Immediate outcomes of transcatheter aortic valve implantation in patients with horizontal aorta
Published 2023-06-30
Keywords
- Aorta,
- Aortic Valve Insufficiency,
- Aortic Valve Stenosis,
- Bioprosthesis,
- Myocardium
- Retrospective Studies,
- Transcatheter Aortic Valve Replacement ...More
How to Cite
Copyright (c) 2023 Baranov A.A., Krestyaninov O.V., Badoian A.G., Khelimskii D.A., Manukian S.N., Tsydenova A.Yu., Makhmudov M.A.

This work is licensed under a Creative Commons Attribution 4.0 International License.
Abstract
Background: Transcatheter aortic valve implantation (TAVI) is an effective and safe procedure for severe aortic stenosis. Increased aortic root angulation is an important anatomical feature that may cause technical difficulties and negatively affect immediate and long-term outcomes.
Objective: To evaluate immediate outcomes of TAVI in patients with increased aortic root angulation.
Methods: Our retrospective single-center study included 412 patients with severe aortic stenosis who underwent TAVI using self-expanding bioprostheses from 2015 to 2022. Patients with aortic root angulation ≥ 49° were included in group 1 (n = 200), and those with aortic root angulation < 49° comprised group 2 (n = 212).
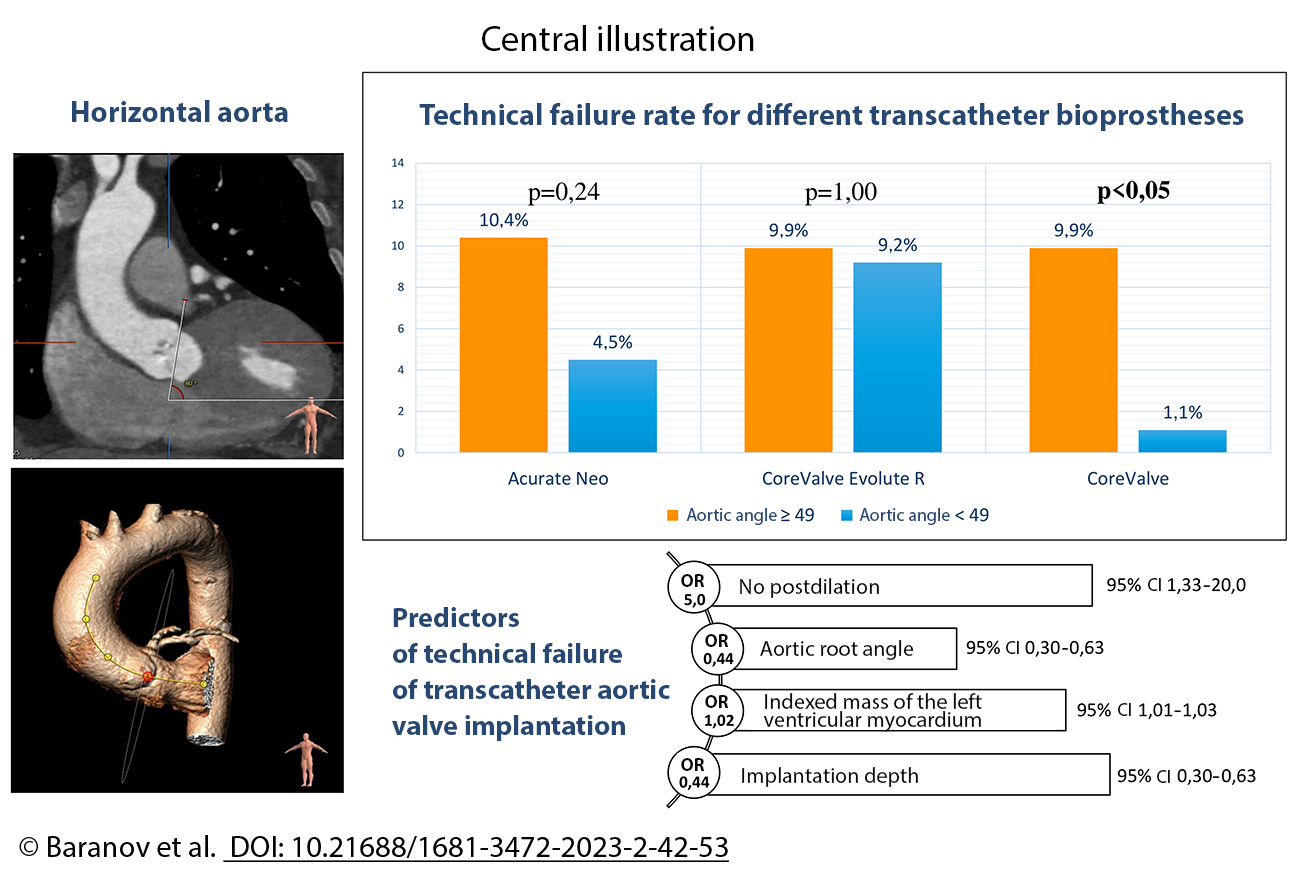
Results: The mean age of the patients was 75.2 ± 7.2 years. In a subgroup with the first-generation CoreValve prosthesis and a ≥ 49° angle, we observed moderate aortic regurgitation significantly more often (7.4% vs 0.0%, P = .010) and technical success significantly less often (90.1% vs 98.9%, P = .010) compared with a similar subgroup with a < 49° angle. In subgroups with CoreValve Evolute R and ACURATE neo prostheses, there were no significant differences in terms of the mentioned parameters. Independent predictors of technical failure were the aortic root angle [OR for each degree increase: 0.44, 95% CI: 0.30-0.63, P < .001], no postdilation [OR: 5.0, 95% CI: 1.33-20.00, P = .074], indexed mass of the left ventricular myocardium [OR: 1.02, 95% CI: 1.01-1.03, P = .003], and higher implantation relative to the aortic annulus [OR for every 1 mm decrease in implantation depth: 0.44, 95% CI: 0.30-0.63, P < .001].
Conclusion: Increased aortic angulation ≥ 49° negatively affected the technical success of TAVI only in patients with the first-generation CoreValve prostheses. Independent predictors of technical failure in TAVI were the aortic root angle, no postdilation, indexed mass of the left ventricular myocardium, and higher implantation relative to the aortic annulus.
Received 9 January 2023. Revised 10 May 2023. Accepted 30 May 2023.
Funding: The study did not have sponsorship.
Conflict of interest: The authors declare no conflict of interest.
Contribution of the authors
Conception and study design: A.A. Baranov, O.V. Krestyaninov, D.A. Khelimskii, A.G. Badoian
Data collection and analysis: A.A. Baranov, O.V. Krestyaninov, D.A. Khelimskii, A.G. Badoian
Statistical analysis: A.A. Baranov, O.V. Krestyaninov, D.A. Khelimskii, A.G. Badoian
Drafting the article: A.A. Baranov, O.V. Krestyaninov, D.A. Khelimskii, A.G. Badoian, S.N. Manukian, A.Yu. Tsydenova,
M.A. Makhmudov
Critical revision of the article: A.A. Baranov, O.V. Krestyaninov, D.A. Khelimskii, A.G. Badoian, S.N. Manukian, A.Yu. Tsydenova, M.A. Makhmudov
Final approval of the version to be published: A.A. Baranov, O.V. Krestyaninov, D.A. Khelimskii, A.G. Badoian, S.N. Manukian, A.Yu. Tsydenova, M.A. Makhmudov
References
- Makkar R.R., Fontana G.P., Jilaihawi H., Kapadia S., Pichard A.D., Douglas P.S., Thourani V.H., Babaliaros V.C., Webb J.G., Herrmann H.C., Bavaria J.E., Kodali S., Brown D.L., Bowers B., Dewey T.M., Svensson L.G., Tuzcu M., Moses J.W., Williams M.R., Siegel R.J., Akin J.J., Anderson W.N., Pocock S., Smith C.R., Leon M.B.; PARTNER Trial Investigators. Transcatheter aortic-valve replacement for inoperable severe aortic stenosis. N Engl J Med. 2012;366(18):1696-1704. PMID: 22443478. https://doi.org/10.1056/NEJMoa1202277
- Kodali S.K., Williams M.R., Smith C.R., Svensson L.G., Webb J.G., Makkar R.R., Fontana G.P., Dewey T.M., Thourani V.H., Pichard A.D., Fischbein M., Szeto W.Y., Lim S., Greason K.L., Teirstein P.S., Malaisrie S.C., Douglas P.S., Hahn R.T., Whisenant B., Zajarias A., Wang D., Akin J.J., Anderson W.N., Leon M.B.; PARTNER Trial Investigators. Two-year outcomes after transcatheter or surgical aortic-valve replacement. N Engl J Med. 2012;366(18):1686-1695. PMID: 22443479. https://doi.org/10.1056/NEJMoa1200384
- Gallo F., Gallone G., Kim W.-K., Reifart J., Veulemans V., Zeus T., Toggweiler S., De Backer O., Søndergaard L., Mangieri A., Khokhar A., De Marco F., Regazzoli D., Reimers B., Muntané-Carol G., Estévez-Loureiro R., Espino A., Moscarelli M., Armario X., Mylotte D., Gorla R., Bhadra O.D., Conradi L., Donday L.A.M., Nombela-Franco L., Barbanti M., Reddavid C., Criscione E., Brugaletta S., Regueiro A., Pérez-Fuentes P., Nicolini E., Piva T., Tzanis G., Rodes-Cabau J., Colombo A., Giannini F. Horizontal aorta in transcatheter self-expanding valves: insights from the HORSE international multicentre registry. Circ Cardiovasc Interv. 2021;14(9):e010641. https://doi.org/10.1161/CIRCINTERVENTIONS.121.010641
- Zhou D., Chen J., Fan J., Yidilisi A., Dai H., Xu Y., Zhu G., Guo Y., Wang J., Liu X. Self-expanding transcatheter aortic valve replacement in patients with extremely horizontal aortas. Catheter Cardiovasc Interv. 2022;99(Suppl 1):1432-1439. PMID: 35094487. https://doi.org/10.1002/ccd.30094
- Sievers H.-H., Schmidtke C. A classification system for the bicuspid aortic valve from 304 surgical specimens. J Thorac Cardiovasc Surg. 2007;133(5):1226-1233. PMID: 17467434. https://doi.org/10.1016/j.jtcvs.2007.01.039
- Vahanian A., Beyersdorf F., Praz F., Milojevic M., Baldus S., Bauersachs J., Capodanno D., Conradi L., De Bonis M., De Paulis R., Delgado V., Freemantle N., Gilard M., Haugaa K.H., Jeppsson A., Jüni P., Pierard L., Prendergast B.D., Sádaba J.R., Tribouilloy C., Wojakowski W.; ESC/EACTS Scientific Document Group. 2021 ESC/EACTS Guidelines for the management of valvular heart disease. Eur Heart J. 2021;43(7):561-632. PMID: 34453165. https://doi.org/10.1093/eurheartj/ehab395
- Nashef S.A.M., Roques F., Sharples L.D., Nilsson J., Smith C., Goldstone A.R., Lockowandt U. EuroSCORE II. Eur J Cardiothorac Surg. 2012;41(4):734-744. PMID: 22378855. https://doi.org/10.1093/ejcts/ezs043
- Shahian D.M., O’Brien S.M., Filardo G., Ferraris V.A., Haan C.K., Rich J.B., Normand S.-L.T., DeLong E.R., Shewan C.M., Dokholyan R.S., Peterson E.D., Edwards F.H., Anderson R.P.; Society of Thoracic Surgeons Quality Measurement Task Force. The Society of Thoracic Surgeons 2008 cardiac surgery risk models: Part 1 — coronary artery bypass grafting surgery. Ann Thorac Surg. 2009;88(1 Suppl):S2-S22. PMID: 19559822. https://doi.org/10.1016/j.athoracsur.2009.05.053
- Kappetein A.P., Head S.J., Généreux P., Piazza N., van Mieghem N.M., Blackstone E.H., Brott T.G., Cohen D.J., Cutlip D.E., van Es G.-A., Hahn R.T., Kirtane A.J., Krucoff M.W., Kodali S., Mack M.J., Mehran R., Rodés-Cabau J., Vranckx P., Webb J.G., Windecker S., Serruys P.W., Leon M.B. Updated standardized endpoint definitions for transcatheter aortic valve implantation: the Valve Academic Research Consortium-2 consensus document. Eur Heart J. 2012;33(19):2403-2418. PMID: 23026477. https://doi.org/10.1093/eurheartj/ehs255
- Di Stefano D., Colombo A., Mangieri A., Gallone G., Tzanis G., Laricchia A., Baldetti L., Palmisano A., Esposito A., Gallo F., Latib A., Montorfano M., Giannini F. Impact of horizontal aorta on procedural and clinical outcomes in second-generation transcatheter aortic valve implantation. EuroIntervention. 2019;15(9):e749-e756. PMID: 31334701. https://doi.org/10.4244/EIJ-D-19-00455
- Имаев Т.Э., Комлев А.Е., Саличкин Д.В., Лепилин П.М., Колегаев А.С., Терновой С.К., Акчурин Р.С. Транскатетерное протезирование аортального клапана при горизонтально расположенном корне аорты. Кардиологический вестник. 2018;13(1):40‑44. https://doi.org/10.17116/Cardiobulletin201813140-44 Imaev T.E., Komlev A.E., Salichkin D.V., Lepilin P.M., Kolegaev A.S., Ternovoy S.K., Akchurin R.S. Transcateter aortic valve implantation in horisontal aortic root. Kardiologicheskii Vestnik = Russian Cardiology Bulletin. 2018;13(1):40‑44. (In Russ.) https://doi.org/10.17116/Cardiobulletin201813140-44
- Abdel-Wahab M., Kitamura M., Thiele H. TAVI and horizontal aorta: a “no impact” relationship? EuroIntervention. 2019;15(9):e736-e738. PMID: 31579008. https://doi.org/10.4244/EIJV15I9A136
- Lv W., Li S., Liao Y., Zhao Z., Che G., Chen M., Feng Y. The ‘obesity paradox’ does exist in patients undergoing transcatheter aortic valve implantation for aortic stenosis: a systematic review and meta-analysis. Interact Cardiovasc Thorac Surg. 2017;25(4):633-642. PMID: 28962502. https://doi.org/10.1093/icvts/ivx191
- Sharma A., Lavie C.J., Elmariah S., Borer J.S., Sharma S.K., Vemulapalli S., Yerokun B.A., Li Z., Matsouaka R.A., Marmur J.D. Relationship of body mass index with outcomes after transcatheter aortic valve replacement: results from the National Cardiovascular Data-STS/ACC TVT registry. Mayo Clin Proc. 2020;95(1):57-68. PMID: 31902429. https://doi.org/10.1016/j.mayocp.2019.09.027
- Moscarelli M., Gallo F., Gallone G., Kim W.-K., Reifart J., Veulemans V., Zeus T., Toggweiler S., De Backer O., Søndergaard L., Mangieri A., De Marco F., Regazzoli D., Reimers B., Muntané-Carol G., Lauriero R.E., Armario X., Mylotte D., Bhadra O.D., Conradi L., Donday L.A.M., Nombela-Franco L., Barbanti M., Reddavid C., Brugaletta S., Nicolini E., Tzanis G., Rodes-Cabau J., Colombo A., Giannini F. Aortic angle distribution and predictors of horizontal aorta in patients undergoing transcatheter aortic valve replacement. Int J Cardiol. 2021;338:58-62. PMID: 34090956. https://doi.org/10.1016/j.ijcard.2021.05.054
- Gorla R., De Marco F., Garatti A., Bianchi G., Rubbio A.P., Acerbi El., Casenghi M., Spagnolo P., Brambilla N., Testa L., Agnifili M.L., Tusa M., Bedogni F. Impact of aortic angle on transcatheter aortic valve implantation outcome with Evolut-R, Portico, and Acurate-NEO. Catheter Cardiovasc Interv. 2021;97(1):E135-E145. PMID: 32400068. https://doi.org/10.1002/ccd.28957
- Abramowitz Y., Maeno Y., Chakravarty T., Kazuno Y., Takahashi N., Kawamori H., Mangat G., Cheng W., Jilaihawi H., Makkar R.R. Aortic angulation attenuates procedural success following self-expandable but not balloon-expandable TAVR. JACC Cardiovasc Imaging. 2016;9(8):964-972. PMID: 27424244. https://doi.org/10.1016/j.jcmg.2016.02.030
- Sherif M.A., Abdel-Wahab M., Stöcker B., Geist V., Richardt D., Tölg R., Richardt G. Anatomic and procedural predictors of paravalvular aortic regurgitation after implantation of the Medtronic CoreValve bioprosthesis. J Am Coll Cardiol. 2010;56(20):1623-1629. PMID: 21050971. https://doi.org/10.1016/j.jacc.2010.06.035
- Fedak P.W., Verma S., David T.E., Leask R.L., Weisel R.D., Butany J. Clinical and pathophysiological implications of a bicuspid aortic valve. Circulation. 2002;106(8):900-904. PMID: 12186790. https://doi.org/10.1161/01.cir.0000027905.26586.e8
- Makkar R.R., Yoon S.-H., Leon M.B., Chakravarty T., Rinaldi M., Shah P.B., Skipper E.R., Thourani V.H., Babaliaros V., Cheng W., Trento A., Vemulapalli S., Kapadia S.R., Kodali S., Mack M.J., Tang G.H.L., Kaneko T. Association between transcatheter aortic valve replacement for bicuspid vs tricuspid aortic stenosis and mortality or stroke. JAMA. 2019;321(22):2193-2202. PMID: 31184741; PMCID: PMC6563564. https://doi.org/10.1001/jama.2019.7108
- Kim M.S., Bracken J., Eshuis P., Chen S.Y.J., Fullerton D., Cleveland J., Messenger J.C., Carroll J.D. Use of short roll C-arm computed tomography and fully automated 3D analysis tools to guide transcatheter aortic valve replacement. Int J Cardiovasc Imaging. 2016;32(7):1145-1152. PMID: 27091735. https://doi.org/10.1007/s10554-016-0886-0

