Tissue inhibitor of metalloproteinase-2 in patients aged 1 month to 1 year with and without cardiac surgery-associated acute kidney injury in congenital heart disease surgery with cardiopulmonary bypass: a single-center retrospective study
Published 2023-12-26
Keywords
- Acute Kidney Injury,
- Cardiac Surgical Procedures,
- Cardiopulmonary Bypass,
- Child,
- Heart Defects, Congenital
- Retrospective Studies,
- Tissue Inhibitor of Metalloproteinase-2 ...More
How to Cite
Copyright (c) 2023 Sergeev S.A., Lomivorotov V.V., Lomivorotov V.N., Nepomniashchikh V.A.

This work is licensed under a Creative Commons Attribution 4.0 International License.
Abstract
Introduction: Acute kidney injury is a common complication of cardiac surgery after management of congenital heart defects. Cardiac surgery-associated acute kidney injury (CS-AKI) results in longer stays of patients in the intensive care unit and hospital. However, using an increase in postoperative creatinine as a means of detecting AKI has some limitations, since significant changes occur after the loss of more than 50% of renal function. In children, the creatinine level is influenced by various factors such as muscle mass, cardiac output, etc. These factors vary significantly among young children and complicate the early diagnosis of AKI. Recent studies have explored biomarkers as potential predictors for the early detection of CS-AKI after cardiac surgery for management of congenital heart disease in children.
Objective: To evaluate the urinary tissue inhibitor of metalloproteinase-2 (TIMP2) as a predictor of CS-AKI following management of congenital heart defects in children aged 1 month to 1 year who underwent cardiopulmonary bypass.
Methods: A single-center retrospective study included patients aged 1 month to 1 year who underwent cardiopulmonary bypass for the correction of congenital heart defects. The groups were formed based on the presence of CS-AKI. The study group comprised of patients who had CS-AKI (group 1, n = 52), while those without CC-AKI constituted the control group (group 2, n = 98). To ensure minimal systematic errors and comparability between two groups, propensity score matching analysis was performed (52 patients in groups 1 and 2). Preoperative, intraoperative, and postoperative parameters and characteristics were compared.
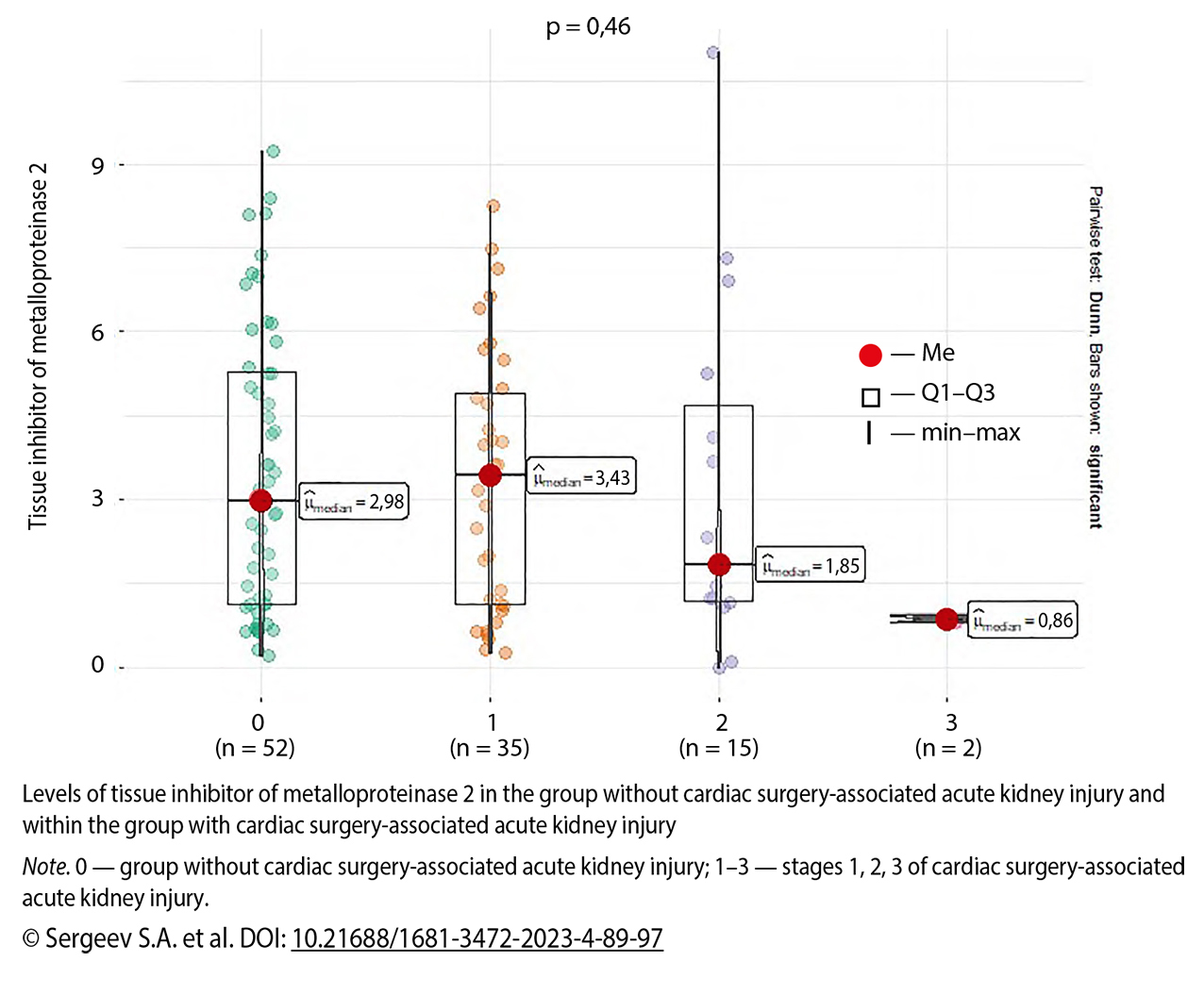
Results: The results showed no differences in baseline or demographic characteristics between the patients. In the study group, 34.6% of patients were diagnosed with CS-AKI. Among them, 67.4% (n = 35) were stage 1, 28.8% (n = 15) were stage 2, and 3.8% (n = 2) were stage 3. The results of the regression analysis show a decrease by 24% and an increase by 9 and 16% in CS-AKI respectively, with an increase in creatinine levels by 1 µmol/l, at baseline and on days 3 and 4. Additionally, male patients have a 76% lower likelihood to develop CS-AKI. It was observed that there was no significant difference in the tissue inhibitor of metalloprotease-2 levels between the groups with and without CS-AKI.
Conclusion: Urinary TIMP2 levels were found to be unable to predict the early onset of CS-AKI in congenital heart defect patients ages 1 month to 1 year who underwent cardiopulmonary bypass surgery.
Received 24 April 2023. Revised 27 November 2023. Accepted 28 November 2023.
Funding: The study did not have sponsorship.
Conflict of interest: The authors declare no conflict of interest.
Contribution of the authors: The authors contributed equally to this article.
References
- Krawczeski C.D., Woo J.G., Wang Y., Bennett M.R., Ma Q., Devarajan P. Neutrophil gelatinase-associated lipocalin concentrations predict development of acute kidney injury in neonates and children after cardiopulmonary bypass. J Pediatr. 2011;158(6):1009-1155.e1. PMID: 21300375. https://doi.org/10.1016/j.jpeds.2010.12.057
- Parikh C.R., Devarajan P., Zappitelli M., Sint K., Thiessen-Philbrook H., Li S., Kim R.W., Koyner J.L., Coca S.G., Edelstein C.L., Shlipak M.G., Garg A.X., Krawczeski C.D.; TRIBE-AKI Consortium. Postoperative biomarkers predict acute kidney injury and poor outcomes after pediatric cardiac surgery. J Am Soc Nephrol. 2011;22(9):1737-1747. PMID: 21836147; PMCID: PMC3171944. https://doi.org/10.1681/ASN.2010111163
- Mehta R.H., Grab J.D., O’Brien S.M., Bridges C.R., Gammie J.S., Haan C.K., Ferguson T.B., Peterson E.D.; Society of Thoracic Surgeons National Cardiac Surgery Database Investigators. Bedside tool for predicting the risk of postoperative dialysis in patients undergoing cardiac surgery. Circulation. 2006;114(21):2208-2216. PMID: 17088458. https://doi.org/10.1161/CIRCULATIONAHA.106.635573
- Rahmanian P.B., Filsoufi F., Castillo J.G., Zaku B., Chikwe J., Carpentier A., Adams D.H. Predicting postoperative renal failure requiring dialysis, and an analysis of long-term outcome in patients undergoing valve surgery. J Heart Valve Dis. 2008;17(6):657-665. PMID: 19137798.
- Waldherr S., Fichtner A., Beedgen B., Bruckner T., Schaefer F., Tönshoff B., Pöschl J., Westhoff T.H., Westhoff J.H. Urinary acute kidney injury biomarkers in very low-birth-weight infants on indomethacin for patent ductus arteriosus. Pediatr Res. 2019;85(5):678-686. PMID: 30745571. https://doi.org/10.1038/s41390-019-0332-9
- Hanna M., Brophy P.D., Giannone P.J., Joshi M.S., Bauer J.A., RamachandraRao S. Early urinary biomarkers of acute kidney injury in preterm infants. Pediatr Res. 2016;80(2):218-223. PMID: 27055185. https://doi.org/10.1038/pr.2016.70
- Ostermann M., McCullough P.A., Forni L.G., Bagshaw S.M., Joannidis M., Shi J., Kashani K., Honore P.M., Chawla L.S., Kellum J.A.; SAPPHIRE Investigators. Kinetics of urinary cell cycle arrest markers for acute kidney injury following exposure to potential renal insults. Crit Care Med. 2018;46(3):375-383. PMID: 29189343; PMCID: PMC5821475. https://doi.org/10.1097/CCM.0000000000002847
- Meersch M., Schmidt C., Van Aken H., Rossaint J., Gorlich D., Stege D., Malec E., Januszewska K., Zarbock A. Validation of cell-cycle arrest biomarkers for acute kidney injury after pediatric cardiac surgery. PLoS One. 2014;9(10):e110865. PMID: 25343505; PMCID: PMC4208780. https://doi.org/10.1371/journal.pone.0110865
- Kashani K., Al-Khafaji A., Ardiles T., Artigas A., Bagshaw S.M., Bell M., Bihorac A., Birkhahn R., Cely C.M., Chawla L.S., Davison D.L., Feldkamp T., Forni L.G., Gong M.N., Gunnerson K.J., Haase M., Hackett J., Honore P.M., Hoste E.A.J., Joannes-Boyau O., Joannidis M., Kim P., Koyner J.L., Laskowitz D.T., Lissauer M.E., Marx G., McCullough P.A., Mullaney S., Ostermann M., Rimmelé T., Shapiro N.I., Shaw A.D., Shi J., Sprague A.M., Vincent J.-L., Vinsonneau C., Wagner L., Walker M.G., Wilkerson R.G., Zacharowski K., Kellum J.A. Discovery and validation of cell cycle arrest biomarkers in human acute kidney injury. Crit Care. 2013;17(1):R25. PMID: 23388612; PMCID: PMC4057242. https://doi.org/10.1186/cc12503
- Hoste E.A., McCullough P.A., Kashani K., Chawla L.S., Joannidis M., Shaw A.D., Feldkamp T., Uettwiller-Geiger D.L., McCarthy P., Shi J., Walker M.G., Kellum J.A.; Sapphire Investigators. Derivation and validation of cutoffs for clinical use of cell cycle arrest biomarkers. Nephrol Dial Transplant. 2014;29(11):2054-2061. PMID: 25237065; PMCID: PMC4209880. https://doi.org/10.1093/ndt/gfu292
- Wetz A.J., Richardt E.M., Wand S., Kunze N., Schotola H., Quintel M., Bräuer A., Moerer O. Quantification of urinary TIMP-2 and IGFBP-7: an adequate diagnostic test to predict acute kidney injury after cardiac surgery? Crit Care. 2015;19(1):3. PMID: 25560277; PMCID: PMC4310039. https://doi.org/10.1186/s13054-014-0717-4
- Vijayan A., Faubel S., Askenazi D.J., Cerda J., Fissell W.H., Heung M., Humphreys B.D., Koyner J.L., Liu K.D., Mour G., Nolin T.D., Bihorac A.; American Society of Nephrology Acute Kidney Injury Advisory Group. Clinical use of the urine biomarker [TIMP-2] x [IGFBP7] for acute kidney injury risk assessment. Am J Kidney Dis. 2016;68(1):19-28. PMID: 26948834; PMCID: PMC4921267. https://doi.org/10.1053/j.ajkd.2015.12.033
- Yamashita T., Doi K., Hamasaki Y., Matsubara T., Ishii T., Yahagi N., Nangaku M., Noiri E. Evaluation of urinary tissue inhibitor of metalloproteinase-2 in acute kidney injury: a prospective observational study. Crit Care. 2014;18(6):716. PMID: 25524453; PMCID: PMC4300076. https://doi.org/10.1186/s13054-014-0716-5
- Bai Z., Fang F., Xu Z., Lu C., Wang X., Chen J., Pan J., Wang J., Li Y. Serum and urine FGF23 and IGFBP-7 for the prediction of acute kidney injury in critically ill children. BMC Pediatr. 2018;18(1):192. PMID: 29907141; PMCID: PMC6004091. https://doi.org/10.1186/s12887-018-1175-y
- Kellum J.A., Lameire N., Aspelin P., Barsoum R.S., Burdmann E.A., Goldstein S.L., Herzog C.A., Joannidis M., Kribben A., Levey A.S., MacLeod A.M., Mehta R.L., Murray P.T., Naicker S., Opal S.M., Schaefer F., Schetz M., Uchino S.; Kidney disease: Improving global outcomes (KDIGO) acute kidney injury work group. KDIGO clinical practice guideline for acute kidney injury. Kidney Int Suppl. 2012;2(1):1-138. https://doi.org/10.1038/kisup.2012.1
- Gaies M.G., Gurney J.G., Yen A.H., Napoli M.L., Gajarski R.J., Ohye R.G., Charpie J.R., Hirsch J.C. Vasoactive-inotropic score as a predictor of morbidity and mortality in infants after cardiopulmonary bypass. Pediatr Crit Care Med. 2010;11(2):234-238. PMID: 19794327. https://doi.org/10.1097/PCC.0b013e3181b806fc
- Jenkins K.J., Gauvreau K. Center-specific differences in mortality: preliminary analyses using the Risk Adjustment in Congenital Heart Surgery (RACHS-1) method. J Thorac Cardiovasc Surg. 2002;124(1):97-104. PMID: 12091814. https://doi.org/10.1067/mtc.2002.122311
- Tóth R., Breuer T., Cserép Z., Lex D., Fazekas L., Sápi E., Szatmári A., Gál J., Székely A. Acute kidney injury is associated with higher morbidity and resource utilization in pediatric patients undergoing heart surgery. Ann Thorac Surg. 2012;93(6):1984-1990. PMID: 22226235. https://doi.org/10.1016/j.athoracsur.2011.10.046
- Taylor M.L., Carmona F., Thiagarajan R.R., Westgate L., Ferguson M.A., del Nido P.J., Rajagopal S.K. Mild postoperative acute kidney injury and outcomes after surgery for congenital heart disease. J Thorac Cardiovasc Surg. 2013;146(1):146-152. PMID: 23040323. https://doi.org/10.1016/j.jtcvs.2012.09.008
- Selewski D.T., Cornell T.T., Heung M., Troost J.P., Ehrmann B.J., Lombel R.M., Blatt N.B., Luckritz K., Hieber S., Gajarski R., Kershaw D.B., Shanley T.P., Gipson D.S. Validation of the KDIGO acute kidney injury criteria in a pediatric critical care population. Intensive Care Med. 2014;40(10):1481-1488. PMID: 25079008. https://doi.org/10.1007/s00134-014-3391-8
- Zappitelli M., Moffett B.S., Hyder A., Goldstein S.L. Acute kidney injury in noncritically ill children treated with aminoglycoside antibiotics in a tertiary healthcare centre: a retrospective cohort study. Nephrol Dial Transplant. 2011;26(1):144-150. PMID: 20591815. https://doi.org/10.1093/ndt/gfq375
- Rheault M.N., Zhang L., Selewski D.T., Kallash M., Tran C.L., Seamon M., Katsoufis C., Ashoor I., Hernandez J., Supe-Markovina K., D'Alessandri-Silva C., DeJesus-Gonzalez N., Vasylyeva T.L., Formeck C., Woll C., Gbadegesin R., Geier P., Devarajan P., Carpenter S.L., Kerlin B.A., Smoyer W.E.; Midwest Pediatric Nephrology Consortium. AKI in children hospitalized with nephrotic syndrome. Clin J Am Soc Nephrol. 2015;10(12):2110-2118. PMID: 26450933; PMCID: PMC4670770. https://doi.org/10.2215/CJN.06620615
- Bell M., Larsson A., Venge P., Bellomo R., Martensson J. Assessment of cell-cycle arrest biomarkers to predict early and delayed acute kidney injury. Dis Markers. 2015;2015:158658. PMID: 25866432; PMCID: PMC4381987. https://doi.org/10.1155/2015/158658
- Bihorac A., Chawla L.S., Shaw A.D., Al-Khafaji A., Davison D.L., Demuth G.E., Fitzgerald R., Gong M.N., Graham D.D., Gunnerson K., Heung M., Jortani S., Kleerup E., Koyner J.L., Krell K., Letourneau J., Lissauer M., Miner J., Nguyen H.B., Ortega L.M., Self W.H., Sellman R., Shi J., Straseski J., Szalados J.E., Wilber S.T., Walker M.G., Wilson J., Wunderink R., Zimmerman J., Kellum J.A. Validation of cell-cycle arrest biomarkers for acute kidney injury using clinical adjudication. Am J Respir Crit Care Med. 2014;189(8):932-939. PMID: 24559465. https://doi.org/10.1164/rccm.201401-0077OC
- Lameire N., Vanmassenhove J., Van Biesen W., Vanholder R. The cell cycle biomarkers: promising research, but do not oversell them. Clin Kidney J. 2016;9(3):353-358. PMID: 27274818; PMCID: PMC4886923. https://doi.org/10.1093/ckj/sfw033
- Selewski D.T., Charlton J.R., Jetton J.G., Guillet R., Mhanna M.J., Askenazi D.J., Kent A.L. Neonatal acute kidney injury. Pediatrics. 2015;136(2):e463-e473. PMID: 26169430. https://doi.org/10.1542/peds.2014-3819
- Perico N., Askenazi D., Cortinovis M., Remuzzi G. Maternal and environmental risk factors for neonatal AKI and its long-term consequences. Nat Rev Nephrol. 2018;14(11):688-703. PMID: 30224767. https://doi.org/10.1038/s41581-018-0054-y
- Chen J., Sun Y., Wang S., Dai X., Huang H., Bai Z., Li X., Wang J., Li Y. The effectiveness of urinary TIMP-2 and IGFBP-7 in predicting acute kidney injury in critically ill neonates. Pediatr Res. 2020;87(6):1052-1059. PMID: 31791043. https://doi.org/10.1038/s41390-019-0698-8

