Endovascular treatment of aortic valve stenosis in combination with coronary artery disease: a systematic review
Published 2024-08-30
Keywords
- Aortic Stenosis,
- Coronary Artery Disease,
- Percutaneous Coronary Intervention,
- Transcatheter Aortic Valve Implantation
How to Cite
Copyright (c) 2024 Alekian B.G., Titov N.S.

This work is licensed under a Creative Commons Attribution 4.0 International License.
Abstract
Objective: To evaluate and compare the efficacy and safety of simultaneous and staged techniques of percutaneous coronary interventions (PCI) and transcatheter aortic valve implantation (TAVI).
Methods: The search for sources was carried out in the PubMed, Google Scholar and Cochrane Library databases using keywords. We selected the most cited studies on strategies for endovascular treatment of patients with coronary artery disease and aortic stenosis with the focus on simultaneous and staged techniques of PCI and TAVI. Most attention has been paid to indicators of survival, complications and other study endpoints. The significance of the order of the interventions on patient outcomes was assessed.
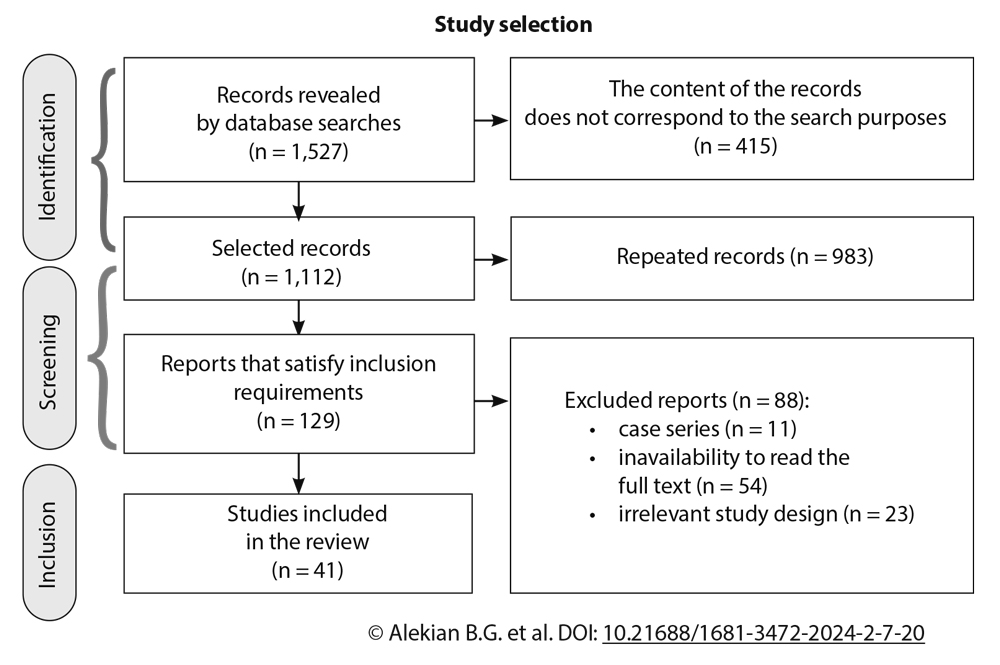
Results: Searching with keywords in the selected databases revealed 1,527 original sources and 60 of them were taken into the review. The selected sources included prospective and retrospective studies as well as the latest guidelines of professional societies on cardiovascular diseases, statistics of surgical interventions and morbidity, and basic researches. In approximately 70% of cases, a staged technique was used with initial putting into practice of PCI followed by TAVI. Most studies comparing selected techniques did not reveal a significant difference in endpoints; at the hospital period their frequency was usually within 3%, and at the long-term period they reached 30%. Nevertheless, a detailed analysis of the frequency of certain control points revealed contradictions in a number of studies.
Conclusion: Despite intensive research into the effects of simultaneous and staged techniques of PCI and TAVI, the point of which approach is better remains disputable. The order of interventions is not reflected in current guidelines, majority of studies are retrospective, and their conclusions are ambiguous. Additional prospective studies are needed to determine the categories of patients who will benefit most from a particular order of PCI and TAVI.
Received 9 April 2024. Revised 19 May 2024. Accepted 2 July 2024.
Funding
The study did not have sponsorship.
Conflict of interest
The authors declare no conflict of interest.
Contribution of the authors
The authors contributed equally to this article.
References
- Shang M., Kahler-Quesada A., Mori M., Yousef S., Geirsson A., Vallabhajosyula P. Progression of aortic stenosis in patients with bicuspid aortic valve. J Card Surg. 2021;36(12):4665-4672. PMID: 34585444. https://doi.org/10.1111/jocs.16026
- Okor I., Bob-Manuel T., Garikapati K., Baldawi H., Gillies C., Ibebuogu U.N. Transcatheter aortic valve replacement in rheumatic aortic stenosis: a comprehensive review. Curr Probl Cardiol. 2021;46(12):100843. PMID: 33994024. https://doi.org/10.1016/j.cpcardiol.2021.100843
- Burdeynaya A.L., Afanasieva O.I., Ezhov M.V., Klesareva E.A., Saidova M.A., Pokrovsky S.N. Lipoprotein(a) and its autoantibodies in association with calcific aortic valve stenosis. Diseases. 2023;11(1):43. PMID: 36975592; PMCID: PMC10047835. https://doi.org/10.3390/diseases11010043
- Stritzke J., Linsel-Nitschke P., Markus M.R.P., Mayer B., Lieb W., Luchner A., Döring A., Koenig W., Keil U., Hense H.-W., Schunkert H.; MONICA/KORA Investigators. Association between degenerative aortic valve disease and long-term exposure to cardiovascular risk factors: results of the longitudinal population-based KORA/MONICA survey. Eur Heart J. 2009;30(16):2044-2053. PMID: 19608594. https://doi.org/10.1093/eurheartj/ehp287
- Vahanian A., Beyersdorf F., Praz F., Milojevic M., Baldus S., Bauersachs J., Capodanno D., Conradi L., De Bonis M., De Paulis R., Delgado V., Freemantle N., Gilard M., Haugaa K.H., Jeppsson A., Jüni P., Pierard L., Prendergast B.D., Sádaba J.R., Tribouilloy C., Wojakowski W.; ESC/EACTS Scientific Document Group. 2021 ESC/EACTS Guidelines for the management of valvular heart disease. Eur Heart J. 2022;43(7):561-632. Erratum in: Eur Heart J. 2022;43(21):2022. PMID: 34453165. https://doi.org/10.1093/eurheartj/ehab395
- Neumann F.J., Sousa-Uva M., Ahlsson A., Alfonso F., Banning A.P., Benedetto U., Byrne R.A., Collet J.-P., Falk V., Head S.J., Jüni P., Kastrati A., Koller A., Kristensen S.D., Niebauer J., Richter D.J., Seferovic P.M., Sibbing D., Stefanini G.G., Windecker S., Yadav R., Zembala M.O.; ESC Scientific Document Group. 2018 ESC/EACTS Guidelines on myocardial revascularization. Eur Heart J. 2019;40(2):87-165. Erratum in: Eur Heart J. 2019;40(37):3096. PMID: 30165437. https://doi.org/10.1093/eurheartj/ehy394
- Otto C.M., Nishimura R.A., Bonow R.O., Carabello B.A., Erwin J.P. 3rd, Gentile F., Jneid H., Krieger E.V., Mack M., McLeod C., O'Gara P.T., Rigolin V.H., Sundt T.M. 3rd, Thompson A., Toly C. 2020 ACC/AHA Guideline for the management of patients with valvular heart disease: executive summary: a report of the American College of Cardiology/American Heart Association Joint Committee on Clinical Practice Guidelines. Circulation. 2021;143(5):e35-e71. Erratum in: Circulation. 2021;143(5):e228. Erratum in: Circulation. 2021;143(10):e784. PMID: 33332149. https://doi.org/10.1161/CIR.0000000000000932
- Vaduganathan M., Mensah G., Turco J., Fuster V., Roth G.A. The global burden of cardiovascular diseases and risk: A сompass for future health. J Am Coll Cardiol. 2022;80(25):2361-2371. PMID: 36368511. https://doi.org/10.1016/j.jacc.2022.11.005
- Окладников С.М., Никитина С.Ю., Александрова Г.А., Ахметзянова Р.Р., Голубев Н.А., Кириллова Г.Н., Огрызко Е.В., Оськов Ю.И., Романенко О.И., Харькова Т.Л., Чумарина В.Ж. Здравоохранение в России. 2023: стат. сб. М.: Росстат, 2023. 179 с. Okladnikov S.M., Nikitina S.Yu., Aleksandrova G.A., Ahmetzyanova R.R., Golubev N.A., Kirillova G.N., Ogryzko E.V., Oskov Yu.I., Romanenko O.I., Harkova T.L., Chumarina V.Zh. Healthcare in Russia. 2023. Statistical collection. Moscow: Rosstat Publ.; 2023. 179 p.
- Lindman B.R., Clavel M.-A., Mathieu P., Iung B., Lancellotti P., Otto C.M., Pibarot P. Calcific aortic stenosis. Nat Rev Dis Primers. 2016;2:16006. PMID: 27188578; PMCID: PMC5127286. https://doi.org/10.1038/nrdp.2016.6
- Sharma T., Krishnan A.M., Lahoud R., Polomsky M., Dauerman H.L. National trends in TAVR and SAVR for patients with severe isolated aortic stenosis. J Am Coll Cardiol. 2022;80(21):2054-2056. PMID: 36122626. https://doi.org/10.1016/j.jacc.2022.08.787
- Бокерия Л.А., Милиевская Е.Б., Прянишников В.В., Юрлов И.А. Сердечно-сосудистая хирургия – 2022. Болезни и врожденные аномалии системы кровообращения. М.: НМИЦ ССХ им. А.Н. Бакулева Минздрава России, 2023. 344 с. Bokeriya L.A., Milievskaya E.B., Pryanishnikov V.V., Yurlov I.A. Cardiovascular surgery – 2022. Diseases and congenital anomalies of the circulatory system. Moscow: Bakulev National Medical Research Center for Cardiovascular Surgery Publ.; 2023. 344 p. (In Russ.)
- Алекян Б.Г., Григорьян А.М., Стаферов А.В., Карапетян Н.Г. Рентгенэндоваскулярная диагностика и лечение заболеваний сердца и сосудов в Российской Федерации – 2021 год. Эндоваскулярная хирургия. Специальный выпуск. 2022;9:S5-S254. https://doi.org/10.24183/2409-4080-2022-9S-S5-S254 Alekyan B.G., Grigoryan A.M., Staferov A.V., Karapetyan N.G. X-ray endovascular diagnosis and treatment of heart and vascular diseases in the Russian Federation — 2021. Endovaskulyarnaya hirurgiya = Russian Journal of Endovascular Surgery. Special Edition. 2022;9:S5-S254. (In Russ.) https://doi.org/10.24183/2409-4080-2022-9S-S5-S254
- de Azevedo Filho A.F., Accorsi T.A., Ribeiro H.B. Coronary artery disease in patients with aortic stenosis and transcatheter aortic valve implantation: implications for management. Eur Cardiol. 2021;16:e49. PMID: 34950245; PMCID: PMC8674631. https://doi.org/10.15420/ecr.2021.27
- Popma J.J., Adams D.H., Reardon M.J., Yakubov S.J., Kleiman N.S., Heimansohn D., Hermiller J. Jr, Hughes G.C., Harrison J.K., Coselli J., Diez J., Kafi A., Schreiber T., Gleason T.G., Conte J., Buchbinder M., Deeb G.M., Carabello B., Serruys P.W., Chenoweth S., Oh J.K.; CoreValve United States Clinical Investigators. Transcatheter aortic valve replacement using a self-expanding bioprosthesis in patients with severe aortic stenosis at extreme risk for surgery. J Am Coll Cardiol. 2014;63(19):1972-1981. PMID: 24657695. https://doi.org/10.1016/j.jacc.2014.02.556
- Leon M.B., Smith C.R., Mack M.J., Makkar R.R., Svensson L.G., Kodali S.K., Thourani V.H., Tuzcu E.M., Miller D.C., Herrmann H.C., Doshi D., Cohen D.J., Pichard A.D., Kapadia S., Dewey T., Babaliaros V., Szeto W.Y., Williams M.R., Kereiakes D., Zajarias A., Greason K.L., Whisenant B.K., Hodson R.W., Moses J.W., Trento A., Brown D.L., Fearon W.F., Pibarot P., Hahn R.T., Jaber W.A., Anderson W.N., Alu M.C., Webb J.G.; PARTNER 2 Investigators. Transcatheter or surgical aortic-valve replacement in intermediate-risk patients. N Engl J Med. 2016;374(17):1609-1620. PMID: 27040324. https://doi.org/10.1056/NEJMoa1514616
- Yang Y., Huang F.-Y., Huang B.-T., Xiong T.-Y., Pu X.-B., Chen S.-J., Chen M., Feng Y. The safety of concomitant transcatheter aortic valve replacement and percutaneous coronary intervention: a systematic review and meta-analysis. Medicine (Baltimore). 2017;96(48):e8919. PMID: 29310382; PMCID: PMC5728783. https://doi.org/10.1097/MD.0000000000008919
- Kotronias R.A., Kwok C.S., George S., Capodanno D., Ludman P.F., Townend J.N., Doshi S.N., Khogali S.S., Généreux P., Herrmann H.C., Mamas M.A., Bagur R. Transcatheter aortic valve implantation with or without percutaneous coronary artery revascularization strategy: a systematic review and meta-analysis. J Am Heart Assoc. 2017;6(6):e005960. PMID: 28655733; PMCID: PMC5669191. https://doi.org/10.1161/JAHA.117.005960
- Gohmann R.F., Lauten P., Seitz P., Krieghoff C., Lücke C., Gottschling S., Mende M., Weiß S., Wilde J., Kiefer P., Noack T., Desch S., Holzhey D., Borger M.A., Thiele H., Abdel-Wahab M., Gutberlet M. Combined coronary CT-Angiography and TAVI-planning: a contrast-neutral routine approach for ruling-out significant coronary artery disease. J Clin Med. 2020;9(6):1623. PMID: 32471233; PMCID: PMC7356559. https://doi.org/10.3390/jcm9061623
- Malebranche D., Hoffner M.K.M., Huber A.T., Cicovic A., Spano G., Bernhard B., Bartkowiak J., Okuno T., Lanz J., Räber L., Praz F., Stortecky S., Windecker S., Pilgrim T., Gräni C. Diagnostic performance of quantitative coronary artery disease assessment using computed tomography in patients with aortic stenosis undergoing transcatheter aortic-valve implantation. BMC Cardiovasc Disord. 2022;22(1):178. PMID: 35436856; PMCID: PMC9014581. https://doi.org/10.1186/s12872-022-02623-8
- Matsumoto S., Yamada Y., Hashimoto M., Okamura T., Yamada M., Yashima F., Hayashida K., Fukuda K., Jinzaki M. CT imaging before transcatheter aortic valve implantation (TAVI) using variable helical pitch scanning and its diagnostic performance for coronary artery disease. Eur Radiol. 2017;27(5):1963-1970. PMID: 27562479. https://doi.org/10.1007/s00330-016-4547-4
- Patel M.R., Calhoon J.H., Dehmer G.J., Grantham J.A., Maddox T.M., Maron D.J., Smith P.K. ACC/AATS/AHA/ASE/ASNC/SCAI/SCCT/STS 2017 appropriate use criteria for coronary revascularization in patients with stable ischemic heart disease: a report of the American College of Cardiology Appropriate Use Criteria Task Force, American Association for Thoracic Surgery, American Heart Association, American Society of Echocardiography, American Society of Nuclear Cardiology, Society for Cardiovascular Angiography and Interventions, Society of Cardiovascular Computed Tomography, and Society of Thoracic Surgeons. J Nucl Cardiol. 2017;24(5):1759-1792. Erratum in: J Nucl Cardiol. 2018;25(6):2191-2192. PMID: 28608183. https://doi.org/10.1007/s12350-017-0917-9
- Francone M., Budde R.P.J., Bremerich J., Dacher J.N., Loewe C., Wolf F., Natale L., Pontone G., Redheuil A., Vliegenthart R., Nikolaou K., Gutberlet M., Salgado R. CT and MR imaging prior to transcatheter aortic valve implantation: standardisation of scanning protocols, measurements and reporting-a consensus document by the European Society of Cardiovascular Radiology (ESCR). Eur Radiol. 2020;30(5):2627-2650. Erratum in: Eur Radiol. 2020;30(7):4143-4144. PMID: 31489471; PMCID: PMC7160220. https://doi.org/10.1007/s00330-019-06357-8
- Blanke P., Weir-McCall J.R., Achenbach S., Delgado V., Hausleiter J., Jilaihawi H., Marwan M., Nørgaard B.L., Piazza N., Schoenhagen P., Leipsic J.A. Computed tomography imaging in the context of Transcatheter Aortic Valve Implantation (TAVI)/Transcatheter Aortic Valve Replacement (TAVR): an expert consensus document of the Society of Cardiovascular Computed Tomography. JACC Cardiovasc Imaging. 2019;12(1):1-24. PMID: 30621986. https://doi.org/10.1016/j.jcmg.2018.12.003
- Knaapen P. Computed tomography to replace invasive coronary angiography? Circ Cardiovasc Imaging. 2019;12(2):e008710. PMID: 30764640. https://doi.org/10.1161/CIRCIMAGING.119.008710
- Mylotte D., Wijns W. Anatomical or functional assessment of coronary artery disease in aortic stenosis: haven't we been down this road before? J Am Heart Assoc. 2019;8(22):e014367. PMID: 31718440; PMCID: PMC6915286. https://doi.org/10.1161/JAHA.119.014367
- Barone-Rochette G., Piérard S., Seldrum S., de Meester de Ravenstein C., Melchior J., Maes F., Pouleur A.-C., Vancraeynest D., Pasquet A., Vanoverschelde J.-L., Gerber B.L. Aortic valve area, stroke volume, left ventricular hypertrophy, remodeling, and fibrosis in aortic stenosis assessed by cardiac magnetic resonance imaging: comparison between high and low gradient and normal and low flow aortic stenosis. Circ Cardiovasc Imaging. 2013;6(6):1009-1017. PMID: 24100045. https://doi.org/10.1161/CIRCIMAGING.113.000515
- Aleksandric S., Banovic M., Beleslin B. Challenges in diagnosis and functional assessment of coronary artery disease in patients with severe aortic stenosis. Front Cardiovasc Med. 2022;9:849032. PMID: 35360024; PMCID: PMC8961810. https://doi.org/10.3389/fcvm.2022.849032
- Vendrik J., Ahmad Y., Eftekhari A., Howard J.P., Wijntjens G.W.M., Stegehuis V.E., Cook C., Terkelsen C.J., Christiansen E.H., Koch K.T., Piek J.J., Sen S., Baan J. Jr. Long-term effects of transcatheter aortic valve implantation on coronary hemodynamics in patients with concomitant coronary artery disease and severe aortic stenosis. J Am Heart Assoc. 2020;9(5):e015133. PMID: 32102615; PMCID: PMC7335578. https://doi.org/10.1161/JAHA.119.015133
- Scarsini R., Pesarini G., Lunardi M., Piccoli A., Zanetti C., Cantone R., Bellamoli M., Ferrero V., Gottin L., Faggian G., Ribichini F. Observations from a real-time, iFR-FFR "hybrid approach" in patients with severe aortic stenosis and coronary artery disease undergoing TAVI. Cardiovasc Revasc Med. 2018;19(3 Pt B):355-359. PMID: 29113864. https://doi.org/10.1016/j.carrev.2017.09.019
- Rajiah P., Cummings K.W., Williamson E., Young P.M. CT fractional flow reserve: a practical guide to application, interpretation, and problem solving. Radiographics. 2022;42(2):340-358. PMID: 35119968. https://doi.org/10.1148/rg.210097
- Tarantini G., Tang G., Nai Fovino L., Blackman D., Van Mieghem N.M., Kim W.-K., Karam N., Carrilho-Ferreira P., Fournier S., Pręgowski J., Fraccaro C., Vincent F., Teles R.C., Mylotte D., Wong I., Bieliauskas G., Czerny M., Bonaros N., Parolari A., Dudek D., Tchetche D., Eltchaninoff H., de Backer O., Stefanini G., Sondergaard L. Management of coronary artery disease in patients undergoing transcatheter aortic valve implantation. A clinical consensus statement from the European Association of Percutaneous Cardiovascular Interventions in collaboration with the ESC Working Group on Cardiovascular Surgery. EuroIntervention. 2023;19(1):37-52. PMID: 36811935; PMCID: PMC10174192. https://doi.org/10.4244/EIJ-D-22-00958
- Tran Z., Hadaya J., Downey P., Sanaiha Y., Verma A., Shemin R.J., Benharash P. Staged versus concomitant transcatheter aortic valve replacement and percutaneous coronary intervention: A national analysis. JTCVS Open. 2022;10:148-161. PMID: 36004248; PMCID: PMC9390561. https://doi.org/10.1016/j.xjon.2022.02.019
- Ochiai T., Yoon S.-H., Flint N., Sharma R., Chakravarty T., Kaewkes D., Patel V., Nakamura M., Cheng W., Makkar R. Timing and outcomes of percutaneous coronary intervention in patients who underwent transcatheter aortic valve implantation. Am J Cardiol. 2020;125(9):1361-1368. PMID: 32106928. https://doi.org/10.1016/j.amjcard.2020.01.043
- Barbanti M., Todaro D., Costa G., Pilato G., Picci A., Gulino S., Capranzano P., La Spina K., Di Simone E., D'Arrigo P., Deste W., Indelicato A., Cannata S., Giannazzo D., Immè S., Tamburino C., Patanè M., Buccheri S., Capodanno D., Sgroi C., Tamburino C. Optimized screening of coronary artery disease with invasive coronary angiography and ad hoc percutaneous coronary intervention during transcatheter aortic valve replacement. Circ Cardiovasc Interv. 2017;10(8):e005234. PMID: 28768757. https://doi.org/10.1161/CIRCINTERVENTIONS.117.005234
- Rheude T., Costa G., Ribichini F.L., Pilgrim T., Santos I.J.A., De Backer O., Kim W.-K., Ribeiro H.B., Saia F., Bunc M., Tchétché D., Garot P., Mylotte D., Burzotta F., Watanabe Y., Bedogni F., Tesorio T., Tocci M., Franzone A., Valvo R., Savontaus M., Wienemann H., Porto I., Gandolfo C., Iadanza A., Bortone A.S., Mach M., Latib A., Biasco L., Taramasso M., Zimarino M., Tomii D., Nuyens P., Sondergaard L., Camara S.F., Palmerini T., Orzalkiewicz M., Steblovnik K., Degrelle B., Gautier A., Del Sole P.A., Mainardi A., Pighi M., Lunardi M., Kawashima H., Criscione E., Cesario V., Biancari F., Zanin F., Esposito G., Adam M., Grube E., Baldus S., De Marzo V., Piredda E., Cannata S., Iacovelli F., Andreas M., Frittitta V., Dipietro E., Reddavid C., Strazzieri O., Motta S., Angellotti D., Sgroi C., Xhepa E., Kargoli F., Tamburino C., Joner M., Barbanti M. Comparison of different percutaneous revascularisation timing strategies in patients undergoing transcatheter aortic valve implantation. EuroIntervention. 2023;19(7):589-599. PMID: 37436190; PMCID: PMC10495747. https://doi.org/10.4244/EIJ-D-23-00186
- Barbanti M., Costa G., Picci A., Criscione E., Reddavid C., Valvo R., Todaro D., Deste W., Condorelli A., Scalia M., Licciardello A., Politi G., De Luca G., Strazzieri O., Motta S., Garretto V., Veroux P., Giaquinta A., Giuffrida A., Sgroi C., Leon M.B., Webb J.G., Tamburino C. Coronary cannulation after transcatheter aortic valve replacement: the RE-ACCESS study. JACC Cardiovasc Interv. 2020;13(21):2542-2555. PMID: 33069648. https://doi.org/10.1016/j.jcin.2020.07.006
- Faroux L., Lhermusier T., Vincent F., Nombela-Franco L., Tchétché D., Barbanti M., Abdel-Wahab M., Windecker S., Auffret V., Campanha-Borges D.C., Fischer Q., Muñoz-Garcia E., Trillo-Nouche R., Jorgensen T., Serra V., Toggweiler S., Tarantini G., Saia F., Durand E., Donaint P., Gutierrez-Ibanes E., Wijeysundera H.C., Veiga G., Patti G., D'Ascenzo F., Moreno R., Hengstenberg C., Chamandi C., Asmarats L., Hernandez-Antolin R., Gomez-Hospital J.A., Cordoba-Soriano J.G., Landes U., Jimenez-Diaz V.A., Cruz-Gonzalez I., Nejjari M., Roubille F., Van Belle É., Armijo G., Siddiqui S., Costa G., Elsaify S., Pilgrim T., le Breton H., Urena M., Muñoz-Garcia A.J., Sondergaard L., Bach-Oller M., Fraccaro C., Eltchaninoff H., Metz D., Tamargo M., Fradejas-Sastre V., Rognoni A., Bruno F., Goliasch G., Santaló-Corcoy M., Jimenez-Mazuecos J., Webb J.G., Muntané-Carol G., Paradis J.-M., Mangieri A., Ribeiro H.B., Campelo-Parada F., Rodés-Cabau J. ST-segment elevation myocardial infarction following transcatheter aortic valve replacement. J Am Coll Cardiol. 2021;77(17):2187-2199. PMID: 33926655. https://doi.org/10.1016/j.jacc.2021.03.014
- Yap J.J.L., Ho K.W. Managing complex coronary access after transcatheter aortic valve implantation. Journal of Asian Pacific Society of Cardiology. 2023;2:e11. https://doi.org/10.15420/japsc.2022.28
- Lunardi M., Venturi G., Del Sole P.A., Ruzzarin A., Mainardi A., Pighi M., Pesarini G., Scarsini R., Tavella D., Gottin L., Ribichini F.L. Optimal timing for percutaneous coronary intervention in patients undergoing transcatheter aortic valve implantation. Int J Cardiol. 2022;365:114-122. PMID: 35870638. https://doi.org/10.1016/j.ijcard.2022.07.030
- Masson J.B., Lee M., Boone R.H., Al Ali A., Al Bugami S., Hamburger J., Mancini G.B.J., Ye J., Cheung A., Humphries K.H., Wood D., Nietlispach F., Webb J.G. Impact of coronary artery disease on outcomes after transcatheter aortic valve implantation. Catheter Cardiovasc Interv. 2010;76(2):165-173. PMID: 20665855. https://doi.org/10.1002/ccd.22501
- Ussia G.P., Barbanti M., Colombo A., Tarantini G., Petronio A.S., Ettori F., Ramondo A., Santoro G., Klugmann S., Bedogni F., Antoniucci D., Maisano F., Marzocchi A., Poli A., De Carlo M., Fiorina C., De Marco F., Napodano M., Violini R., Bortone A.S., Tamburino C.; CoreValve Italian Registry Investigators. Impact of coronary artery disease in elderly patients undergoing transcatheter aortic valve implantation: insight from the Italian CoreValve Registry. Int J Cardiol. 2013;167(3):943-950. PMID: 22459391. https://doi.org/10.1016/j.ijcard.2012.03.089
- Dewey T.M., Brown D.L., Herbert M.A., Culica D., Smith C.R., Leon M.B., Svensson L.G., Tuzcu M., Webb J.G., Cribier A., Mack M.J. Effect of concomitant coronary artery disease on procedural and late outcomes of transcatheter aortic valve implantation. Ann Thorac Surg. 2010;89(3):758-767. PMID: 20172123. https://doi.org/10.1016/j.athoracsur.2009.12.033
- Khawaja M.Z., Asrress K.N., Haran H., Arri S., Nadra I., Bolter K., Wilson K., Clack L., Hancock J., Young C.P., Bapat V., Thomas M., Redwood S. The effect of coronary artery disease defined by quantitative coronary angiography and SYNTAX score upon outcome after transcatheter aortic valve implantation (TAVI) using the Edwards bioprosthesis. EuroIntervention. 2015;11(4):450-455. PMID: 24832041. https://doi.org/10.4244/EIJY14M05_09
- Sankaramangalam K., Banerjee K., Kandregula K., Mohananey D., Parashar A., Jones B.M., Jobanputra Y., Mick S., Krishnaswamy A., Svensson L.G., Kapadia S.R. Impact of coronary artery disease on 30-day and 1-year mortality in patients undergoing transcatheter aortic valve replacement: a meta-analysis. J Am Heart Assoc. 2017;6(10):e006092. PMID: 29021275; PMCID: PMC5721835. https://doi.org/10.1161/JAHA.117.006092
- D'Ascenzo F., Verardi R., Visconti M., Conrotto F., Scacciatella P., Dziewierz A., Stefanini G.G., Paradis J.-M., Omedè P., Kodali S., D'Amico M., Rinaldi M., Salizzoni S. Independent impact of extent of coronary artery disease and percutaneous revascularisation on 30-day and one-year mortality after TAVI: a meta-analysis of adjusted observational results. EuroIntervention. 2018;14(11):e1169-e1177. PMID: 30082258. https://doi.org/10.4244/EIJ-D-18-00098
- Abdel-Wahab M., Mostafa A.E., Geist V., Stöcker B., Gordian K., Merten C., Richardt D., Toelg R., Richardt G. Comparison of outcomes in patients having isolated transcatheter aortic valve implantation versus combined with preprocedural percutaneous coronary intervention. Am J Cardiol. 2012;109(4):581-586. PMID: 22133754. https://doi.org/10.1016/j.amjcard.2011.09.053
- Goel S.S., Agarwal S., Tuzcu E.M., Ellis S.G., Svensson L.G., Zaman T., Bajaj N., Joseph L., Patel N.S., Aksoy O., Stewart W.J., Griffin B.P., Kapadia S.R. Percutaneous coronary intervention in patients with severe aortic stenosis: implications for transcatheter aortic valve replacement. Circulation. 2012;125(8):1005-1013. PMID: 22282327. https://doi.org/10.1161/CIRCULATIONAHA.111.039180
- Lateef N., Khan M.S., Deo S.V., Yamani N., Riaz H., Virk H.U.H., Khan S.U., Hedrick D.P., Kanaan A., Reed G.W., Krishnaswamy A., Puri R., Kapadia S.R., Kalra A. Meta-analysis comparing outcomes in patients undergoing transcatheter aortic valve implantation with versus without percutaneous coronary intervention. Am J Cardiol. 2019;124(11):1757-1764. PMID: 31575422; PMCID: PMC7453960. https://doi.org/10.1016/j.amjcard.2019.08.024
- Patterson T., Clayton T., Dodd M., Khawaja Z., Morice M.C., Wilson K., Kim W.-K., Meneveau N., Hambrecht R., Byrne J., Carrié D., Fraser D., Roberts D.H., Doshi S.N., Zaman A., Banning A.P., Eltchaninoff H., Le Breton H., Smith D., Cox I., Frank D., Gershlick A., de Belder M., Thomas M., Hildick-Smith D., Prendergast B., Redwood S.; ACTIVATION Trial Investigators. ACTIVATION (PercutAneous Coronary inTervention prIor to transcatheter aortic VAlve implantaTION): a randomized clinical trial. JACC Cardiovasc Interv. 2021;14(18):1965-1974. PMID: 34556269. https://doi.org/10.1016/j.jcin.2021.06.041
- Costa G., Pilgrim T., Amat Santos I.J., De Backer O., Kim W.-K., Ribeiro H.B., Saia F., Bunc M., Tchetche D., Garot P., Ribichini F.L., Mylotte D., Burzotta F., Watanabe Y., De Marco F., Tesorio T., Rheude T., Tocci M., Franzone A., Valvo R., Savontaus M., Wienemann H., Porto I., Gandolfo C., Iadanza A., Bortone A.S., Mach M., Latib A., Biasco L., Taramasso M., Zimarino M., Tomii D., Nuyens P., Sondergaard L., Camara S.F., Palmerini T., Orzalkiewicz M., Steblovnik K., Degrelle B., Gautier A., Del Sole P.A., Mainardi A., Pighi M., Lunardi M., Kawashima H., Criscione E., Cesario V., Biancari F., Zanin F., Joner M., Esposito G., Adam M., Grube E., Baldus S., De Marzo V., Piredda E., Cannata S., Iacovelli F., Andreas M., Frittitta V., Dipietro E., Reddavid C., Strazzieri O., Motta S., Angellotti D., Sgroi C., Kargoli F., Tamburino C., Barbanti M.; REVASC-TAVI Registry. Management of myocardial revascularization in patients with stable coronary artery disease undergoing transcatheter aortic valve implantation. Circ Cardiovasc Interv. 2022;15(12):e012417. PMID: 36538579. https://doi.org/10.1161/CIRCINTERVENTIONS.122.012417
- Paradis J.M., White J.M., Généreux P., Urena M., Doshi D., Nazif T., Hahn R., George I., Khalique O., Harjai K., Lasalle L., Labbé B.M., DeLarochellière R., Doyle D., Dumont É., Mohammadi S., Leon M.B., Rodés-Cabau J., Kodali S. Impact of coronary artery disease severity assessed with the SYNTAX Score on outcomes following transcatheter aortic valve replacement. J Am Heart Assoc. 2017;6(2):e005070. PMID: 28219920; PMCID: PMC5523783. https://doi.org/10.1161/JAHA.116.005070
- Ramee S., Anwaruddin S., Kumar G., Piana R.N., Babaliaros V., Rab T., Klein L.W.; Aortic Stenosis AUC Writing Group; Interventional Section of the Leadership Council of the American College of Cardiology. The rationale for performance of coronary angiography and stenting before transcatheter aortic valve replacement: from the Interventional Section Leadership Council of the American College of Cardiology. JACC Cardiovasc Interv. 2016;9(23):2371-2375. PMID: 27931592. https://doi.org/10.1016/j.jcin.2016.09.024
- Rosseel L., Mylotte D., Cosyns B., Vanhaverbeke M., Zweiker D., Teles R.C., Angerås O., Neylon A., Rudolph T.K., Wykrzykowska J.J., Patterson T., Costa G., Ojeda S., Tzikas A., Abras M., Leroux L., Van Belle E., Tchétché D., Bleiziffer S., Swaans M.J., Parma R., Blackman D.J., Van Mieghem N.M., Grygier M., Redwood S., Prendergast B., Van Camp G., De Backer O. Contemporary European practice in transcatheter aortic valve implantation: results from the 2022 European TAVI Pathway Registry. Front Cardiovasc Med. 2023;10:1227217. PMID: 37645516; PMCID: PMC10461475. https://doi.org/10.3389/fcvm.2023.1227217

