow-up period, as well as rehospitalization caused by heart failure progression. The secondary endpoint was related to recurrence of mitral regurgitation > 2 degree, effective reverse left ventricular remodeling and reoperation. The discussion presents own authors’ experience based on treatment of 100 patients with type IIIb ischemic mitral regurgitation and low reconstructive potential (median follow-up 62 months).
Results: The analysis involved 29 papers (n = 4,857) representing by 2 randomized controlled trials (7 %, n = 347) and 27 retrospective investigations (93 %, n = 4,424). All patients underwent coronary artery bypass grafting or stenting of the coronary arteries. All included studies were divided into 2 groups according to the compared type of surgery strategies: 1) isolated restrictive annuloplasty (RA) versus mitral valve replacement (MVR) with preservation of subvalvular structures (19 papers, n = 4,020); 2) isolated restrictive annuloplasty (RA) versus reconstruction with intervention on subvalvular structures (RISS) (10 papers, n = 751).
Comparison of MVR and RA: 30-day mortality was 11.78% (164/1,392) in the MVR group vs 6.28% (150/2,389) in the RA group, p < 0.0001 (further indicators are referred to MVR and RA comparison, respectively); long-term mortality reached 28.62% (281/982) vs 25.35% (413/1,629), p = 0.067; mitral regurgitation > 2 degree manifested at the level of 3.82% (27/707) (paraprosthetic regurgitation) vs 18.91% (173/915), p < 0.0001; reoperation was performed in 6.56% (49/747) of patients vs 9.21% (63/684), p = 0.0622.
Comparison of RISS and RA: 30-day mortality was 4.86% (15/307) in the RISS group vs 7.93% (28/353) in the RA group, p = 0.11 (further indicators are referred to RISS and RA comparison, respectively); long-term mortality was 12.62% (13/103) vs 15.53% (16/103), p = 0.55; mitral regurgitation > 2 degree was detected in 7.30% (17/233) of cases vs 24.19% (67/277), p < 0.01; rehospitalization was performed in 17.48% (18/103) of cases vs 28.16% (29/103), p = 0.07; reoperation was accomplished in 2.94% (4/136) of cases vs 7.41% (12/162), p = 0.09; effective reverse left ventricular remodeling was characterized by left ventricular end-diastolic dimension of –8.9%, p < 0.01 vs –2.2%, p = 0.04.
Conclusion: The choice of a surgical treatment strategy in patients with ischemic mitral regurgitation should be determined by the type of mitral dysfunction. In type I, restrictive annuloplasty may be an effective technique, while in type IIIb, reconstruction with intervention on subvalvular structures or mitral valve replacement with preservation of subvalvular structures is necessary.
Received 30 March 2024. Revised 5 July 2024. Accepted 1 October 2024.
Funding
The study did not have sponsorship.
Conflict of interest
The authors declare no conflict of interest.
Contribution of the authors
Conception and study design: I.I. Skopin, M.S. Latyshev, P.V. Kakhktsyan
Data collection and analysis: M.S. Latyshev, Z.R. Ukurova, Yu.I. Babukhina
Statistical analysis: M.S. Latyshev, T.V. Asatryan, D.V. Murysova
Drafting the article: I.I. Skopin, M.S. Latyshev, D.V. Murysova, P.V. Kakhktsyan
Critical revision of the article: I.I. Skopin, M.S. Latyshev
Final approval of the version to be published: I.I. Skopin, M.S. Latyshev, P.V. Kakhktsyan, Z.R. Ukurova, D.V. Murysova, Yu.I. Babukhina, A.V. Dremin, T.V. Asatryan
References
- de Marchena E., Badiye A., Robalino G., Junttila J., Atapattu S., Nakamura M., De Canniere D., Salerno T. Respective prevalence of the different Carpentier classes of mitral regurgitation: a stepping stone for future therapeutic research and development. J Card Surg. 2011;26(4):385-392. PMID: 21793928. https://doi.org/10.1111/j.1540-8191.2011.01274.x
- Nkomo V.T., Gardin J.M., Skelton T.N., Gottdiener J.S., Scott C.G., Enriquez-Sarano M. Burden of valvular heart diseases: a population-based study. Lancet. 2006;368(9540):1005-1011. PMID: 16980116. https://doi.org/10.1016/S0140-6736(06)69208-8
- Moher D., Liberati A., Tetzlaff J., Altman D.G.; PRISMA Group. Preferred reporting items for systematic reviews and meta-analyses: the PRISMA statement. PLoS Med. 2009;6(7):e1000097. PMID: 19621072; PMCID: PMC2707599. https://doi.org/10.1371/journal.pmed.1000097
- Zoghbi W.A., Adams D., Bonow R.O., Enriquez-Sarano M., Foster E., Grayburn P.A., Hahn R.T., Han Y., Hung J., Lang R.M., Little S.H., Shah D.J., Shernan S., Thavendiranathan P., Thomas J.D., Weissman N.J. Recommendations for noninvasive evaluation of native valvular regurgitation: A report from the American Society of Echocardiography developed in collaboration with the Society for Cardiovascular Magnetic Resonance. J Am Soc Echocardiogr. 2017;30(4):303-371. PMID: 28314623. https://doi.org/10.1016/j.echo.2017.01.007
- Vahanian A., Beyersdorf F., Praz F., Milojevic M., Baldus S., Bauersachs J., Capodanno D., Conradi L., De Bonis M., De Paulis R., Delgado V., Freemantle N., Gilard M., Haugaa K.H., Jeppsson A., Jüni P., Pierard L., Prendergast B.D., Sádaba J.R., Tribouilloy C., Wojakowski W.; ESC/EACTS Scientific Document Group. 2021 ESC/EACTS Guidelines for the management of valvular heart disease. Eur Heart J. 2022;43(7):561-632. Erratum in: Eur Heart J. 2022;43(21):2022. PMID: 34453165. https://doi.org/10.1093/eurheartj/ehab395
- Hickey M.S., Smith L.R., Muhlbaier L.H., Harrell F.E. Jr, Reves J.G., Hinohara T., Califf R.M., Pryor D.B., Rankin J.S. Current prognosis of ischemic mitral regurgitation. Implications for future management. Circulation. 1988;78(3 Pt 2):I51-I59. PMID: 2970346.
- Cohn L.H., Rizzo R.J., Adams D.H., Couper G.S., Sullivan T.E., Collins J.J. Jr, Aranki S.F. The effect of pathophysiology on the surgical treatment of ischemic mitral regurgitation: operative and late risks of repair versus replacement. Eur J Cardiothorac Surg. 1995;9(10):568-574. PMID: 8562102. https://doi.org/10.1016/s1010-7940(05)80008-9
- Gillinov A.M., Wierup P.N., Blackstone E.H., Bishay E.S., Cosgrove D.M., White J., Lytle B.W., McCarthy P.M. Is repair preferable to replacement for ischemic mitral regurgitation? J Thorac Cardiovasc Surg. 2001;122(6):1125-1141. PMID: 11726887. https://doi.org/10.1067/mtc.2001.116557
- Reece T.B., Tribble C.G., Ellman P.I., Maxey T.S., Woodford R.L., Dimeling G.M., Wellons H.A., Crosby I.K., Kern J.A., Kron I.L. Mitral repair is superior to replacement when associated with coronary artery disease. Ann Surg. 2004;239(5):671-675; discussion 675-677. PMID: 15082971; PMCID: PMC1356275. https://doi.org/10.1097/01.sla.0000124297.40815.86
- Mantovani V., Mariscalco G., Leva C., Blanzola C., Cattaneo P., Sala A. Long-term results of the surgical treatment of chronic ischemic mitral regurgitation: comparison of repair and prosthetic replacement. J Heart Valve Dis. 2004;13(3):421-428; discussion 428-429. PMID: 15222289.
- Al-Radi O.O., Austin P.C., Tu J.V., David T.E., Yau T.M. Mitral repair versus replacement for ischemic mitral regurgitation. Ann Thorac Surg. 2005;79(4):1260-1267; discussion 1260-1267. PMID: 15797060. https://doi.org/10.1016/j.athoracsur.2004.09.044
- Silberman S., Oren A., Klutstein M.W., Deeb M., Asher E., Merin O., Fink D., Bitran D. Does mitral valve intervention have an impact on late survival in ischemic cardiomyopathy? Isr Med Assoc J. 2006;8(1):17-20. PMID: 16450745.
- Milano C.A., Daneshmand M.A., Rankin J.S., Honeycutt E., Williams M.L., Swaminathan M., Linblad L., Shaw L.K., Glower D.D., Smith P.K. Survival prognosis and surgical management of ischemic mitral regurgitation. Ann Thorac Surg. 2008;86(3):735-744. PMID: 18721554. https://doi.org/10.1016/j.athoracsur.2008.05.017
- Micovic S., Milacic P., Otasevic P., Tasic N., Boskovic S., Nezic D., Djukanovic B. Comparison of valve annuloplasty and replacement for ischemic mitral valve incompetence. Heart Surg Forum. 2008;11(6):E340-E345. PMID: 19073530. https://doi.org/10.1532/HSF98.20081087
- Ngaage D.L., Daly R.C., Rosales G., Sundt T.M. 3rd, Dearani J.A., Mullany C.J., McGregor C.G., Orszulak T.A., Puga F.J., Schaff H.V. Mitral regurgitation surgery in heart failure due to ischemic cardiomyopathy: a 24-year experience. J Heart Valve Dis. 2008;17(3):251-259; discussion 259-260. PMID: 18592921.
- Magne J., Girerd N., Sénéchal M., Mathieu P., Dagenais F., Dumesnil J.G., Charbonneau E., Voisine P., Pibarot P. Mitral repair versus replacement for ischemic mitral regurgitation: comparison of short-term and long-term survival. Circulation. 2009;120(11 Suppl):S104-S111. PMID: 19752354. https://doi.org/10.1161/CIRCULATIONAHA.108.843995
- Chan V., Ruel M., Mesana T.G. Mitral valve replacement is a viable alternative to mitral valve repair for ischemic mitral regurgitation: a case-matched study. Ann Thorac Surg. 2011;92(4):1358-1365; discussion 1365-1366. PMID: 21958783. https://doi.org/10.1016/j.athoracsur.2011.05.056
- Maltais S., Schaff H.V., Daly R.C., Suri R.M., Dearani J.A., Sundt T.M. 3rd, Enriquez-Sarano M., Topilsky Y., Park S.J. Mitral regurgitation surgery in patients with ischemic cardiomyopathy and ischemic mitral regurgitation: factors that influence survival. J Thorac Cardiovasc Surg. 2011;142(5):995-1001. PMID: 21855899. https://doi.org/10.1016/j.jtcvs.2011.07.044
- Yoshida K., Okada K., Miyahara S., Omura A., Inoue T., Minami H., Okita Y. Mitral valve replacement versus annuloplasty for treating severe functional mitral regurgitation. Gen Thorac Cardiovasc Surg. 2014;62(1):38-47. PMID: 24005597. https://doi.org/10.1007/s11748-013-0297-2
- De Bonis M., Ferrara D., Taramasso M., Calabrese M.C., Verzini A., Buzzatti N., Alfieri O. Mitral replacement or repair for functional mitral regurgitation in dilated and ischemic cardiomyopathy: is it really the same? Ann Thorac Surg. 2012;94(1):44-51. PMID: 22440363. https://doi.org/10.1016/j.athoracsur.2012.01.047
- Ljubacev A., Medved I., Ostrik M., Zuvić-Butorac M., Sokolić J. Mitral regurgitation and coronary artery bypass surgery: comparison of mitral valve repair and replacement. Acta Chir Belg. 2013;113(3):187-191. PMID: 24941714. https://doi.org/10.1080/00015458.2013.11680909
- Lorusso R., Gelsomino S., Vizzardi E., D'Aloia A., De Cicco G., Lucà F., Parise O., Gensini G.F., Stefàno P., Livi U., Vendramin I., Pacini D., Di Bartolomeo R., Miceli A., Varone E., Glauber M., Parolari A., Giuseppe Arlati F., Alamanni F., Serraino F., Renzulli A., Messina A., Troise G., Mariscalco G., Cottini M., Beghi C., Nicolini F., Gherli T., Borghetti V., Pardini A., Caimmi P.P., Micalizzi E., Fino C., Ferrazzi P., Di Mauro M., Calafiore A.M.; ISTIMIR Investigators. Mitral valve repair or replacement for ischemic mitral regurgitation? The Italian Study on the Treatment of Ischemic Mitral Regurgitation (ISTIMIR). J Thorac Cardiovasc Surg. 2013;145(1):128-139; discussion 137-138. PMID: 23127376. https://doi.org/10.1016/j.jtcvs.2012.09.042
- Lio A., Miceli A., Varone E., Canarutto D., Di Stefano G., Della Pina F., Gilmanov D., Murzi M., Solinas M., Glauber M. Mitral valve repair versus replacement in patients with ischaemic mitral regurgitation and depressed ejection fraction: risk factors for early and mid-term mortality. Interact Cardiovasc Thorac Surg. 2014;19(1):64-69. PMID: 24676552. https://doi.org/10.1093/icvts/ivu066
- Goldstein D., Moskowitz A.J., Gelijns A.C., Ailawadi G., Parides M.K., Perrault L.P., Hung J.W., Voisine P., Dagenais F., Gillinov A.M., Thourani V., Argenziano M., Gammie J.S., Mack M., Demers P., Atluri P., Rose E.A., O'Sullivan K., Williams D.L., Bagiella E., Michler R.E., Weisel R.D., Miller M.A., Geller N.L., Taddei-Peters W.C., Smith P.K., Moquete E., Overbey J.R., Kron I.L., O'Gara P.T., Acker M.A.; CTSN. Two-year outcomes of surgical treatment of severe ischemic mitral regurgitation. N Engl J Med. 2016;374(4):344-353. PMID: 26550689; PMCID: PMC4908819. https://doi.org/10.1056/NEJMoa1512913
- Borger M.A., Murphy P.M., Alam A., Fazel S., Maganti M., Armstrong S., Rao V., David T.E. Initial results of the chordal-cutting operation for ischemic mitral regurgitation. J Thorac Cardiovasc Surg. 2007;133(6):1483-1492. PMID: 17532944. https://doi.org/10.1016/j.jtcvs.2007.01.064
- Langer F., Kunihara T., Hell K., Schramm R., Schmidt K.I., Aicher D., Kindermann M., Schäfers H.J. RING+STRING: Successful repair technique for ischemic mitral regurgitation with severe leaflet tethering. Circulation. 2009;120(11 Suppl):S85-S91. PMID: 19752391. https://doi.org/10.1161/CIRCULATIONAHA.108.840173
- Fattouch K., Lancellotti P., Castrovinci S., Murana G., Sampognaro R., Corrado E., Caruso M., Speziale G., Novo S., Ruvolo G. Papillary muscle relocation in conjunction with valve annuloplasty improve repair results in severe ischemic mitral regurgitation. J Thorac Cardiovasc Surg. 2012;143(6):1352-1355. PMID: 22050990. https://doi.org/10.1016/j.jtcvs.2011.09.062
- Roshanali F., Vedadian A., Shoar S., Naderan M., Mandegar M.H. Efficacy of papillary muscle approximation in preventing functional mitral regurgitation recurrence in high-risk patients with ischaemic cardiomyopathy and mitral regurgitation. Acta Cardiol. 2013;68(3):271-278. PMID: 23882872. https://doi.org/10.1080/ac.68.3.2983421
- Calafiore A.M., Refaie R., Iacò A.L., Asif M., Al Shurafa H.S., Al-Amri H., Romeo A., Di Mauro M. Chordal cutting in ischemic mitral regurgitation: a propensity-matched study. J Thorac Cardiovasc Surg. 2014;148(1):41-46. Erratum in: J Thorac Cardiovasc Surg. 2014;148(4):1773. PMID: 24041764. https://doi.org/10.1016/j.jtcvs.2013.07.036
- Murashita T., Okada Y., Kanemitsu H., Fukunaga N., Konishi Y., Nakamura K., Koyama T. Midterm outcomes of chordal cutting in combination with downsized ring annuloplasty for ischemic mitral regurgitation. Ann Thorac Cardiovasc Surg. 2014;20(6):1008-1015. PMID: 24492174. https://doi.org/10.5761/atcs.oa.13-00293
- Watanabe T., Arai H., Nagaoka E., Oi K., Hachimaru T., Kuroki H., Fujiwara T., Mizuno T. Influence of procedural differences on mitral valve configuration after surgical repair for functional mitral regurgitation: in which direction should the papillary muscle be relocated? J Cardiothorac Surg. 2014;9:185. PMID: 25491075; PMCID: PMC4272782. https://doi.org/10.1186/s13019-014-0185-6
- Mihos C.G., Capoulade R., Yucel E., Melnitchouk S., Hung J. Combined papillary muscle sling and ring annuloplasty for moderate-to-severe secondary mitral regurgitation. J Card Surg. 2016;31(11):664-671. PMID: 27620350. https://doi.org/10.1111/jocs.12843
- Nappi F., Lusini M., Spadaccio C., Nenna A., Covino E., Acar C., Chello M. Papillary muscle approximation versus restrictive annuloplasty alone for severe ischemic mitral regurgitation. J Am Coll Cardiol. 2016;67(20):2334-2346. PMID: 27199056. https://doi.org/10.1016/j.jacc.2016.03.478
- Harmel E., Pausch J., Gross T., Petersen J., Sinning C., Kubitz J., Reichenspurner H., Girdauskas E. Standardized subannular repair improves outcomes in type IIIb functional mitral regurgitation. Ann Thorac Surg. 2019;108(6):1783-1792. PMID: 31254507. https://doi.org/10.1016/j.athoracsur.2019.04.120
- Otto C.M., Nishimura R.A., Bonow R.O., Carabello B.A., Erwin J.P. 3rd, Gentile F., Jneid H., Krieger E.V., Mack M., McLeod C., O'Gara P.T., Rigolin V.H., Sundt T.M. 3rd, Thompson A., Toly C. 2020 ACC/AHA Guideline for the management of patients with valvular heart disease: Executive summary: A report of the American College of Cardiology/American Heart Association Joint Committee on Clinical Practice Guidelines. Circulation. 2021;143(5):e35-e71. Erratum in: Circulation. 2021;143(5):e228. Erratum in: Circulation. 2021;143(10):e784. PMID: 33332149. https://doi.org/10.1161/CIR.0000000000000932
- Vassileva C.M., Boley T., Markwell S., Hazelrigg S. Meta-analysis of short-term and long-term survival following repair versus replacement for ischemic mitral regurgitation. Eur J Cardiothorac Surg. 2011;39(3):295-303. PMID: 20727782. https://doi.org/10.1016/j.ejcts.2010.06.034
- Salmasi M.Y., Acharya M., Humayun N., Baskaran D., Hubbard S., Vohra H. Is valve repair preferable to valve replacement in ischaemic mitral regurgitation? A systematic review and meta-analysis. Eur J Cardiothorac Surg. 2016;50(1):17-28. PMID: 27009102. https://doi.org/10.1093/ejcts/ezw053
- Белов Ю.В., Вараксин В.А. Постинфарктное ремоделирование левого желудочка сердца. От концепции к хирургическому лечению. М.: ДеНово, 2002. 194 с. Belov Yu.V., Varaksin V.A. Post-infarction remodeling of the left ventricle of the heart. From concept to surgical treatment. Moscow: DeNovo Publ.; 2002. 194 p. (In Russ.)
- Молочков А.В., Жбанов И.В., Ховрин В.В., Кулагина Т.Ю., Кузнецова Л.М., Ревуненков Г.В., Шабалкин Б.В. Диагностические критерии и хирургические принципы адекватной коррекции полости левого желудочка у больных ишемической кардиомиопатией. Кардиология и сердечно-сосудистая хирургия. 2009;2(2):23-27. Molochkov A.V., Zhbanov I.V., Khovrin V.V., Kulagina T.Iu., Kuznetsova L.M., Revunenkov G.V., Shabalkin B.V. Diagnostic criterions and surgical principles for adequate correction of left ventricular cavity in patients with ischemic cardiomyopathy. Russian Journal of Cardiology and Cardiovascular Surgery. 2009;2(2):23-27. (In Russ.)
- Magne J., Girerd N., Sénéchal M., Mathieu P., Dagenais F., Dumesnil J.G., Charbonneau E., Voisine P., Pibarot P. Mitral repair versus replacement for ischemic mitral regurgitation: comparison of short-term and long-term survival. Circulation. 2009;120(11 Suppl):S104-S111. PMID: 19752354. https://doi.org/10.1161/CIRCULATIONAHA.108.843995
- Thourani V.H., Weintraub W.S., Guyton R.A., Jones E.L., Williams W.H., Elkabbani S., Craver J.M. Outcomes and long-term survival for patients undergoing mitral valve repair versus replacement: effect of age and concomitant coronary artery bypass grafting. Circulation. 2003;108(3):298-304. PMID: 12835220. https://doi.org/10.1161/01.CIR.0000079169.15862.13
- Milano C.A., Daneshmand M.A., Rankin J.S., Honeycutt E., Williams M.L., Swaminathan M., Linblad L., Shaw L.K., Glower D.D., Smith P.K. Survival prognosis and surgical management of ischemic mitral regurgitation. Ann Thorac Surg. 2008;86(3):735-744. PMID: 18721554. https://doi.org/10.1016/j.athoracsur.2008.05.017
- Nappi F., Spadaccio C., Nenna A., Lusini M., Fraldi M., Acar C., Chello M. Is subvalvular repair worthwhile in severe ischemic mitral regurgitation? Subanalysis of the Papillary Muscle Approximation trial. J Thorac Cardiovasc Surg. 2017;153(2):286-295.e2. PMID: 27773578. https://doi.org/10.1016/j.jtcvs.2016.09.050
- Хубулава Г.Г., Марченко С.П., Алексанян М.Г., Сизенко В.В., Кривопалов В.А., Кусай А.С., Наумов А.Б., Ополченов Д.П., Сухарев А.Е., Волков А.М. Пластика митрального клапана в сочетании с коронарным шунтированием у пациентов с ишемической митральной недостаточностью. Вестник Российской Военно-медицинской академии. 2013;41(1):6-10. Khubulava G.G., Marchenko S.P., Aleksanyan M.G., Sizenko V.V., Krivopalov V.A., Kusay A.S., Naumov A.B., Opolchenov D.P., Sukharev A.E., Volkov A.M. Mitral valve repair with coronary artery bypass grafting in patients with ischemic mitral regurgitation. Bulletin of the Russian Military Medical Academy. 2013;41(1):6-10. (In Russ.)
- Kuwahara E., Otsuji Y., Iguro Y., Ueno T., Zhu F., Mizukami N., Kubota K., Nakashiki K., Yuasa T., Yu B., Uemura T., Takasaki K., Miyata M., Hamasaki S., Kisanuki A., Levine R.A., Sakata R., Tei C. Mechanism of recurrent/persistent ischemic/functional mitral regurgitation in the chronic phase after surgical annuloplasty: importance of augmented posterior leaflet tethering. Circulation. 2006;114(1 Suppl):I529-I534. PMID: 16820632. https://doi.org/10.1161/CIRCULATIONAHA.105.000729
- Yamamoto H., Iguro Y., Sakata R., Arata K., Yotsumoto G. Effectively treating ischemic mitral regurgitation with chordal cutting in combination with ring annuloplasty and left ventricular reshaping approach. J Thorac Cardiovasc Surg. 2005;130(2):589-590. PMID: 16077444. https://doi.org/10.1016/j.jtcvs.2005.04.006
- Sharma H., Liu B., Mahmoud-Elsayed H., Myerson S.G., Steeds R.P. Multimodality imaging in secondary mitral regurgitation. Front Cardiovasc Med. 2020;7:546279. PMID: 33415127; PMCID: PMC7782243. https://doi.org/10.3389/fcvm.2020.546279
- Lancellotti P., Tribouilloy C., Hagendorff A., Popescu B.A., Edvardsen T., Pierard L.A., Badano L., Zamorano J.L.; Scientific Document Committee of the European Association of Cardiovascular Imaging. Recommendations for the echocardiographic assessment of native valvular regurgitation: an executive summary from the European Association of Cardiovascular Imaging. Eur Heart J Cardiovasc Imaging. 2013;14(7):611-644. PMID: 23733442. https://doi.org/10.1093/ehjci/jet105
- Petrus A.H.J., Dekkers O.M., Tops L.F., Timmer E., Klautz R.J.M., Braun J. Impact of recurrent mitral regurgitation after mitral valve repair for functional mitral regurgitation: long-term analysis of competing outcomes. Eur Heart J. 2019;40(27):2206-2214. PMID: 31114862. https://doi.org/10.1093/eurheartj/ehz306
- Шумовец В.В., Гринчук И.И., Андралойть И.Е., Шкет А.П., Курганович С.А., Лысенок Е.Р., Семенова Н.В., Островский Ю.П. Пластика или протезирование митрального клапана у пациентов с выраженной ишемической митральной недостаточностью? Пилотное исследование. Кардиология в Беларуси. 2016;8(1):61-72. Shumavet V., Grinchuk I., Andraloits I., Shket A., Kurganovich S., Lysjonok E., Semenova N., Ostrovski Yu. Mitral valve repair or replacement in patients with severe ischemic mitral regurgitation? A pilot study. Cardiology in Belarus. 2016;8(1):61-72. (In Russ.)
- Гордеев М.Л., Майстренко А.Д., Сухова И.В., Майстренко Н.С., Исаков С.В., Гурщенков А.В., Гребенник В.К. Отдаленные результаты использования безимплантационной аннулопластики митрального клапана у пациентов с митральной недостаточностью ишемического генеза. Патология кровообращения и кардиохирургия. 2015;19(1):36-42. Gordeev M.L., Maistrenko A.D., Sukhova I.V., Maistrenko N.S., Isakov S.V., Gurshchenkov A.V., Grebennik V.K. Suture annuloplasty for surgical treatment of ischemic mitral regurgitation: long-term results. Patologiya krovoobrashcheniya i kardiokhirurgiya = Circulation Pathology and Cardiac Surgery. 2015;19(1):36-42. (In Russ.)
- Антипов Г.Н., Постол А.С., Котов С.Н., Макарова М.О., Шнейдер Ю.А. Анализ результатов коррекции ишемической митральной недостаточности с применением шва О. Алфиери и без него. Грудная и сердечно-сосудистая хирургия. 2021;63(5):412-417. https://doi.org/10.24022/0236-2791-2021-63-5-412-417 Antipov G.N., Postol A.S., Kotov S.N., Makarova M.O., Schneider Yu.A. Analysis of the results of correction of ischemic mitral insufficiency with and without the O. Alfieri stitch. Russian Journal of Thoracic and Cardiovascular Surgery. 2021;63(5):412-417. (In Russ.) https://doi.org/10.24022/0236-2791-2021-63-5-412-417
- Базылев В.В., Тунгусов Д.С., Микуляк А.И., Сенжапов И.Я., Белик А.О., Гаранян Д.Н. Отдаленные результаты аппроксимации папиллярных мышц у пациентов с выраженной сердечной недостаточностью вследствие ишемической митральной регургитации. Грудная и сердечно-сосудистая хирургия. 2023;65(2):182-190. https://doi.org/10.24022/0236-2791-2023-65-2-182-190 Bazylev V.V., Tungusov D.S., Mikulyak A.I., Senzhapov I.Ya., Belik A.O., Garanyan D.N. Long-term results of papillary muscle approximation in patients with severe heart failure due to ischemic mitral regurgitation. Russian Journal of Thoracic and Cardiovascular Surgery. 2023;65(2):182-190. (In Russ.) https://doi.org/10.24022/0236-2791-2023-65-2-182-190
- Жбанов И.В., Ревишвили Г.А., Ван Е.Ю., Кулагина Т.Ю., Шабалкин Б.В. Отдаленные результаты хирургического лечения больных с ишемической болезнью сердца, осложненной ишемической митральной недостаточностью. Кардиология и сердечно-сосудистая хирургия. 2022;15(4):393-401. https://doi.org/10.17116/kardio202215041393 Zhbanov I.V., Revishvili G.A., Van E.Yu., Kulagina T.Yu., Shabalkin B.V. Long-term postoperative outcomes in patients with coronary artery disease and ischemic mitral insufficiency. Russian Journal of Cardiology and Cardiovascular Surgery. 2022;15(4):393-401. (In Russ.) https://doi.org/10.17116/kardio202215041393
- Чернявский А.М., Разумахин Р.А., Эфендиев В.У., Рузматов Т.М., Подсосникова Т.Н., Волокитина Т.Л., Матвеева Н.В. Отдаленные результаты хирургического лечения умеренной ишемической митральной недостаточности у пациентов с сохраненной фракцией выброса левого желудочка. Патология кровообращения и кардиохирургия. 2015;19(2):63-71. Cherniavsky A.M., Razumakhin R.A., Efendiev V.U., Ruzmatov T.M., Podsosnikova T.N., Volokitina T.L., Matveyeva N.V. Remote results of surgical treatment of moderate ischemic mitral regurgitation in patients with normal left ventricle function. Patologiya Krovoobrashcheniya i Kardiokhirurgiya = Circulation Pathology and Cardiac Surgery. 2015;19(2):63-71. (In Russ.)
- Суханов С.Г., Орехова Е.Н., Науменко И.Е., Матановская Т.В. Динамика продольной систолической деформации и симптомов хронической сердечной недостаточности у пациентов до и после хирургической реваскуляризации в сочетании с коррекцией ишемической митральной недостаточности. Патология кровообращения и кардиохирургия. 2015;19(1):43-50. Sukhanov S.G., Orekhova E.N., Naumenko I.Ye., Matanovskaya T.V. Systolic longitudinal strain and congestive heart failure in patients with moderate ischemic mitral insufficiency before and after surgical revascularization and mitral annuloplasty. Patologiya Krovoobrashcheniya i Kardiokhirurgiya = Circulation Pathology and Cardiac Surgery. 2015;19(1):43-50. (In Russ.)

