The relationship between diastolic function characteristics and severe myocardial injury in coronary artery bypass graft surgery: a retrospective cohort study
Published 2024-08-30
Keywords
- Cardiopulmonary Bypass,
- Coronary Artery Bypass,
- Echocardiography,
- Retrospective Studies,
- Troponin I
How to Cite
Copyright (c) 2024 Efremov S.M., Shmidt R.E., Zyryanova A.V., Shmidt T.A., Kamenskih M.S., Shmatov D.V.

This work is licensed under a Creative Commons Attribution 4.0 International License.
Abstract
Introduction: The clinical significance of parameters characterizing left ventricular diastolic function after cardiac surgery has not been sufficiently studied.
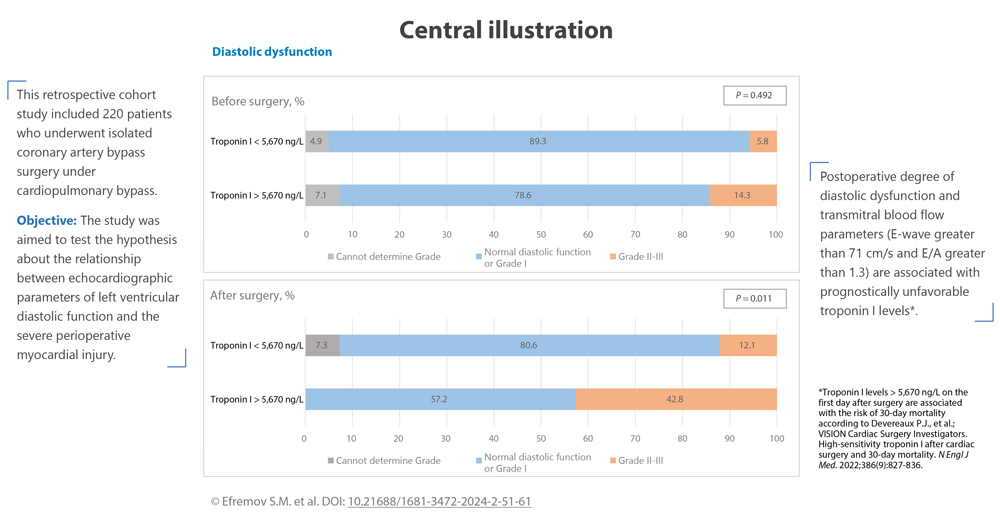
Objective: The study was aimed to test the hypothesis about the relationship between echocardiographic parameters of left ventricular diastolic function and the severe perioperative myocardial injury.
Methods: This retrospective cohort study included 220 patients who underwent isolated coronary artery bypass surgery under cardiopulmonary bypass. We analyzed the degree of diastolic dysfunction, and transmittal blood flow characteristics including left ventricular early diastolic filling velocity (E-wave), and the ratio of E-wave to left atrial systole filling velocity (E/A), left atrial volume index, tricuspid regurgitation velocity, mean mitral valve annulus velocity (e'), and E/e' ratio according to echocardiography before and after surgery. Severe perioperative myocardial injury (the primary outcome) was identified when the high-sensitivity troponin I concentration reached a level greater than 5,670 ng/L on the first day after surgery.
Results: ROC analysis showed that E-wave greater than 71 cm/s and E/A greater than 1.3 were associated with severe perioperative myocardial injury. In addition, diastolic dysfunction of grade 2 and 3 was found in 13.1% of patients with postoperative troponin I levels less than 5,670 ng/L and in 42.9% of patients with levels greater than 5,670 ng/L (P = 0.009).
Conclusion: Postoperative degree of diastolic dysfunction and transmitral blood flow parameters are associated with prognostically unfavorable troponin I levels.
Received 26 January 2024. Revised 31 July 2024. Accepted 2 August 2024.
Funding
The study did not have sponsorship.
Conflict of interest
The authors declare no conflict of interest.
Contribution of the authors
Conception and study design: S.M. Efremov
Data collection and analysis: S.M. Efremov, R.E. Shmidt, T.A. Shmidt, A.V. Zyryanova
Statistical analysis: S.M. Efremov, R.E. Shmidt
Drafting the article: S.M. Efremov, R.E. Shmidt, A.V. Zyryanova
Critical revision of the article: S.M. Efremov, R.E. Shmidt, A.V. Zyryanova, T.A. Shmidt, M.S. Kamenskih, D.V. Shmatov
Final approval of the version to be published: S.M. Efremov, R.E. Shmidt, A.V. Zyryanova, T.A. Shmidt, M.S. Kamenskih, D.V. Shmatov
References
- Shah A.M., Claggett B., Loehr L.R., Chang P.P., Matsushita K., Kitzman D., Konety S., Kucharska-Newton A., Sueta C.A., Mosley T.H., Wright J.D., Coresh J., Heiss G., Folsom A.R., Solomon S.D. Heart failure stages among older adults in the community: the atherosclerosis risk in communities study. Circulation. 2017;135(3):224-240. PMID: 27881564; PMCID: PMC5241178. https://doi.org/10.1161/CIRCULATIONAHA.116.023361
- Brown J.A., Yousef S., Zhu J., Thoma F., Serna-Gallegos D., Joshi R., Subramaniam K., Kaczorowski D.J., Chu D., Aranda-Michel E., Bianco V., Sultan I. The long-term impact of diastolic dysfunction after routine cardiac surgery. J Cardiothorac Vasc Anesth. 2023;37(6):927-932. PMID: 36863985. https://doi.org/10.1053/j.jvca.2023.01.036
- Cios T.J., Klick J.C., Roberts S.M. Managing diastolic dysfunction perioperatively. Semin Cardiothorac Vasc Anesth. 2023;27(1):42-50. PMID: 36473032; PMCID: PMC9968995. https://doi.org/10.1177/10892532221142441
- Хлопина И.А., Шацова Е.Н., Лупачев В.В., Плакуев А.Н., Чернозёмова А.В., Кубасов Р.В. Характеристика диастолической функции левого желудочка у больных после аортокоронарного шунтирования. Вестник Российской академии медицинских наук. 2015;70(2):196-202. https://doi.org/10.15690/vramn.v70i2.1313 Khlopina I.A., Shatsova E.N., Lupachev V.V., Pakuev A.N., Chernozemova A.V., Kubasov R.V. Characteristics of left ventricular diastolic function in patients before and after coronary artery bypass grafting. Annals of the Russian Academy of Medical Sciences. 2015;70(2):196-202. (In Russ.) https://doi.org/10.15690/vramn.v70i2.1313
- Nagueh S.F., Smiseth O.A., Appleton C.P., Byrd B.F. 3rd, Dokainish H., Edvardsen T., Flachskampf F.A., Gillebert T.C., Klein A.L., Lancellotti P., Marino P., Oh J.K., Popescu B.A., Waggoner A.D. Recommendations for the evaluation of left ventricular diastolic function by echocardiography: An update from the American Society of Echocardiography and the European Association of Cardiovascular Imaging. J Am Soc Echocardiogr. 2016;29(4):277-314. PMID: 27037982. https://doi.org/10.1016/j.echo.2016.01.011
- McDonagh T.A., Metra M., Adamo M., Gardner R.S., Baumbach A., Böhm M., Burri H., Butler J., Čelutkienė J., Chioncel O., Cleland J.G.F., Coats A.J.S., Crespo-Leiro M.G., Farmakis D., Gilard M., Heymans S., Hoes A.W., Jaarsma T., Jankowska E.A., Lainscak M., Lam C.S.P., Lyon A.R., McMurray J.J.V., Mebazaa A., Mindham R., Muneretto C., Francesco Piepoli M., Price S., Rosano G.M.C., Ruschitzka F., Skibelund A.K.; ESC Scientific Document Group. 2021 ESC Guidelines for the diagnosis and treatment of acute and chronic heart failure: Developed by the Task Force for the diagnosis and treatment of acute and chronic heart failure of the European Society of Cardiology (ESC). With the special contribution of the Heart Failure Association (HFA) of the ESC. Eur J Heart Fail. 2022;24(1):4-131. PMID: 35083827. https://doi.org/10.1002/ejhf.2333
- Devereaux P.J., Lamy A., Chan M.T.V., Allard R.V., Lomivorotov V.V., Landoni G., Zheng H., Paparella D., McGillion M.H., Belley-Côté E.P., Parlow J.L., Underwood M.J., Wang C.Y., Dvirnik N., Abubakirov M., Fominskiy E., Choi S., Fremes S., Monaco F., Urrútia G., Maestre M., Hajjar L.A., Hillis G.S., Mills N.L., Margari V., Mills J.D., Billing J.S., Methangkool E., Polanczyk C.A., Sant'Anna R., Shukevich D., Conen D., Kavsak P.A., McQueen M.J., Brady K., Spence J., Le Manach Y., Mian R., Lee S.F., Bangdiwala S.I., Hussain S., Borges F.K., Pettit S., Vincent J., Guyatt G.H., Yusuf S., Alpert J.S., White H.D., Whitlock R.P.; VISION Cardiac Surgery Investigators. High-sensitivity troponin I after cardiac surgery and 30-day mortality. N Engl J Med. 2022;386(9):827-836. PMID: 35235725. https://doi.org/10.1056/NEJMoa2000803
- Lang R.M., Badano L.P., Mor-Avi V., Afilalo J., Armstrong A., Ernande L., Flachskampf F.A., Foster E., Goldstein S.A., Kuznetsova T., Lancellotti P., Muraru D., Picard M.H., Rietzschel E.R., Rudski L., Spencer K.T., Tsang W., Voigt J.-U. Recommendations for cardiac chamber quantification by echocardiography in adults: an update from the American Society of Echocardiography and the European Association of Cardiovascular Imaging. J Am Soc Echocardiogr. 2015;28(1):1-39.e14. PMID: 25559473. https://doi.org/10.1016/j.echo.2014.10.003
- Мингалимова А.Р., Драпкина О.М., Бикбова Н.М., Сагиров М.А., Мазанов М.Х., Тимербаев А.В., Аргир И.А. Госпитальная динамика показателей диастолической функции левого желудочка у пациентов, перенесших операцию коронарного шунтирования. Российский кардиологический журнал. 2022;27(8):4948. https://doi.org/10.15829/1560-4071-2022-4948 Mingalimova A.R., Drapkina O.M., Bikbova N.M., Sagirov M.A., Mazanov M.Kh., Timerbaev A.V., Argir I.A. Inhospital changes of left ventricular diastolic function in patients undergoing coronary bypass surgery. Russian Journal of Cardiology. 2022;27(8):4948. (In Russ.) https://doi.org/10.15829/1560-4071-2022-4948
- Silbiger J.J. Pathophysiology and echocardiographic diagnosis of left ventricular diastolic dysfunction. J Am Soc Echocardiogr. 2019;32(2):216-232.e2. PMID: 30717860. https://doi.org/10.1016/j.echo.2018.11.011
- Chemla D., Coirault C., Hébert J.-L., Lecarpentier Y. Mechanics of relaxation of the human heart. News Physiol Sci. 2000;15:78-83. PMID: 11390883. https://doi.org/10.1152/physiologyonline.2000.15.2.78
- Bernard F., Denault A., Babin D., Goyer C., Couture P., Couturier A., Buithieu J. Diastolic dysfunction is predictive of difficult weaning from cardiopulmonary bypass. Anesth Analg. 2001;92(2):291-298. PMID: 11159219. https://doi.org/10.1097/00000539-200102000-00002
- Metkus T.S., Suarez-Pierre A., Crawford T.C., Lawton J.S., Goeddel L., Dodd-O J., Mukherjee M., Abraham T.P., Whitman G.J. Diastolic dysfunction is common and predicts outcome after cardiac surgery. J Cardiothorac Surg. 2018;13(1):67. PMID: 29903030; PMCID: PMC6003153. https://doi.org/10.1186/s13019-018-0744-3
- Kaw R., Hernandez A.V., Pasupuleti V., Deshpande A., Nagarajan V., Bueno H., Coleman C.I., Ioannidis J.P., Bhatt D.L., Blackstone E.H.; Cardiovascular Meta-analyses Research Group. Effect of diastolic dysfunction on postoperative outcomes after cardiovascular surgery: A systematic review and meta-analysis. J Thorac Cardiovasc Surg. 2016;152(4):1142-1153. PMID: 27364601. https://doi.org/10.1016/j.jtcvs.2016.05.057
- Salem R., Denault A.Y., Couture P., Bélisle S., Fortier A., Guertin M.-C., Carrier M., Martineau R. Left ventricular end-diastolic pressure is a predictor of mortality in cardiac surgery independently of left ventricular ejection fraction. Br J Anaesth. 2006;97(3):292-297. PMID: 16835254. https://doi.org/10.1093/bja/ael140
- Sastry P., Theologou T., Field M., Shaw M., Pullan D.M., Fabri B.M. Predictive accuracy of EuroSCORE: is end-diastolic dysfunction a missing variable? Eur J Cardiothorac Surg. 2010;37(2):261-266. PMID: 19773181. https://doi.org/10.1016/j.ejcts.2009.05.059
- Merello L., Riesle E., Alburquerque J., Torres H., Aránguiz-Santander E., Pedemonte O., Westerberg B. Risk scores do not predict high mortality after coronary artery bypass surgery in the presence of diastolic dysfunction. Ann Thorac Surg. 2008;85(4):1247-1255. PMID: 18355505. https://doi.org/10.1016/j.athoracsur.2007.12.068
- Thygesen K., Alpert J.S., Jaffe A.S., Chaitman B.R., Bax J.J., Morrow D.A., White H.D.; Executive Group on behalf of the Joint European Society of Cardiology (ESC)/American College of Cardiology (ACC)/American Heart Association (AHA)/World Heart Federation (WHF) Task Force for the Universal Definition of Myocardial Infarction. Fourth universal definition of myocardial infarction (2018). J Am Coll Cardiol. 2018;72(18):2231-2264. PMID: 30153967. https://doi.org/10.1016/j.jacc.2018.08.1038
- Мерекин Д.Н., Ломиворотов В.В., Ефремов С.М., Киров М.Ю., Ломиворотов В.Н. Синдром низкого сердечного выброса в кардиохирургии. Альманах клинической медицины. 2019;47(3):276-297. https://doi.org/10.18786/2072-0505-2019-47-035 Merekin D.N., Lomivorotov V.V., Efremov S.M., Kirov M.Yu., Lomivorotov V.N. Low cardiac output syndrome in cardiac surgery. Almanac of Clinical Medicine. 2019;47(3):276-297. (In Russ.) https://doi.org/10.18786/2072-0505-2019-47-035
- Shah A.M., Claggett B., Sweitzer N.K., Shah S.J., Deswal A., Anand I.S., Fleg J.L., Pitt B., Pfeffer M.A., Solomon S.D. Prognostic importance of changes in cardiac structure and function in heart failure with preserved ejection fraction and the impact of spironolactone. Circ Heart Fail. 2015;8(6):1052-1058. PMID: 26475142; PMCID: PMC4936912. https://doi.org/10.1161/CIRCHEARTFAILURE.115.002249

