Published 2023-03-30
Keywords
- Adult,
- Case Report,
- Coronary Artery Disease,
- Heart Defects, Congenital,
- Heart Septal Defects, Atrial
How to Cite
Copyright (c) 2023 Podzolkov V.P., Minaev A.V., Chiaureli M.R., Cheban V.N., Golubev E.P., Petrosyan K.V., Sobolev A.V., Zemlyanskaya I.V.

This work is licensed under a Creative Commons Attribution 4.0 International License.
Abstract
Background: The relevance of coronary artery disease treatment in congenital heart disease is related to the increasing number of older patients with congenital conditions, predisposing factors and continuous silent ischemia.
Objective: To analyze clinical data and results of surgery in patients with a combination of congenital heart disease and hemodynamically significant coronary artery lesions.
Methods: 17 patients (7 women (41.2%), 10 men (58.8%)) were included in the study. All of them underwent myocardial revascularization and congenital heart disease corrective surgery from 2003 to 2020. The mean age at the time of surgery was 57.2 years. The congenital diagnosis was an atrial septal defect (14 patients), partial anomalous pulmonary vein connection (1 patient), recanalization of atrial septal defect (1 patient), recanalization of ventricular septal defect (1 patient). In 7 cases congenital and coronary pathology correction were performed percutaneously — coronary stenting as the first stage, defect closure at an interval of 4 to 10 days as the second. One patient underwent stenting 7 months prior to an open-heart surgery. In 9 cases one-staged open-heart surgery was performed simultaneously.
Results: At the hospital 1 patient died after surgery due to multiple organ dysfunction syndrome. In all other cases there were no symptoms of ischemia on discharge, the patients were in NYHA class I–II (New York Heart Association).
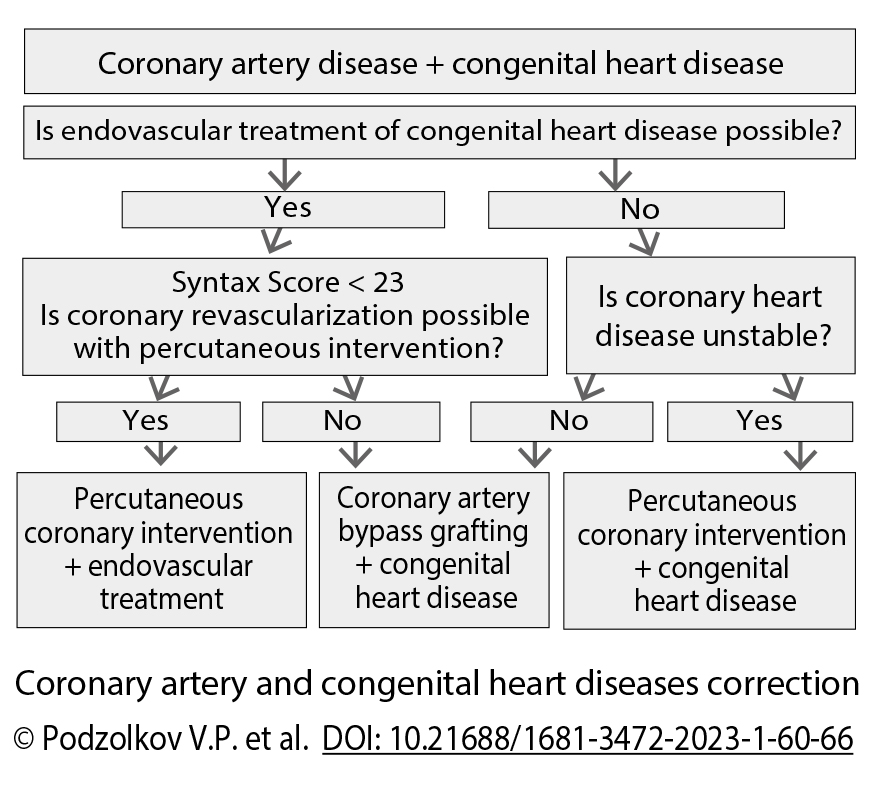
Conclusion: The tactics of coronary revascularization is determined by the necessity of percutaneous or open-heart intervention. Myocardial revascularization may be preferable as the first stage, or a one-stage correction may be performed and proved by good results.
Received 14 October 2022. Revised 25 November 2022. Accepted 27 November 2022.
Informed consent: The patient’s informed consent to use the records for medical purposes is obtained.
Funding: The study did not have sponsorship.
Conflict of interest: The authors declare no conflict of interest.
Contribution of the authors
Literature review: A.V. Minaev
Drafting the article: A.V. Minaev, A.V. Sobolev, I.V. Zemlyanskaya
Critical revision of the article: V.P. Podzolkov
Surgical treatment: M.R. Chiaureli, V.N. Cheban, E.P. Golubev, K.V. Petrosyan
Final approval of the version to be published: V.P. Podzolkov, A.V. Minaev, M.R. Chiaureli, V.N. Cheban, E.P. Golubev, K.V. Petrosyan, A.V. Sobolev, I.V. Zemlyanskaya
References
- Khan A., Gurvitz M. Epidemiology of ACHD: what has changed and what is changing? Prog Cardiovasc Dis. 2018;61(3-4):275-281. PMID: 30125582. https://doi.org/10.1016/j.pcad.2018.08.004
- Tutarel O., Kempny A., Alonso-Gonzalez R., Jabbour R., Li W., Uebing A., Dimopoulos K., Swan L., Gatzoulis M.A., Diller G.-P. Congenital heart disease beyond the age of 60: emergence of a new population with high resource utilization, high morbidity, and high mortality. Eur Heart J. 2014;35(11):725-732. PMID: 23882067. https://doi.org/10.1093/eurheartj/eht257
- Lin Y.-S., Liu P.-H., Wu L.-S., Chen Y.-M., Chang C.-J., Chu P.-H. Major adverse cardiovascular events in adult congenital heart disease: a population-based follow-up study from Taiwan. BMC Cardiovasc Disord. 2014;(14):38. PMID: 24655794; PMCID: PMC3994523. https://doi.org/10.1186/1471-2261-14-38
- Giannakoulas G., Dimopoulos K., Engel R., Goktekin O., Kucukdurmaz Z., Vatankulu M.A., Bedard E., Diller G.P., Papaphylactou M., Francis D.P., Di Mario C., Gatzoulis M.A. Burden of coronary artery disease in adults with congenital heart disease and its relation to congenital and traditional heart risk factors. Am J Cardiol. 2009;103(10):1445-1450. PMID: 19427444. https://doi.org/10.1016/j.amjcard.2009.01.353
- Benjamin E.J., Virani S.S., Callaway C.W., Chamberlain A.M., Chang A.R., Cheng S., Chiuve S.E., Cushman M., Delling F.N., Deo R., de Ferranti S.D., Ferguson J.F., Fornage M., Gillespie C., Isasi C.R., Jiménez M.C., Jordan L.C., Judd S.E., Lackland D., Lichtman J.H., Lisabeth L., Liu S., Longenecker C.T., Lutsey P.L., Mackey J.S., Matchar D.B., Matsushita K., Mussolino M.E., Nasir K., O'Flaherty M., Palaniappan L.P., Pandey A., Pandey D.K., Reeves M.J., Ritchey M.D., Rodriguez C.J., Roth G.A., Rosamond W.D., Sampson U.K.A., Satou G.M., Shah S.H., Spartano N.L., Tirschwell D.L., Tsao C.W., Voeks J.H., Willey J.Z., Wilkins J.T., Wu J.H., Alger H.M., Wong S.S., Muntner P.; American Heart Association Council on Epidemiology and Prevention Statistics Committee and Stroke Statistics Subcommittee. Heart disease and stroke statistics-2018 update: a report from the American Heart Association. Circulation. 2018;137(12):e67-e492. PMID: 29386200. https://doi.org/10.1161/CIR.0000000000000558
- Zomer A.C., Vaartjes I., Uiterwaal C.S.P., van der Velde E.T., Sieswerda G.-J.T., Wajon E.M.C., Plomp K., van Bergen P.F.M., Verheugt C.L., Krivka E., de Vries C.J., Lok D.J.A., Grobbee D.E., Mulder B.J.M. Social burden and lifestyle in adults with congenital heart disease. Am J Cardiol. 2012;109(11):1657-1663. PMID: 22444325. https://doi.org/10.1016/j.amjcard.2012.01.397
- Ghaderian M., Emami-Moghadam A.R., Ali Samir M., Amin Zadeh M., Saadi A.H. Lipid and glucose serum levels in children with congenital heart disease. J Tehran Heart Cent. 2014;9(1):20-26. PMID: 25561966; PMCID: PMC4277787.
- Martínez-Quintana E., Rodríguez-González F., Nieto-Lago V., Nóvoa F.J., López-Rios L., Riaño-Ruiz M. Serum glucose and lipid levels in adult congenital heart disease patients. Metabolism. 2010;59(11):1642-1648. PMID: 20423747. https://doi.org/10.1016/j.metabol.2010.03.014
- Duffels M.G., Mulder K.M., Trip M.D., de Groot E., Gort J., van Dijk A.P., Hoendermis E.S., Daliento L., Zwinderman A.H., Berger R.M., Mulder B.J. Atherosclerosis in patients with cyanotic congenital heart disease. Circ J. 2010;74(7):1436-1441. PMID: 20526039. https://doi.org/10.1253/circj.cj-09-0858
- Fyfe A., Perloff J.K., Niwa K., Child J.S., Miner P.D. Cyanotic congenital heart disease and coronary artery atherogenesis. Am J Cardiol. 2005;96(2):283-290. PMID: 16018858. https://doi.org/10.1016/j.amjcard.2005.03.060
- Tarp J.B., Sørgaard M.H., Christoffersen C., Jensen A.S., Sillesen H., Celermajer D., Eriksson P., Estensen M.E., Nagy E., Holstein-Rathlou N.H., Engstrøm T., Søndergaard L. Subclinical atherosclerosis in patients with cyanotic congenital heart disease. Int J Cardiol. 2019;277:97-103. PMID: 30228018. https://doi.org/10.1016/j.ijcard.2018.08.104
- Perloff J.K. The coronary circulation in cyanotic congenital heart disease. Int J Cardiol. 2004;97(Suppl 1):79-86. PMID: 15590083. https://doi.org/10.1016/j.ijcard.2004.08.018
- Abraham D., Freeman L.J., Lewis C., O'Sullivan M. Coronary artery disease in Eisenmenger's syndrome — Rare but not to be forgotten. Int J Cardiol. 2016;203:276-277. PMID: 26519685. https://doi.org/10.1016/j.ijcard.2015.10.148
- Häcker A.L., Oberhoffer R., Hager A., Ewert P., Müller J. Age-related cardiovascular risk in adult patients with congenital heart disease. Int J Cardiol. 2019;277:90-96. PMID: 30262228. https://doi.org/10.1016/j.ijcard.2018.09.042
- Jokinen E. Coronary artery disease in patients with congenital heart defects. J Intern Med. 2020;288(4):383-389. PMID: 32391638. https://doi.org/10.1111/joim.13080
- Иоселиани Д.Г., Колединский А.Г., Ковальчук И.А., Абильдинова А.Ж. Рентгенэндоваскулярная реваскуляризация миокарда и закрытие вторичного дефекта межпредсердной перегородки: одномоментно или раздельно? Грудная и сердечно-сосудистая хирургия. 2013;(5):72-76. Ioseliani D.G., Koledinsky A.G., Kovalchuk I.A., Abildinova A.Zh. Endovascular revascularization and closing of secondary atrial septal defect: simultaneously or separately? Russian Journal of Thoracic and Cardiovascular Surgery. 2013;(5):72-76. (In Russ.)
- Подзолков В.П., Алекян Б.Г., Чиаурели М.Р., Мерзляков В.Ю., Зеленикин М.М., Нежлукто А.А., Абдулкасумова С.К. Хирургическое лечение врожденных пороков сердца в сочетании с ишемической болезнью сердца. Грудная и сердечно-сосудистая хирургия. 2009;(3):4-6. Podzolkov V.P., Alekyan B.G., Chiaureli M.R., Merzlyakov V.Yu., Zelenikin M.M., Nezhlukto A.A., Abdulkasumova S.K. Surgical treatment for congenital heart disease concurrent with ischemic heart disease. Russian Journal of Thoracic and Cardiovascular Surgery. 2009;(3):4-6. (In Russ.)

