Long-term normothermic autoperfusion of the cardiopulmonary complex ex vivo as a method of effective graft conditioning: an experimental study
Published 2023-12-26
Keywords
- Bretschneider Cardioplegic Solution,
- Isolated Heart Preparation,
- Heart Transplantation,
- Perfusion,
- Reperfusion
- Swine,
- Tissue Donors ...More
How to Cite
Copyright (c) 2023 Zhulkov M.O., Tarkova A.R., Zykov I.S., Makaev A.G., Protopopov A.V., Murtazaliev M.N., Kosimov F.Yu., Karmadonova N.A., Smirnov Ya.M., Kliver E.E., Volkov A.M., Agaeva H.A., Sirota D.A.

This work is licensed under a Creative Commons Attribution 4.0 International License.
Abstract
Objective: To compare the effectiveness of 6-hour normothermic autoperfusion of a heart graft ex vivo with pharmaco-cold preservation using Bretschneider's solution (Custodiol, Dr Franz Köhler Chemie GmbH, Bensheim, Germany).
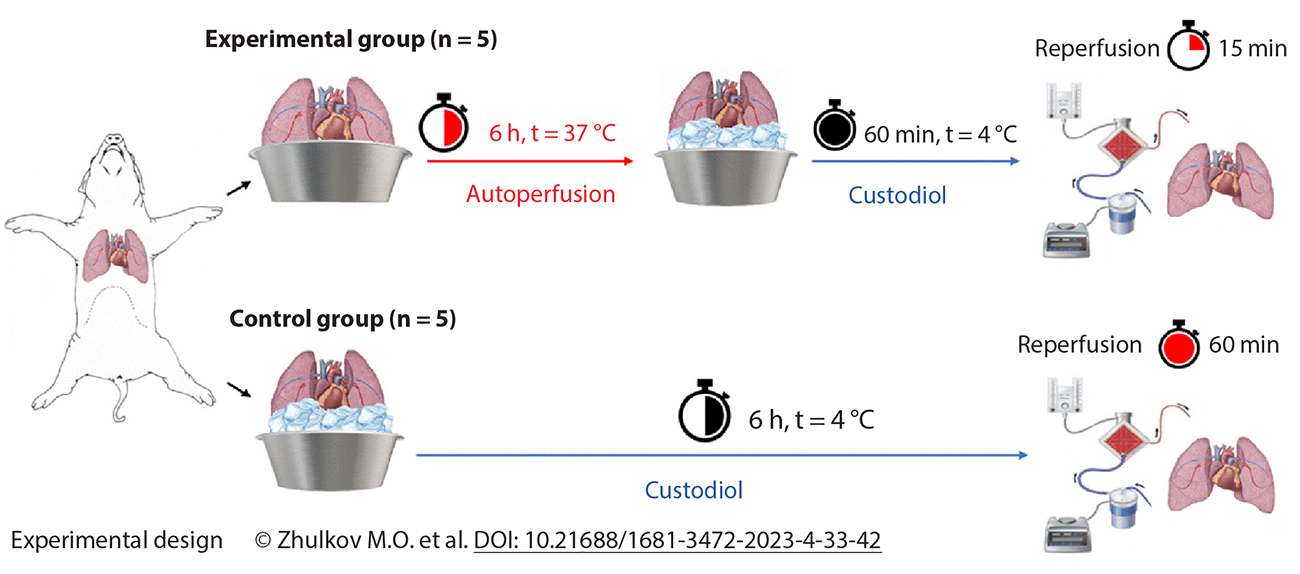
Methods: Landrace pigs weighing 50 ± 5 kg and aged 4–5 months (n = 10) were selected as a model for a series of acute experiments. Cardiopulmonary conditioning using autoperfusion was conducted for 6 hours on the experimental group (n = 5). On the other hand, the control group underwent a 6-hour pharmaco-cold preservation with Bretschneider solution to recover the heart's pumping function. Graft preservation effectiveness was evaluated by measuring hemodynamic parameters, heartbeat, and myocardial ischemia marker concentrations.
Results: After reperfusion and isolation of the working cardiopulmonary complex, cardiac output was 0.63 [0.37; 0.8] L/min and 0.37 [0.23; 0.37] L/min in the experimental and control groups, respectively (P < .05). The levels of CPK-MB, LDH, troponin-I, and lactate in the coronary sinus blood was significantly higher in the control group.
Conclusion: The study demonstrated significant benefits of normothermic autoperfusion in maintaining the morphofunctional status of the donor heart compared to pharmaco-cold preservation using Bretschneider's solution for 6 hours of ex vivo graft conditioning.
Received 16 July 2023. Revised 8 September 2023. Accepted 11 September 2023.
Funding: The study was carried out within the framework of project No. 23-25-10013 (agreement No. 23-25-10013 dated April 20, 2023 with the Russian Science Foundation, agreement No. р-52 dated April 3, 2023 with the Ministry of Science and Innovation Policy of the Novosibirsk Region).
Conflict of interest: The authors declare no conflict of interest.
Contribution of the authors
Conception and study design: M.O. Zhulkov, D.A. Sirota, I.S. Zykov
Data collection and analysis: M.O. Zhulkov, A.R. Tarkova, I.S. Zykov, A.G. Makaev, A.V. Protopopov, M.N. Murtazaliev, F.Yu. Kosimov, N.A. Karmadonova, Ya.M. Smirnov, E.E. Kliver, A.M. Volkov, H.A. Agaeva, D.A. Sirota
Statistical analysis: M.O. Zhulkov
Drafting the article: M.O. Zhulkov
Critical revision of the article: M.O. Zhulkov, D.A. Sirota, I.S. Zykov
Final approval of the version to be published: M.O. Zhulkov, A.R. Tarkova, I.S. Zykov, A.G. Makaev, A.V. Protopopov, M.N. Murtazaliev, F.Yu. Kosimov, N.A. Karmadonova, Ya.M. Smirnov, E.E. Kliver, A.M. Volkov, H.A. Agaeva, D.A. Sirota
References
- Colvin M., Smith J.M., Hadley N., Skeans M.A., Uccellini K., Goff R., Foutz J., Israni A.K., Snyder J.J., Kasiske B.L. OPTN/SRTR 2018 Annual data report: Heart. Am J Transplant. 2020;20 Suppl s1:340-426. PMID: 31898418. https://doi.org/10.1111/ajt.15676
- Kim W.R., Lake J.R., Smith J.M., Schladt D.P., Skeans M.A., Harper A.M., Wainright J.L., Snyder J.J., Israni A.K., Kasiske B.L. OPTN/SRTR 2016 Annual data report: Liver. Am J Transplant. 2018;18 Suppl 1:172-253. PMID: 29292603. https://doi.org/10.1111/ajt.14559
- Hart A., Smith J.M., Skeans M.A., Gustafson S.K., Wilk A.R., Robinson A., Wainright J.L., Haynes C.R., Snyder J.J., Kasiske B.L., Israni A.K. OPTN/SRTR 2016 Annual data report: Kidney. Am J Transplant. 2018;18 Suppl 1(Suppl 1):18-113. PMID: 29292608; PMCID: PMC5772947. https://doi.org/10.1111/ajt.14557
- Жульков М.О., Зыков И.С., Сирота Д.А., Агаева Х.А., Сабетов А.К., Повещенко О.В., Бозоров С.Ш., Фомичев А.В., Чернявский А.М. Способ длительного кондиционирования донорского сердца методом аутоперфузии. Вестник экспериментальной и клинической хирургии. 2022;15(3):214-220. https://doi.org/10.18499/2070-478X-2022-15-3-214-220 Zhulkov M.O., Zykov I.S., Sirota D.А., Agaeva H.A., Sabetov A.K., Poveschenko O.V., Bozorov S.Sh., Fomichev A.V., Chernyavsky A.M. Long-term conditioning of a donor heart by autoperfusion. Journal of Experimental and Clinical Surgery. 2022;15(3):214-220. (In Russ.) https://doi.org/10.18499/2070-478X-2022-15-3-214-220
- Barnard C.N. The operation. A human cardiac transplant: an interim report of a successful operation performed at Groote Schuur Hospital, Cape Town. S Afr Med J. 1967;41(48):1271-1274. PMID: 4170370.
- Guibert E.E., Petrenko A.Y., Balaban C.L., Somov A.Y., Rodriguez J.V., Fuller B.J. Organ preservation: current concepts and new strategies for the next decade. Transfus Med Hemother. 2011;38(2):125-142. PMID: 21566713; PMCID: PMC3088735. https://doi.org/10.1159/000327033
- Mehta V., Taylor M., Hasan J., Dimarakis I., Barnard J., Callan P., Shaw S., Venkateswaran R.V. Establishing a heart transplant programme using donation after circulatory-determined death donors: a United Kingdom based single-centre experience. Interact Cardiovasc Thorac Surg. 2019;29(3):422-429. PMID: 31098641. https://doi.org/10.1093/icvts/ivz121
- Фомичев А.В., Хван Д.С., Агаева Х.А., Жульков М.О., Доронин Д.В., Чернявский А.М. Опыт использования донорского сердца с продленной холодовой ишемией. Российский кардиологический журнал. 2020;25(8):4011. https://doi.org/10.15829/1560-4071-2020-4011 Fomichev A.V., Khvan D.S., Agaeva H.A., Zhulkov M.O., Doronin D.V., Chernyavsky A.M. Experience of heart transplantation with an extended cold ischemic time of donor heart. Russian Journal of Cardiology. 2020;25(8):4011. (In Russ.) https://doi.org/10.15829/1560-4071-2020-4011
- Ravikumar R., Leuvenink H., Friend P.J. Normothermic liver preservation: a new paradigm? Transpl Int. 2015;28(6):690-699. PMID: 25847684. https://doi.org/10.1111/tri.12576
- Messer S., Ardehali A., Tsui S. Normothermic donor heart perfusion: current clinical experience and the future. Transpl Int. 2015;28(6):634-642. PMID: 24853906. https://doi.org/10.1111/tri.12361
- Chang D.D., Han J.J. The TransMedics Organ Care System for the liver receives FDA pre-market approval. Artif Organs. 2022;46(1):25-26. PMID: 34802155. https://doi.org/10.1111/aor.14115
- Демихов В.П. Пересадка жизненно важных органов в эксперименте: опыты по пересадке сердца, легких, головы, почек и других органов. М.: Медгиз, 1960. 259 с. Demikhov V.P. Transplantation of vital organs in an experiment: Experiments on transplantation of the heart, lungs, head, kidneys and other organs. Moscow: Medgiz Publ.; 1960. 259 p. (In Russ.)
- Zych B., Popov A.F., Stavri G., Bashford A., Bahrami T., Amrani M., De Robertis F., Carby M., Marczin N., Simon A.R., Redmond K.C. Early outcomes of bilateral sequential single lung transplantation after ex-vivo lung evaluation and reconditioning. J Heart Lung Transplant. 2012;31(3):274-281. PMID: 22088786. https://doi.org/10.1016/j.healun.2011.10.008
- Iyer A., Gao L., Doyle A., Rao P., Cropper J.R., Soto C., Dinale A., Kumarasinghe G., Jabbour A., Hicks M., Jansz P.C., Feneley M.P., Harvey R.P., Graham R.M., Dhital K.K., MacDonald P.S. Normothermic ex vivo perfusion provides superior organ preservation and enables viability assessment of hearts from DCD donors. Am J Transplant. 2015;15(2):371-380. PMID: 25612491. https://doi.org/10.1111/ajt.12994
- Vogel T., Brockmann J.G., Quaglia A., Morovat A., Jassem W., Heaton N.D., Coussios C.C., Friend P.J. The 24-hour normothermic machine perfusion of discarded human liver grafts. Liver Transpl. 2017;23(2):207-220. PMID: 27809409. https://doi.org/10.1002/lt.24672
- Angelico R., Perera M.T.P.R., Ravikumar R., Holroyd D., Coussios C., Mergental H., Isaac J.R., Iqbal A., Cilliers H., Muiesan P., Friend P.J., Mirza D.F. Normothermic machine perfusion of deceased donor liver grafts is associated with improved postreperfusion hemodynamics. Transplant Direct. 2016;2(9):e97. PMID: 27795989; PMCID: PMC5068202. https://doi.org/10.1097/TXD.0000000000000611
- Wallinder A., Ricksten S.-E., Hansson C., Riise G.C., Silverborn M., Liden H., Olausson M., Dellgren G. Transplantation of initially rejected donor lungs after ex vivo lung perfusion. J Thorac Cardiovasc Surg. 2012;144(5):1222-1228. PMID: 22995721. https://doi.org/10.1016/j.jtcvs.2012.08.011
- Jamieson R.W., Zilvetti M., Roy D., Hughes D., Morovat A., Coussios C.C., Friend P.J. Hepatic steatosis and normothermic perfusion-preliminary experiments in a porcine model. Transplantation. 2011;92(3):289-295. PMID: 21681143. https://doi.org/10.1097/TP.0b013e318223d817
- Pettit S.J., Petrie M.C. Transplantation of hearts donated after circulatory-determined death. Circ Heart Fail. 2019;12(4):e005991. PMID: 30998399. https://doi.org/10.1161/CIRCHEARTFAILURE.119.005991
- Hardesty R.L., Griffith B.P. Autoperfusion of the heart and lungs for preservation during distant procurement. J Thorac Cardiovasc Surg. 1987;93(1):11-18. PMID: 3540455.
- Starling E.H., Visscher M.B. The regulation of the energy output of the heart. J Physiol. 1927;62(3):243-261. PMID: 16993846; PMCID: PMC1514842. https://doi.org/10.1113/jphysiol.1927.sp002355
- Robicsek F., Pruitt J.R., Sanger P.W., Daugherty H.K., Moore M., Bagby E. The maintenance of function of the donor heart in the extracorporeal stage and during transplantation. Ann Thorac Surg. 1968;6(4):330-342. PMID: 4913322. https://doi.org/10.1016/s0003-4975(10)66033-x
- Morimoto T., Golding L.R., Stewart R.W., Harasaki H., Matsushita S., Shimomitsu T., Kasick J., Olsen E., Loop F.D., Nose Y. A simple method for extended heart-lung preservation by autoperfusion. Trans Am Soc Artif Intern Organs. 1984;30:320-324. PMID: 6442806.
- Banner N.R., Thomas H.L., Curnow E., Hussey J.C., Rogers C.A., Bonser R.S.; Steering Group of the United Kingdom Cardiothoracic Transplant Audit. The importance of cold and warm cardiac ischemia for survival after heart transplantation. Transplantation. 2008;86(4):542-547. PMID: 18724223. https://doi.org/10.1097/TP.0b013e31818149b9
- Van Raemdonck D., Rega F., Rex S., Neyrinck A. Machine perfusion of thoracic organs. J Thorac Dis. 2018;10(Suppl 8):S910-S923. PMID: 29744218; PMCID: PMC5934115. https://doi.org/10.21037/jtd.2018.02.85
- King R.C., Binns O.A., Rodriguez F., Kanithanon R.C., Daniel T.M., Spotnitz W.D., Tribble C.G., Kron I.L. Reperfusion injury significantly impacts clinical outcome after pulmonary transplantation. Ann Thorac Surg. 2000;69(6):1681-1685. PMID: 10892906. https://doi.org/10.1016/s0003-4975(00)01425-9
- Monteagudo Vela M., García Sáez D., Simon A.R. Current approaches in retrieval and heart preservation. Ann Cardiothorac Surg. 2018;7(1):67-74. PMID: 29492384; PMCID: PMC5827116. https://doi.org/10.21037/acs.2018.01.06
- Ploeg R.J., D'Alessandro A.M., Hoffmann R.M., Eckhoff D., Isaacs R., Knechtle S.J., Pirsch J.D., Stegall M.D., Kalayoglu M., Belzer F.O. Impact of donor factors and preservation on function and survival after liver transplantation. Transplant Proc. 1993;25(6):3031-3033. PMID: 8266441.
- Pinnelas R., Kobashigawa J.A. Ex vivo normothermic perfusion in heart transplantation: a review of the TransMedics Organ Care System. Future Cardiol. 2022;18(1):5-15. PMID: 34503344. https://doi.org/10.2217/fca-2021-0030
- Macdonald P.S., Chew H.C., Connellan M., Dhital K. Extracorporeal heart perfusion before heart transplantation: the heart in a box. Curr Opin Organ Transplant. 2016;21(3):336-342. PMID: 26967996. https://doi.org/10.1097/MOT.0000000000000309
- Hassanein W.H., Zellos L., Tyrrell T.A., Healey N.A., Crittenden M.D., Birjiniuk V., Khuri S.F. Continuous perfusion of donor hearts in the beating state extends preservation time and improves recovery of function. J Thorac Cardiovasc Surg. 1998;116(5):821-830. PMID: 9806389. https://doi.org/10.1016/S0022-5223(98)00452-8
- Makdisi G., Makdisi T., Jarmi T., Caldeira C.C. Ex vivo lung perfusion review of a revolutionary technology. Ann Transl Med. 2017;5(17):343. PMID: 28936437; PMCID: PMC5599284. https://doi.org/10.21037/atm.2017.07.17
- Ceresa C.D.L., Nasralla D., Jassem W. Normothermic machine preservation of the liver: state of the art. Curr Transplant Rep. 2018;5(1):104-110. PMID: 29564207; PMCID: PMC5843699. https://doi.org/10.1007/s40472-018-0186-9
- Kaliyev R., Bekbossynov S., Nurmykhametova Z. Sixteen-hour ex vivo donor heart perfusion during long-distance transportation for heart transplantation. Artif Organs. 2019;43(3):319-320. PMID: 30585343; PMCID: PMC6590649. https://doi.org/10.1111/aor.13359
- Tatum R., O'Malley T.J., Bodzin A.S., Tchantchaleishvili V. Machine perfusion of donor organs for transplantation. Artif Organs. 2021;45(7):682-695. PMID: 33349946. https://doi.org/10.1111/aor.13894
- Chien S., Diana J.N., Oeltgen P.R., Todd E.P., O'Connor W.N., Chitwood W.R. Jr. Eighteen to 37 hours' preservation of major organs using a new autoperfusion multiorgan preparation. Ann Thorac Surg. 1989;47(6):860-867. PMID: 2757441. https://doi.org/10.1016/0003-4975(89)90021-0
- Chien S.F., Diana J.N., Oeltgen P.R., Salley R. Functional studies of the heart during a 24-hour preservation using a new autoperfusion preparation. J Heart Lung Transplant. 1991;10(3):401-408. PMID: 1854768.
- Chien S., Diana J.N., Todd E.P., O'Connor W.N., Marion T., Smith K. New autoperfusion preparation for long-term organ preservation. Circulation. 1988;78(5 Pt 2):III58-III65. PMID: 3180407.
- Riveron F.A., Ross J.H., Schwartz K.A., Casey G., Sanders O., Eisiminger R., Magilligan D.J. Jr. Energy expenditure of autoperfusing heart-lung preparation. Circulation. 1988;78(5 Pt 2):III103-III109. PMID: 3180388.
- Robicsek F., Masters T.N., Duncan G.D., Denyer M.H., Rise H.E., Etchison M. An autoperfused heart-lung-preparation: metabolism and function. J Heart Transplant. 1985;4(3):334-338. PMID: 3916505.

